February 27, 2026 — 5:00am
Save
You have reached your maximum number of saved items.
Remove items from your saved list to add more.
Save this article for later
Add articles to your saved list and come back to them anytime.
Got it
AAA
It was a friend who first mentioned the disorder to Stacey Anderson.
“We worked together, and she noticed I went to the bathroom a lot,” Anderson, now 41, says. “She’d noticed that I talked about my appearance quite often, but in a way that sought constant reassurance. And that I also spent a lot of money on skincare.”
In isolation, none of these things would seem particularly weird. But when Anderson was going to the bathroom, it was to look at herself in the mirror, which would continue almost constantly throughout the day.
 Stacey Anderson was diagnosed with body dysmorphic disorder when she was 28. Simon Schluter
Stacey Anderson was diagnosed with body dysmorphic disorder when she was 28. Simon Schluter
“It wouldn’t just have to be the toilet: it could be the mirror in my car, or the camera on my phone,” says Anderson, who admits it’s difficult to put an exact number on how many times a day she was checking her own reflection, or picking at her skin or looking at skincare products online that might help what she saw in the mirror.
“But I think it was eight hours a day,” she says.
Anderson’s friend told her she might have body dysmorphic disorder (BDD) and a few months later, at age 28, she was officially diagnosed.
What is facial dysmorphia?
Distinct from eating disorders or body image concerns, under the DSM-5 (the standard tool used by clinicians and researchers to classify and diagnose mental disorders), BDD is a mental health condition that sits in the class of obsessive compulsive disorder, describing a preoccupation or obsession with a perceived defect or flaw in physical appearance that may be only slight to others, or may not even be observable.
Facial dysmorphia is an unofficial offshoot of BDD.
“Facial concerns are often the focus of the concern in BDD,” says Professor Gemma Sharp from the School of Psychology at Adelaide University. “Because that’s our window to the soul, isn’t it?”
Sharp says the key distinction between those who have standard body image issues and people with BDD is that for the latter, their condition makes participating in everyday life almost impossible. One of Sharp’s patients refused to leave their bedroom or be seen by their family.
From looking at them, it would be impossible to determine if someone has BDD, but that’s what makes this a mental disorder – it’s really not about what they actually look like at all. They will become obsessed with a particular element of their appearance and be able to think of little else; it could be the back of their knees, or the asymmetry of their face.
Says 33-year-old model and creative consultant Mahalia Handley, who was diagnosed with BDD four years ago: “It’s like having a record on in the back of your head constantly that’s telling you to focus on one thing, and it’s never really the things that people think you’re going to focus on.”
For Anderson, BDD manifested as a fixation on looking in the mirror. “I would just be in a trance-like state, and I could be there, it would feel like minutes, but it would be much, much longer,” she says. Things reached breaking point when the fixation compromised her relationship at the time.
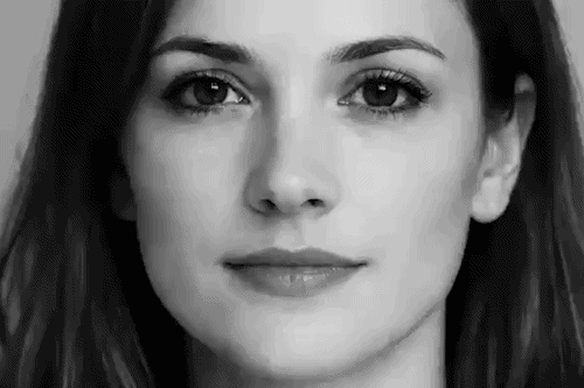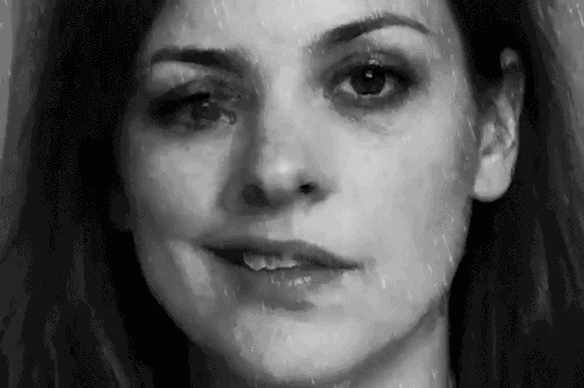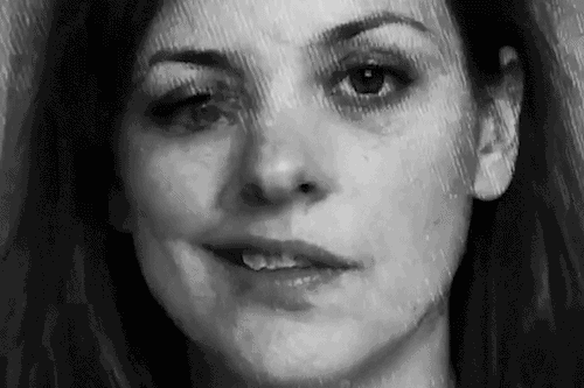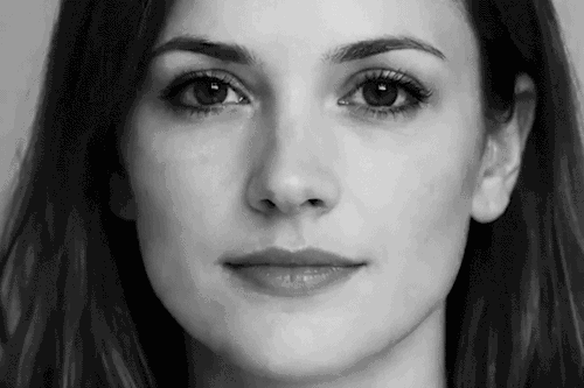 Facial dysmorphia describes the unsettling feeling that what you see in photos doesn’t match the image you have of yourself in your head.Tom CompagnoniThe influence of social media
Facial dysmorphia describes the unsettling feeling that what you see in photos doesn’t match the image you have of yourself in your head.Tom CompagnoniThe influence of social media
We encounter opportunities to look at ourselves many times a day, whether it’s at the gym or during a video call while working from home. And social media has compounded this obsession with ourselves by encouraging self-documentation.
On TikTok, there are now thousands of videos with the hashtags #facedysmorphia and #facialdysmorphia showing people lament the disconnect between what they think they look like, and what they see in photos or their reflection. This isn’t shocking considering 40 per cent of Australians report being dissatisfied with their appearance. But it’s important to make the distinction between not liking what you see in photos – which is a common body image concern – and having diagnosed BDD.
It’s hard to say how many people making social media videos about their so-called facial dysmorphia actually have the condition, but for Handley, it’s an inevitable consequence of our image-based culture.
“When there’s so much saturation of who we are and what we’re supposed to look like online, and that’s constantly changing due to trends, I think it’s natural we’d start to lose our understanding of self,” she says.
It’s a problem probably exacerbated by filters such as the “inverted face”, which are allegedly designed to show you “what you really look like”.
A few years ago, a similar phenomenon was given the name “Snapchat dysmorphia” to describe the effect beauty filters were having on our distorted sense of self, and in 2021 a study into the “Zoom Effect”, published in the Aesthetic Surgery Journal, found more than a third of the 335 participants identified new image concerns while on video calls.
AI isn’t helping, either. Dr Toni Pikoos, a co-author of the Zoom Effect study and a psychologist who has been researching BDD for more than a decade, says it’s become a big problem for her clients. “They’ll upload pictures of themselves to AI and ask it, “Rate my appearance. What do I need to fix about myself? Show me how I could change if I get this surgery,’” Pikoos says.
Cosmetic surgery as a solution
The tricky thing about a condition like BDD is that people confuse it with being an issue of vanity. “Particularly because treatment is often sought at the cosmetic clinic,” Sharp, of Adelaide University, says.
In a 2023 review into the prevalence of BDD in different settings, researchers found that in cosmetic or dermatology settings, 20 per cent of people had the condition. That’s an increase on an oft-cited 1998 study that estimated 7 per cent to 15 per cent of aesthetic patients displayed BDD symptoms.
Mahalia Handley says that at one point her BDD led her to consider getting surgery that would elongate her legs. “They smash the bones of your legs perfectly and then they elongate it by inserting metal. I was that fixated on my knees and my legs that I was close to going in and doing it,” she says.
 Model Mahalia Handley believes the obsession online with self-documentation is exacerbating the problem. Mahalia Handley
Model Mahalia Handley believes the obsession online with self-documentation is exacerbating the problem. Mahalia Handley
In July 2023, the Australian Health Practitioner Regulation Agency and the Medical Board of Australia made it a requirement for cosmetic surgeons to use a validated psychological screening tool to assess patients for BDD and suitability for treatment. But many doctors, including cosmetic and vascular physician Dr Keturah Hoffman, believe it’s ineffectual.
“It’s not going to help anybody know anything,” says Hoffman. “The first question is, ‘Are you unhappy with your appearance?’ If you answer no to that, what are you doing in my office?”
She believes BDD patients who are determined to get work done will find a way to go undetected by the screening questions. “Clever people with BDD can get around them,” she points out, saying that in order for cosmetic practitioners to be able to properly identify someone with BDD, the most important thing is that they have a relationship with them that can assist in reaching a proper diagnosis. “The current law has started down the right path, but it needs to be further developed,” Hoffman says.
Even if they are successful in getting work they want done, it’s common for BDD patients to be dissatisfied with the outcome, or they’ll find another part of themselves to fixate on.
“That focus of the appearance flaw can move around the body and sometimes [getting work done] makes people feel worse rather than better,” Sharp says.
Handley says her own obsessions have never stayed static. “There were points when my face was just ripped up from picking at it so badly, I felt like I couldn’t go outside. And other times, all I could concentrate on was fixing my neck, which, I’m like, there’s literally nothing wrong with my neck,” she says.
Pikoos notes that in treating her BDD clients, she finds it useful to frame the condition as “a disorder of attention”.
“The more attention we pay to the way that we look, the more we look at ourselves in the mirror, the more time we spend trying to fix or perfect ourselves, the more worried we become,” she says. “So a lot of the time with treatment, the goal is to reduce the amount of time you spend taking photos, reduce the amount of time you spend looking in the mirror. Exposure therapy is a big part of it as well.”
Stacey Anderson thinks more awareness is needed around the disorder and that the effect of diagnosis and therapy is immense. “I really wish I could have done something like this many, many years ago because my life could have been a lot different.”
Make the most of your health, relationships, fitness and nutrition with our Live Well newsletter. Get it in your inbox every Monday.
Save
You have reached your maximum number of saved items.
Remove items from your saved list to add more.
Default avatarCourtney Thompson is a Lifestyle Reporter at the Sydney Morning Herald and The Age.From our partners



