A new preclinical study has demonstrated that locking the focal adhesion kinase (FAK) protein may help the immune system better detect and attack ovarian tumours.
Scientists have identified a potential strategy to strengthen the immune system’s ability to fight one of the most aggressive forms of ovarian cancer.
Researchers from Sanford Burnham Prebys Medical Discovery Institute and University of California San Diego found that blocking a protein known as focal adhesion kinase (FAK) enabled more tumour-fighting immune cells to reach cancerous tissue in mice and improved the effectiveness of immunotherapy.
The findings provide new insights into how tumours suppress immune responses and suggest a possible way to overcome treatment resistance in high grade serous ovarian cancer, the most common and difficult-to-treat form of the disease.
Tumours that evade immune attack
Cells in the immune system are responsible for defending the body against external threats such as bacteria and viruses. They also play an important role in identifying and destroying abnormal cells that may develop into cancer.
Earlier preclinical studies suggested that drugs blocking FAK could increase the effects of chemotherapy.
However, many cancers evolve strategies that help them avoid detection or weaken immune responses. In ovarian cancer these mechanisms can also reduce the effectiveness of immunotherapies designed to activate immune cells against tumours.
“Even if you boost the capability of immune cells, a treatment will have limited success if the cells struggle to recognise and react to the tumour,” said Dr David Schlaepfer, a professor in the department of OBGYN and Reproductive Sciences at the UC San Diego Moores Cancer Center.
Previous research had identified a possible driver of this immune resistance. Genetic mutations cause an overabundance of FAK in more than three quarters of cases of high grade serous ovarian cancer and the protein is associated with poorer patient survival.
Earlier preclinical studies suggested that drugs blocking FAK could increase the effects of chemotherapy. These findings have already contributed to the launch of a Phase II clinical trial exploring this approach.
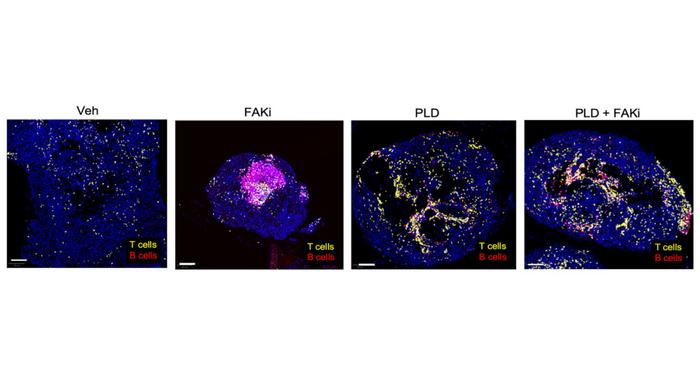
This figure shows the results of treating an aggressive, chemotherapy-resistant ovarian mouse tumour model with an FAK inhibitor and/or a chemotherapy called Pegylated liposomal doxorubicin or PLD. Compared with untreated mice labelled as vehicle (Veh), the combined treatment led to controlled tumour growth while modifying the immune response to increase the infiltration of T and B cells. Credit: David Schlaepfer & Kevin Tharp.
Testing a combination approach
To better understand the potential of FAK inhibition researchers used an aggressive mouse model of ovarian cancer that mimics the chemotherapy resistance seen in patients with high grade serous ovarian cancer.
The scientists compared several treatment strategies including a drug that blocks FAK alone and in combination with chemotherapy and immunotherapy. These groups were then measured against untreated control mice.
The team assessed tumour size, survival time and the presence of immune cells known as B cells and T cells that can attack tumours.
The most effective results occurred when the FAK inhibitor was combined with both chemotherapy and immunotherapy.
The most effective results occurred when the FAK inhibitor was combined with both chemotherapy and immunotherapy. This triple treatment improved the recruitment of immune cells to tumours, reduced tumour growth and increased survival in the mice.
“Once it was established that genetically or pharmacologically targeting FAK improved the ability of the immune system to recognise and attack ovarian tumour models, then we needed to figure out how this worked,” said Dr Kevin Tharp, an assistant professor in the Cancer Metabolism and Microenvironment Program at Sanford Burnham Prebys.
Macrophages switch roles
The researchers discovered that the treatment changed the behaviour of macrophages, which are normally known for engulfing bacteria and other harmful material.
Instead of focusing solely on this function the macrophages began sending chemical signals that helped coordinate an immune attack against the tumour.
“With FAK blocked, the macrophages that coordinate the immune system’s response to a tumour started assisting other immune cells in recognising and targeting the tumour,” said Tharp.
The team found that macrophages produced a signalling protein called CXCL13. This molecule helped recruit B cells and T cells to the tumour site where they formed structures similar to temporary immune bases known as tertiary lymphoid structures.
Potential path towards new therapies
The researchers say more work is required before the findings can be tested in clinical trials involving patients. Future studies will explore combination therapies using FAK inhibitors alongside existing chemotherapy and immunotherapy treatments.
“The moment high grade serous ovarian cancer becomes metastatic, it’s too distributed throughout the body for you to really do anything but recruit the immune system,” said Tharp. “I think that this represents an important treatment opportunity for patients who have progressed and not responded to the standard of care. It’s an extreme clinical need.”