A former nurse said the NHS is “unrecognisable” from the institution she left twenty years ago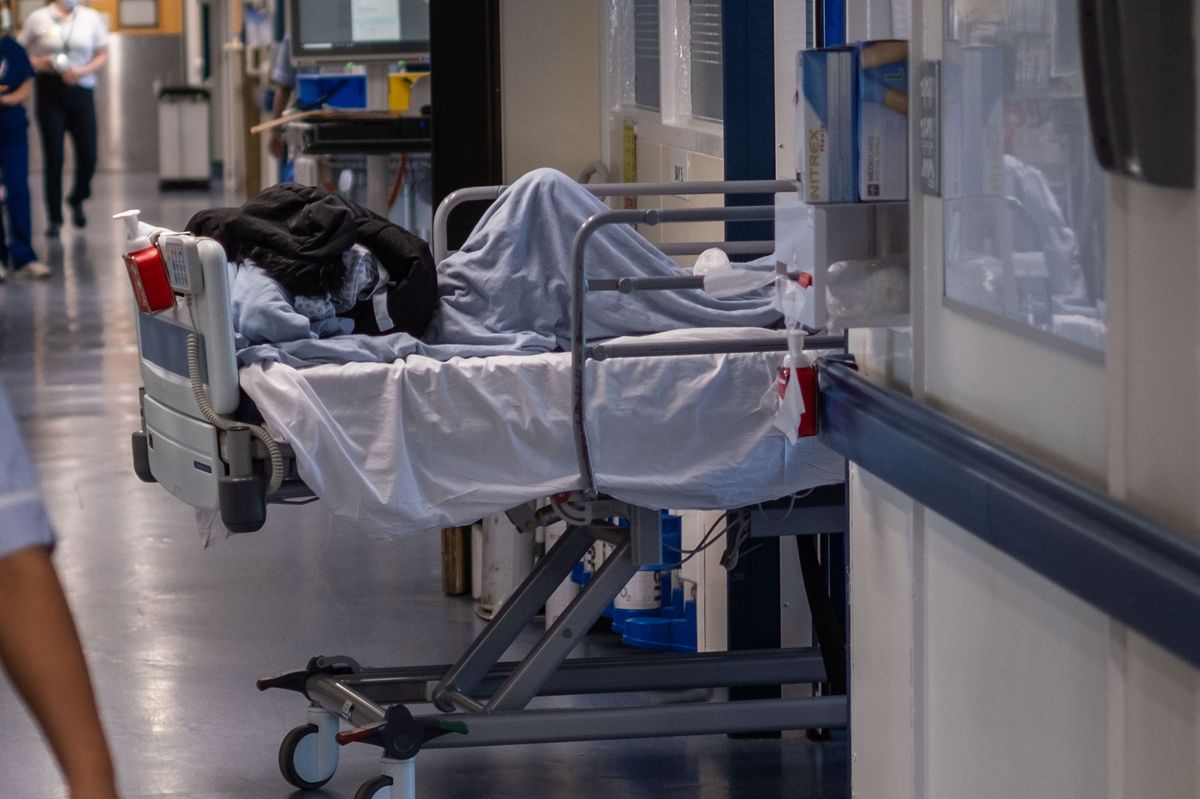
3,109 patients waited more than 12 hours at Merseyside’s A&Es last month. (Image: PA)
More than 3,000 people waited more than 12 hours in Merseyside A&Es last month. The figures have risen more than 16,000% in just five years, with just 19 people waiting more than 12 hours at the region’s emergency departments in January 2021.
Ten years ago, in January 2016, no patient waited more than 12 hours to be seen at any of Merseyside’s A&E departments. Numbers skyrocketed between January 2022 and January 2023, when numbers jumped from 210 to 2,038 patients waiting more than 12 hours in A&E.
Figures have remained above 2,000 each January since. Last month, 3,109 patients were forced to wait more than 12 hours from decision to admit to admission at Merseyside’s A&Es.
NHS Cheshire and Merseyside, the body that oversees the region’s hospital trusts, pointed to rising demand as a cause for long waits, saying that the NHS is experiencing its busiest winter on record. The board said it was working hard to reduce the use of corridor care.
Former nurse Irene Jenkins, 80, waited so long at the Royal Liverpool Hospital‘s emergency department last month that she took her sick husband Alan, 81, home. Alan is suffering with kidney failure.
Irene, from Huyton, spent four decades working as a nurse at Whiston Hospital. She said the NHS of today is “unrecognisable” from the one she left 20 years ago, saying she was left “absolutely disgusted” by Alan’s treatment at the Royal.
Irene took Alan to hospital on January 29 after seeing his hands and face swell-up, saying “I knew he wasn’t well at all”. Of the Royal A&E, she said: “Ambulances were bringing people in wheelchairs and just leaving them in the A&E department. They were in terrible pain and nobody was taking notice.
“There was a woman brought in by ambulance who was on her own. She vomited into a receiver. A member of staff took the receiver from her and threw it in the public bin by the doors instead of taking it to the sluice. Then the lady vomited on the floor because nobody gave her another receiver. When the vomit on the floor was reported, they slapped an incontinence pad over it without any hazard signs. About 15 minutes later, someone cleaned it up and threw it in the bin by the door. I was mortified.”
Alan and Irene waited from 11.30am to 5pm, during which time Alan was triaged and was told he needed care on the nephrology ward. With no movement by 5pm, Irene took Alan home, and then received a call from the nephrology ward asking them to return to A&E, and saying that a bed would be ready by 10pm.
The pair arrived back at A&E at 9pm. They remained there at 3.30am. Irene said: “A nurse then gave us two options: sleep in a chair until 8am or go home and go straight onto a ward the following morning. I told them he wasn’t sleeping in a chair at nearly 81 years old.”
Alan was eventually admitted onto the ward on January 31. Irene added: “The A&E is not fit for purpose. It made Alan feel useless.
“The trouble starts from the GPs. People go to A&E with the sniffles because they can’t get an appointment. It’s a systemic, knock-on effect. I feel so sorry for the people who don’t know any different because they’ve never worked in a hospital.”
A spokesperson for The Royal Liverpool University Hospital, said: “We apologise that Mr Jenkins’ experience did not meet the standards we strive for.
“Demand for urgent and emergency care continues to place significant pressure on our services, and we are working hard to improve patient flow, reduce waiting times, and strengthen the overall experience for patients. We recognise that there were some communication issues during Mr Jenkin’s time in our care and we are looking into this further.”
In recent weeks, the ECHO has reported on long waits and pressures at local hospitals. Last week, we reported on Christopher Birch, who spent 50 hours on a trolley in the Royal’s A&E department, and shared video from that same department showing patients on trolleys lining a corridor for its full length.
Earlier this month, the ECHO told how Arrowe Park Hospital on the Wirral was in crisis as patients on trolleys lined corridors and ambulances queued up outside carrying sick and ill people. And in January, the ECHO revealed an elderly woman had died alone on a trolley in a corridor with exhausted staff unable to care for her.
A spokesperson for NHS Cheshire and Merseyside said: “Accident and Emergency Departments in our local hospitals and nationally have experienced rising demand for a number of years and the NHS has just experienced its busiest winter on record.
“Despite teams working incredibly hard in very difficult circumstances, this does mean that some patients are cared for by doctors and nurses in corridors and patients are still experiencing very long waits in our emergency departments and long waits to be admitted to hospital.
“Providing care in corridors is not what we want for our patients, and we are working hard to reduce the use of corridor care. New standards are being developed nationally to reduce long waits and corridor care, and we’ll be working to ensure these are implemented locally.
“We continue to work closely with local health and social care partners across Cheshire and Merseyside and have initiatives in place such as Urgent Community Response and virtual wards, to help prevent avoidable hospital admissions and treat more people in the community. This in turn helps to reduce A&E pressures and long waits.
“The public can help by remembering that busy hospital A&E departments should only be used for life-threatening illnesses and injuries. People should continue to call 999 in emergency situations, but for conditions which are less urgent, please use NHS 111. The service can assess and direct to the most appropriate local service, including urgent treatment centres, GP practices, and consultations with a pharmacist. It is available 24/7 online at 111.nhs.uk, on the NHS App and by calling 111.”
A Department of Health and Social Care spokesperson said: “Nobody should have to wait this long in A&E. That’s why we started preparing for winter earlier than ever before – boosting capacity, supporting staff, and strengthening urgent and emergency care services.
“As a result, A&E treatment times have been faster this winter for the majority of people – even as staff faced record demand – but we know there is more to do to cut the longest waits. A&E waiting times have been worsening over the last decade. We have begun to turn the tide, but there’s a long way to go.”
Do you have a information, a tip or a story? Contact jon.blackburn@liverpoolecho.co.uk
Ensure our latest news and what’s on headlines always appear at the top of your Google search by making us a preferred source. Click here to activate or add us as a preferred source in your Google search settings.

