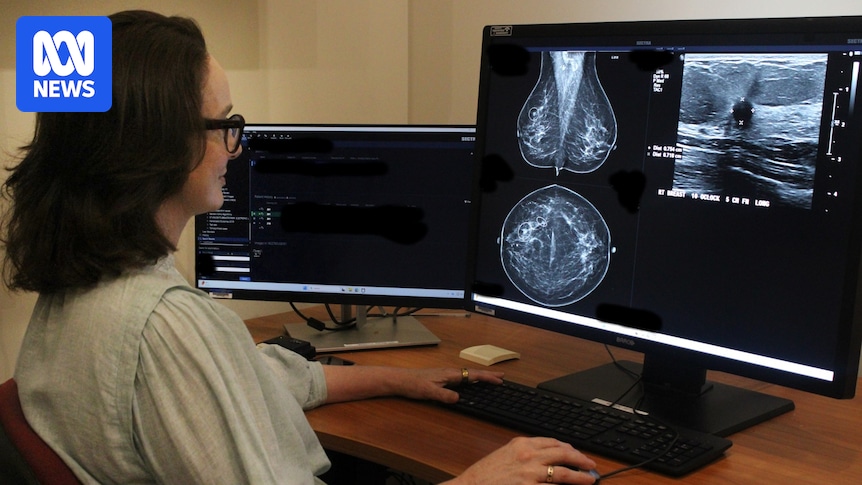
An Australian-made artificial intelligence tool can detect women with a high likelihood of breast cancer who were otherwise missed in normal screening, according to new research.
The AI tool identified women that were at the same or greater risk of breast cancer as those with the deadly BRCA gene mutations.
The study, published in the Lancet Digital Health journal, found the tool could pick up risk factors humans could not see and was more accurate than current methods for determining risk.
Unlike a radiologist, who either finds cancer or not, the AI tool gives a personalised risk score between 0 and 99.9 that predicts the woman’s likelihood of having breast cancer at any time over the next four years.
The study found one in 10 women who were in the top 2 per cent of risk scores went on to develop breast cancer, even though their mammograms were all clear.
“I think it’s a breakthrough discovery that the algorithm was able to identify signals for risk and/or early cancer that the human eyes weren’t able to perceive,” said lead researcher Helen Frazer, the clinical director at St Vincent’s BreastScreen.

Dr Helen Frazer has been working on this technology for 10 years. (ABC News: Paige Cockburn)
“Ninety thousand Australian women are forecast to die from breast cancer in the next 25 years and we need to change that,” Dr Frazer said.
The algorithm, called BRAIx, was developed using data from nearly half a million mammograms of Australian women from 2016 to 2017 and then bolstered with an independent dataset of around 4,500 women in Sweden.
The Lancet Digital Health study found it was better at detecting risk than tools relying on other established risk factors such as age, family history and breast density score.
Women with dense breast tissue are at higher risk of developing cancer but it can be particularly difficult to detect as dense tissue and cancer both appear white on a mammogram. Despite that, the AI could tell them apart, Dr Frazer said.
“The algorithm learns density and it’s not confused or confounded by it … and it’s operating at a pixel level whereas the resolution of the human eye is far more limited than that.”
‘I say bring it on’
Jess Armstrong is a cancer survivor who was diagnosed with stage 2 breast cancer in 2023 after finding a pea-size lump under her armpit.
She is excited by the AI and believes it could reduce some of the fear and anxiety that comes with having a mammogram deciphered.

Jess Armstrong said she would be comfortable having AI used as part of her ongoing monitoring. (Supplied: Fuca)
“I say bring it on because hospital systems are under a lot of pressure, human error can happen … there’s grey areas and opinions,” she said.
“But this AI tool can lay out the facts and give you a score … so it will reduce wait times and tell you whether you need to go forward with more scans.”
Ms Armstrong was under the age of 40 when she was diagnosed, which meant she was not eligible for free mammograms through the national screening program.
She said earlier screening was essential and AI could make that a reality.
“We don’t have the resources to test everyone but with AI it’s cheaper and more efficient, so we could widen that net to a younger group.”
Dr Frazer believes the long-term goal of zero deaths from breast cancer is possible with artificial intelligence, especially if screening starts at age 40 or younger.
She said while population screening had reduced breast cancer by as much as 50 per cent in women aged 50 to 74, it still largely followed a “one-size-fits-all” approach.
Dr Frazer said it was the cases missed by mammograms that motivated her to spend 10 years developing the AI.
“The hardest part of the job is sitting opposite a woman who says ‘breast screening failed to detect my cancer, please explain’,” she said.
The AI is particularly good at identifying those with the most elevated risk levels.
Women determined by the tool as being in the top 2 per cent of risk had the same or greater likelihood of developing cancer than women with BRCA1 and BRCA2 gene mutations.

Dr Wendy Ingman said she was excited about the capabilities of the AI tool. (Supplied: Australian Breast Cancer Research)
The research is a game changer, according to Adelaide University breast health researcher Wendy Ingman, who was not involved in the study.
“There are other AI algorithms around the world that are finding that they can predict breast cancer risk, but I think this one is probably the one that’s gone the furthest in actually defining what that level of risk is,” she said.
“I’m pretty excited about the ability of this AI algorithm to detect something in the mammogram which is able to give a prediction of who will get breast cancer in the next four years.”
Women express trust in AI
This AI tool could support the Australian radiology workforce, which is experiencing shortages amid growing demand from an aging population.
It gives almost immediate results and could reduce overall system costs, as women at low risk will be able to dial back their screening, according to the researchers.
However, the AI is not perfect and does not have human context so a radiologist must always have the ultimate oversight.
The researchers ran a small focus group to find out how women felt about using artificial intelligence in breast screening. They found most were open to it if humans were involved and believed it could be just as accurate as a radiologist.
Chinese women get breast cancer younger
The Breast Cancer Network Australia’s director of policy and advocacy Vicki Durston said the research was a timely reminder that screening must keep pace with science.
“AI is not the whole answer, but the emerging evidence shows real potential to strengthen how we understand risk and support earlier detection for every woman.”
The tool was a collaborative effort by researchers from a range of institutions including St Vincent’s BreastScreen Melbourne, The University of Adelaide and The University of Melbourne and received around $5 million from the federal government’s Medical Research Future Fund.
The researchers are now planning a smaller prospective study to assess women’s mammograms in real time. They believe the tool will be ready to roll out in five years.