A serious outbreak of measles in Asia has fuelled a surge in cases in NSW — but what concerns health authorities most are signs the highly infectious disease is spreading undetected in the community.
In the first three months of the year, the state recorded 38 cases of measles, five of which have no known infection source.
Vicky Sheppeard, director of South Eastern Sydney Local Health District’s Public Health Unit, said the majority of cases were linked to returned travellers from south-east Asian countries.
However, Dr Sheppeard said the five infections identified between January 1 to March 7 cannot be traced back to exposure sites or overseas travel, which may indicate the virus was being locally transmitted.
“That is of concern because there must have been undetected cases,” Dr Sheppeard said.
“In order to prevent an outbreak, we need to identify all cases and make sure that all their contacts are followed up.”
Dr Sheppeard says unknown infection sources are a cause for concern to health authorities. (ABC News: Monish Nand)
Measles, which can cause a fever, cough and a characteristic rash that spreads to the whole body, is a potentially fatal but vaccine-preventable disease.
Severe complications can lead to middle-ear infections, diarrhoea and pneumonia.
In rare cases, patients can develop a fatal, progressive brain disease known as subacute sclerosing panencephalitis.
Rise linked to overseas travel
Dr Sheppeard said cases usually increased in the first few months of the year as travellers returned from overseas.
She said infections for 2026 had risen compared to the number of cases in previous years, as south-east Asian countries like Indonesia, Vietnam and the Philippines experienced significant outbreaks since the COVID-19 pandemic.
“Australians love to travel to south-east Asia and do that frequently, particularly over the summer period,” Dr Sheppeard said.
She said cases were detected among Australians in their 20s and 40s, likely due to a change in the vaccine schedule dose and less vigorous childhood immunisation protocols.
A first dose of measles-mumps-rubella (MMR) vaccine was recommended at 12 months of age and a second at 18 months.

A majority of measles cases have been linked to travel in south-east Asia in countries like Indonesia, Vietnam and the Philippines. (ABC News: Abbey Haberecht)
In January, the Australian Technical Advisory Group on Immunisation updated its advice to recommend an additional dose for infants aged six to 11 months when travelling overseas.
“In Australia, we’re really lucky we have had a long-standing national immunisation program that funds our vaccines,” Dr Sheppeard said.
“We’ve got a strong public health sector, we have Medicare and we have a national register, so that has enabled us to really maximise our coverage.”
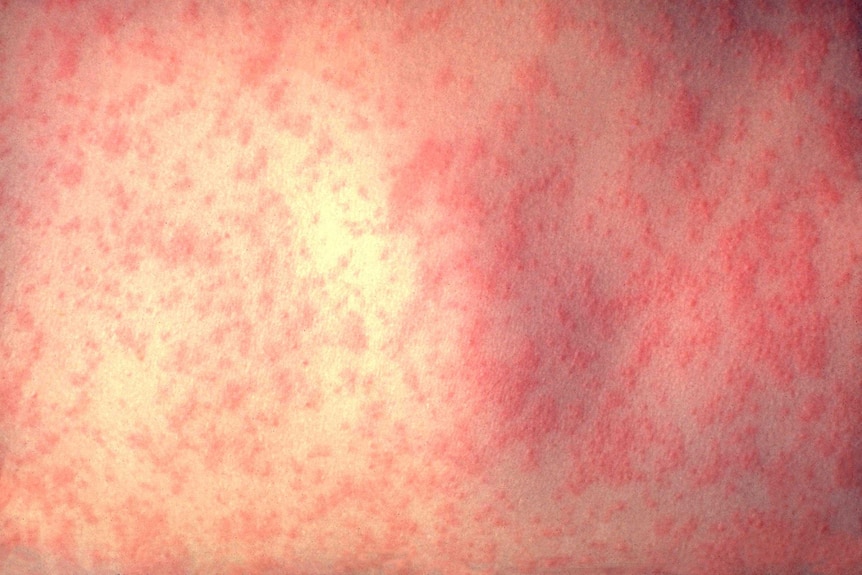
Measles is a highly contagious disease, which can cause a fever, cough and rash. (Centres for Disease Control)
Could Australia lose its measles-free status?
The World Health Organisation declared Australia had eliminated measles endemically in 2014.
But in recent years, dozens of countries including the United Kingdom, Spain and Canada have lost their elimination status amid uncontrolled outbreaks and lagging vaccination rates.
Is Australia about to see the return of endemic measles?
The United States — which first achieved elimination status in 2000 — is now on track to lose its status with outbreaks identified across more than 40 states.
Deakin University epidemiology chair Catherine Bennett said Australia did not have the level of local transmission compared to America and south-east Asian countries.
However, Professor Bennett said if vaccination rates remained low and people failed to respond to the outbreaks occurring overseas, it was “quite possible” Australia could also lose its status.
“If [cases] are all imported that’s telling us about endemic disease in other parts of the world that haven’t eliminated it,” she said.
“But if we have enough unvaccinated people and enough secondary cases in Australia particularly, that then start passing it on to other people — then it changes the whole dynamic,” she said.

Catherine Bennett says America is experiencing “local explosions” of the measles virus. (Supplied)
Professor Bennett said America was an example where “local explosions” were occurring not just as a result of geography, but due to religious and cultural views on vaccination.
“If measles gets into part of the community where it starts to spread because there’s enough susceptible people who aren’t vaccinated or haven’t had a prior infection, then that’s when local transmission starts to take off,” she said.
“It’s a disease that, thankfully has a relatively low fatality rate, but the most fatalities occur in children.”
Best defence an ‘effective vaccination regime’
To achieve herd immunity, vaccine coverage is required for 92–94 per cent of the population, according to the Department of Health.
The National Centre for Immunisation Research and Surveillance found coverage of the first dose of MMR vaccine in children at 24 months of age decreased by 0.4 of a percentage point from 2022 to 2023.
Terry Slevin, chief executive of the Public Health Association of Australia, said measles was “the canary in the coal mine” in terms of infectious diseases.

Terry Slevin says Australia’s vaccination rates are slowly declining. (ABC News: Harry Frost)
Adjunct Professor Slevin said Australia’s vaccination rates were typically high, but were slowly declining below the nation’s target level of 95 per cent.
“We know measles is a highly infectious disease and ultimately our best defence is a very, very effective vaccination regime,” he said.
“In most cohorts, we have in excess of 90 per cent take-up, it’s slightly coming off from the target.”
Adjunct Professor Slevin said it was virtually impossible to keep out travel-related infections, as measles was mostly asymptomatic in its early stages.
“Australians travelling overseas or people coming from overseas into Australia, and bringing the infection with them — ultimately it comes down to issues relating to regions around the world having varying levels of vaccination,” he said.
“I don’t think there’s reason to be concerned about our disease-free status being removed as long as we respond to these challenges sensibly and continue to reinforce the importance and value of vaccination in Australia.”