 The modified laser cuts on a bovine femur. Credit: University of Basel, Catherine Weyer
The modified laser cuts on a bovine femur. Credit: University of Basel, Catherine Weyer
Conventional orthopedic surgery relies heavily on mechanical tools like saws, chisels, and drills to cut bone. While these instruments are reliable, they generate significant friction and mechanical stress, which can damage surrounding tissue and prolong a patient’s recovery.
Seeking a gentler alternative, medical engineers have long explored laser technology. Because lasers operate without physical contact, they eliminate mechanical pressure and minimize the risk of bone microcracks. This level of precision is ideal for specialized procedures, such as inserting highly customized, 3D-printed joint implants.
However, adapting lasers for hard tissue has proven difficult. While surgical lasers effectively cut soft tissue, penetrating dense bone remains a significant challenge.
Until recently, laser osteotomy could only achieve shallow cuts of up to 3 centimeters. This depth falls critically short for major orthopedic procedures like a total knee arthroplasty, which requires planar cuts roughly 6 centimeters deep.
Flattening the Beam
The limitation isn’t simply a matter of power. “Increasing the energy of the laser beam would not be a good solution. This could char the bone and have a negative impact on the healing process,” explains Dr. Ferda Canbaz from the University of Basel.
Instead of turning up the dial, the team changed the fundamental shape of the laser. Traditional surgical lasers, such as the Er:YAG, are most intense at the center and fade toward the edges, much like a standard flashlight. When this uneven beam cuts into bone, it carves a V-shaped trench.
As that cut deepens, the V-shaped geometry causes the beam to lose its focus and energy density. This acts like an optical funnel, eventually choking off the beam’s energy completely.
To bypass this barrier, the researchers flattened the beam into a uniform “top hat” profile. This redesigned beam spreads its energy evenly across its entire width before dropping off sharply at the edges.
×
Thank you! One more thing…
Please check your inbox and confirm your subscription.
“Because the energy is transmitted more evenly, the laser cuts more efficiently and faster,” says doctoral student and lead author Mingyi Liu. By maintaining a flat bottom, the laser ablates straight down, preventing the trench walls from sapping its strength and unlocking much deeper penetration.
A New Era for Joint Implants
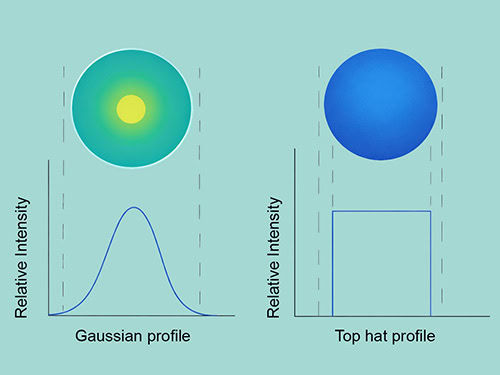 The two laser profiles compared. Credit: University of Basel
The two laser profiles compared. Credit: University of Basel
The team tested their reshaped Er:YAG laser on thick bovine femur bones. To prevent the tissue from charring, the bone was continuously cooled with a micro-jet of water and blasts of compressed air. The results, published recently in the journal Scientific Reports, mark a significant leap forward.
While the traditional Gaussian laser stalled at a depth of roughly 2.6 centimeters (almost 1 inch), the top hat profile sliced down to 4.45 centimeters. This brings the technology remarkably close to the dimensions required for major joint resurfacing surgeries. Furthermore, microscopic analysis confirmed that the bone’s cellular network remained intact and healthy right up to the edge of the cut.
Yet, the laser blade is not quite ready to banish the mechanical saw from the operating room. The sheer speed of the cut remains a stubborn hurdle.
Currently, the top hat laser removes about 0.42 cubic millimeters of bone per second. A conventional oscillating saw, by contrast, removes roughly 11 cubic millimeters per second—nearly 25 times faster.
Despite this operating time gap, the unprecedented depth achieved by the team opens a realistic pathway for mainstream clinical use. The researchers are now focused on refining the robotic delivery system for living, vascularized tissue.
“As part of the next steps, we will also need to investigate how we can adapt the system to the more complex situation in the body. There, it is also about protecting the surrounding tissue,” explains Dr. Ferda Canbaz.

