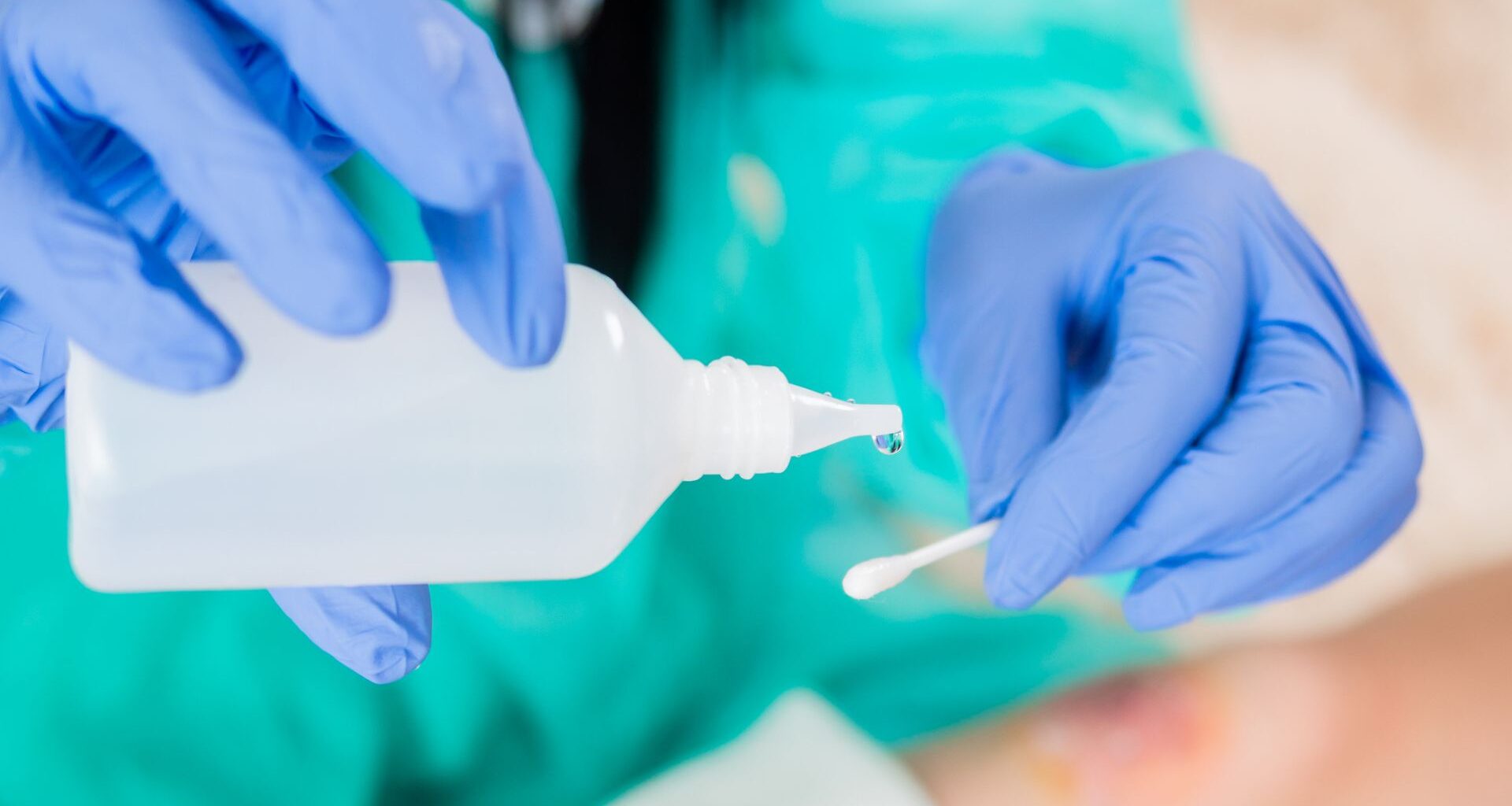
A common antiseptic used to clean hospital patients’ skin can linger on surfaces for hours, creating breeding grounds for bacteria to become tolerant, or even gain resistance, to chemicals that usually kill them.
Once they develop “tolerance,” bacteria can survive certain concentrations of chemicals more easily than their peers do, but they can still be killed by the doses of antiseptics typically used for cleaning. Antiseptics include chemicals, such as alcohol, iodine or hydrogen peroxide, that are used to disinfect surfaces or the skin. “Resistance” is a greater concern because it enables bacteria to grow even when exposed to concentrations of an antiseptic that would typically kill them.
According to a study published April 2 in the journal Environmental Science & Technology, as they learn to tolerate faint traces of antiseptics, bacteria might be swapping bits of DNA with each other. That same DNA might also help them dodge drugs designed to treat bacterial infections — namely antibiotics.
You may like
The study adds to a growing body of research mapping the hidden environmental stressors that can encourage bacteria to evolve these tolerance and resistance genes.
“Antimicrobial resistance comes from a lot of different places,” said lead author Erica Hartmann, a professor of civil and environmental engineering at Northwestern’s McCormick School of Engineering. “To really tackle the problem, we need antimicrobial stewardship, responsible use in agriculture, and we need to think about responsible use of chemicals in other environments, as well,” she told Live Science.
Practicing stewardship means using antimicrobial agents like antibiotics and antiseptics sparingly in order to prevent bacteria from evolving tolerance or resistance.
Tolerant bacteria travel by air
In the study, Hartmann and her colleagues tracked bacteria with tolerance to chlorhexidine, a commonly used chemical applied to patients’ skins before surgery or catheter insertion. They searched for these bacteria in an intensive care unit in an Illinois medical center.
Researchers swabbed 219 samples from bedrails, nurse call buttons, door sills, keyboards, light switches, and sink drains in six locations around the ICU in 2018. The rooms were quite clean, they found, but they were able to isolate about 1,400 bacteria and they found that 36% showed some tolerance to chlorhexidine.
In the lab, the researchers applied chlorhexidine to common materials — plastic, metal and laminate — and then tracked how long the antiseptic lingered on the surfaces, including after they cleaned the materials with water and other chemical cleaners. They found that, even after cleaning, traces of the antiseptic persisted on surfaces for at least 24 hours.
These lingering traces weren’t strong enough to kill bacteria. But these types of microenvironments, in which bacteria are exposed to non-lethal doses of a chemical that usually kills them, always raise alarm bells.
What to read next
In these settings, the bacteria that thrive are those that carry genes that help them survive the chemical’s effects. These tolerant bacteria outcompete those that lack tolerance genes and thus grow more abundant. The worst case scenario would be that bacteria become so used to fighting off a chemical — and so good at it — that they become resistant to its effects.
The team found chlorhexidine-tolerant bacteria throughout the hospital rooms, even though the antiseptic was applied only to patients’ skin. The sink emerged as a hotspot for these bacteria.
Hospital sinks have become a focus for those studying antimicrobial resistance in recent decades. Bacteria love the humid, warm U-bends found in sinks, and they will do what they can to stay there, even if they are exposed to watered-down chemicals that get washed down the drain. This creates a perfect environment for tolerance and resistance to emerge.
Sinks can also spread bacteria by generating aerosols, or tiny particles that can float through the air; as water leaves the tap, hits standing water, or splashes against the drain, these particles can fly through the air. The researchers’ swabs showed that tolerant strains could be found on door sills, suggesting they traveled through the air and settled up there.

The sink emerged as a hotspot for antiseptic residues. (Image credit: MCT via Getty Images)Antiseptics still work really well
Some of the antiseptic-resistant bacteria carried a plasmid — a small DNA loop that can be transferred between bacteria — that not only helped them tolerate chlorhexidine but could also help them resist antibiotics, such as carbapenems. This type of gene transfer is a well known way that bacteria gain resistance to antimicrobials, and it can take place between bacteria of totally different species.
That is “really quite important,” said Danna Gifford, a lecturer in antimicrobial resistance at the University of Manchester in the U.K., who wasn’t involved in the study. This finding suggests that antibiotic resistance could be accelerated “without the use of antibiotics,” she said, driven by antiseptic exposure alone.
But let’s be clear: chlorhexidine is still highly effective at killing germs. The bacteria observed in the study could only survive very low concentrations of the chemical, far below the amounts used to clean patients’ skin.
“I don’t think that this supports a really conservative approach” to using chlorhexidine, said Gifford, adding that limiting the antiseptic’s use in high-risk settings like ICUs, without proper clinical evidence, could put vulnerable patients at risk of infections. But this work, alongside other recent research, still raises the question of whether we need to be more cautious about our use of antiseptics, Hartmann and Gifford agreed.
Further studies should look into whether these effects can be seen in other settings — for instance, in the home or in veterinary clinics — to better understand how these antiseptic residues affect bacteria, the study authors wrote.
Whether we should be reserving antiseptics for “high-risk situations” is “probably worth more investigation,” said Gifford. Often for household cleaning, “plain soap and water are more than sufficient for our cleaning and hygiene,” Hartmann noted, so that might be a setting where antiseptic use can be reduced.
In the meantime, “we are running out of antibiotics that work effectively,” she said. “We are not quite fully there yet, but if we don’t intervene in the things that we do now, we’re going to end up in a situation in the future where we can’t do simple things like treat dental infections or do surgery because we can’t then give patients antibiotics after treatment.”
This article is for informational purposes only and is not meant to offer medical advice.
Shen, J., Weng, Y., Shimada, T., Karan, M., Watson, A., Medernach, R. L., Young, V. B., Hayden, M. K., & Hartmann, E. M. (2026). Hospital environments harbor Chlorhexidine-Tolerant bacteria potentially linked to chlorhexidine persistence in the environment. Environmental Science & Technology. https://doi.org/10.1021/acs.est.5c18587