Have you ever been to a MyHealth GP clinic, bought weight loss treatments at health.hub or had a telehealth appointment with Blua?
If so, you were being treated by an operation owned in part by some of the country’s major private health insurers.
Since the pandemic, health insurers have increasingly pursued a ‘vertical integration’ business strategy, which involves investing in or partnering with other businesses along the health service supply chain.
Whereas once insurers mainly had their own dental or optical service providers, now insurers are increasingly expanding their reach into GP medical centres and telehealth providers.
The most recent foray by insurers into GP care has raised specific concerns that insurers may be creeping too close towards US-style managed care.
It has raised alarms among medical groups, who are calling for more guardrails.
 Medibank Private owns a majority stake in MyHealth Medical Centre through Amplar Health.(ABC News: John Gunn)
Medibank Private owns a majority stake in MyHealth Medical Centre through Amplar Health.(ABC News: John Gunn)
In the most recent moves, Medibank Private’s subsidiary, Amplar Health, now has a 90 per cent stake in MyHealth’s 105 GP clinics.
In December, it was given sign off by the competition watchdog, the Australian Competition and Consumer Commission, to buy another 61 clinics owned by Better Medical.
Bupa own 27 medical centres in Australia and in May announced plans to get to 130 by 2027, along with 60 mental health clinics, which would make it one of the biggest in the country.
“There’s far too little oversight of the sector,” Australian Medical Association vice president Julian Rait said.
“Private health insurers have attempted to get more involved in primary care, and we think they’re doing this really to follow the US models.”
While there are laws in Australia restricting managed care, the concern is that insurers are slowly pushing too close to the line of what is legally allowed or exploiting loopholes.
So who owns what:Medibank Private Sign on a Medibank building in Sydney on June 9, 2011.(AAP)Owns Amplar Health, which has a 90 per cent stake in 105 MyHealth GP clinics 61 Better Medical clinicsAmplar also offer home hospital services and GP telehealthAmplar owns a minority share in seven private hospitals, including Adeney Private in Kew, three mental health hospitals, East Sydney and Western Adelaide PrivateBupa
Sign on a Medibank building in Sydney on June 9, 2011.(AAP)Owns Amplar Health, which has a 90 per cent stake in 105 MyHealth GP clinics 61 Better Medical clinicsAmplar also offer home hospital services and GP telehealthAmplar owns a minority share in seven private hospitals, including Adeney Private in Kew, three mental health hospitals, East Sydney and Western Adelaide PrivateBupa Operates 27 GP clinics with plans to move up to 130 by 2027Plans for 60 mental health clinicsBupa Dental and Optical Partnership with AmplifonBlua digital healthNIB
Operates 27 GP clinics with plans to move up to 130 by 2027Plans for 60 mental health clinicsBupa Dental and Optical Partnership with AmplifonBlua digital healthNIB nib generic logo(Supplied: nib)Majority share in hub.healthOffers members 10 per cent discounts on GP telehealth consults.NIB dentalAudiology deal with SpecsaversHCF
nib generic logo(Supplied: nib)Majority share in hub.healthOffers members 10 per cent discounts on GP telehealth consults.NIB dentalAudiology deal with SpecsaversHCF Signage at a HCF healthcare outlet in Sydney, Friday, Feb. 24, 2017.(AAP: Joel Carrett)Offers free GP visits through partner GP2U productsHCF dental centres
Signage at a HCF healthcare outlet in Sydney, Friday, Feb. 24, 2017.(AAP: Joel Carrett)Offers free GP visits through partner GP2U productsHCF dental centres
Catholic Health Australia represents 85 Catholic hospitals nationally.
Its health policy director, Katharine Bassett, said the insurers’ move towards vertical integration had been happening slowly over time, but it had reached a critical juncture.
“We’re now at a point where our major insurers are some of the biggest players when it comes to delivering healthcare,” she said.
Dr Bassett said insurers were finding ways to exploit loopholes in existing laws preventing managed care.
“Insurers are using quite clever ways to do these models of care, so they’re framing them as things like pilots or experiments or ways to test innovation.”
For example, Medibank is piloting a Proactive Primary Care pilot in three Western Sydney MyHealth clinics.
Under the pilot, MyHealth chronic disease patients, regardless of insurer, get reviews of their health with the aim of ordering scans and tests and intervening early.
The insurer stands to benefit because if it can prevent people from getting sick and ending up in the hospital, even if only some are Medibank customers, it will reduce how much the insurance company pay out in claims.
“The challenge is when you have a funder that’s also delivering care, they’re looking at it from a cost containment perspective as opposed to a patient access choice and quality perspective,” Dr Bassett said.
Insurer-owned GP clinics could impact referrals Julian Rait says perverse incentives can potentially creep in when insurers own GP clinics. (ABC News: Simon Winter)
Julian Rait says perverse incentives can potentially creep in when insurers own GP clinics. (ABC News: Simon Winter)
The Australian Medical Association (AMA) is concerned that GPs in insurer-owned clinics could be pressured into referring patients to insurer-owned hospitals or preferred no-gap specialists.
While that could be a win for some patient hip pockets, it might not be the best option for their treatment.
“Over a period of time, various perverse incentives can creep into such arrangements, and that’s why we’re very concerned,” the AMA’s vice president, Julian Rait, said.
While patients are legally allowed to take their referral to any specialist, many patients rely on their GP for recommendations for specific specialists or medical facilities in their area.
“If they [insurers] also control the referral pathways, it’s very easy for them to encourage referral to their own facilities,” Dr Rait said.
“It means that patient choice is reduced, but it also diminishes the competition that’s available.”
The ABC has previously exposed non-insurer GP clinics where incentives to over-service have come from above.
Insurers say they’re trying to ‘plug gaps’ in system
Health insurer industry body Private Healthcare Australia chief executive Rachel David said insurers cannot tell GPs what to do.
“The health funds are not trying to take over the whole health system. What they’re trying to do is to plug gaps in the health system that consumers are experiencing,” she said.
She said ‘managed care’, which is a main feature of the system in the United States, was impossible in Australia because health funds had to pay regardless of the hospital.
Also, health funds do not employ doctors directly, and patients purchase insurance privately, not through employers.
“We have a totally different health system,” she said.
“What the funds are trying to do is ensure that there are sufficient funds available for GPs to engage in things like preventive health,” she said.
Is insurer telehealth queue-jumping?
With insurers moving into GP telehealth, the AMA and Catholic Health Australia have raised concerns that it is opening the door to a two-tier system where those with private health insurance get better access to GPs.
While anyone can use these services, the insurers are offering discounts that make it cheaper for members compared to others.
For example, Bupa already offers up to six free doctor telehealth appointments for its members through its digital health company Blua.
HCF offers free online GP appointments for some of its rural and remote members through its partner GP2U, or $50 for other members.
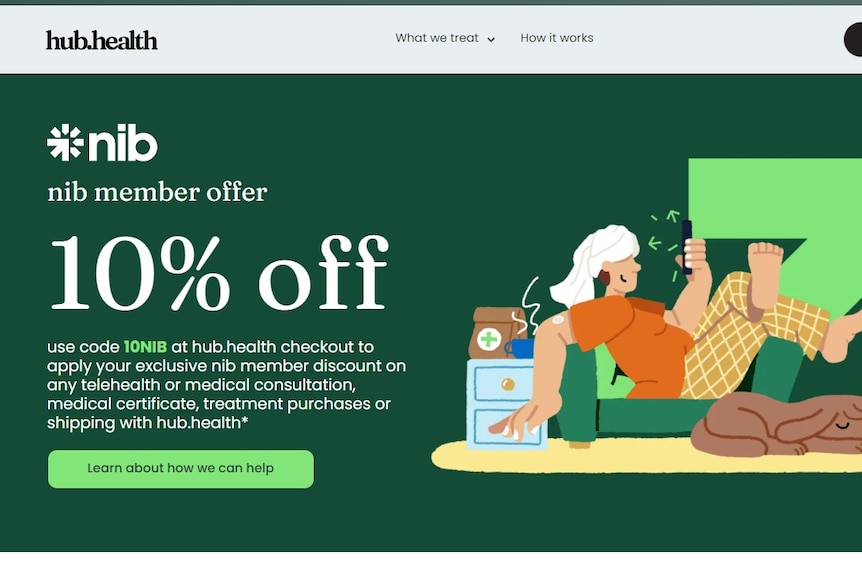 Insurers like NIB offer discounted telehealth services to members.(ABC News: Supplied)
Insurers like NIB offer discounted telehealth services to members.(ABC News: Supplied)
Similarly, NIB gives its members discounts on GP telehealth consultations at hub.health, marketing a range of services from contraception consults to medical certificates.
The telehealth services are legal because of a loophole created by the interaction of two laws.
One bans private health insurance covering anything outside the hospital, where Medicare might normally pick up the bill, and the other says Medicare cannot cover GP telehealth where there has not been a face-to-face consult in the past 12 months.
In effect, it opened the door for doctors who have not seen a patient in the flesh to charge for telehealth appointments via private health, but they cannot claim it on Medicare.
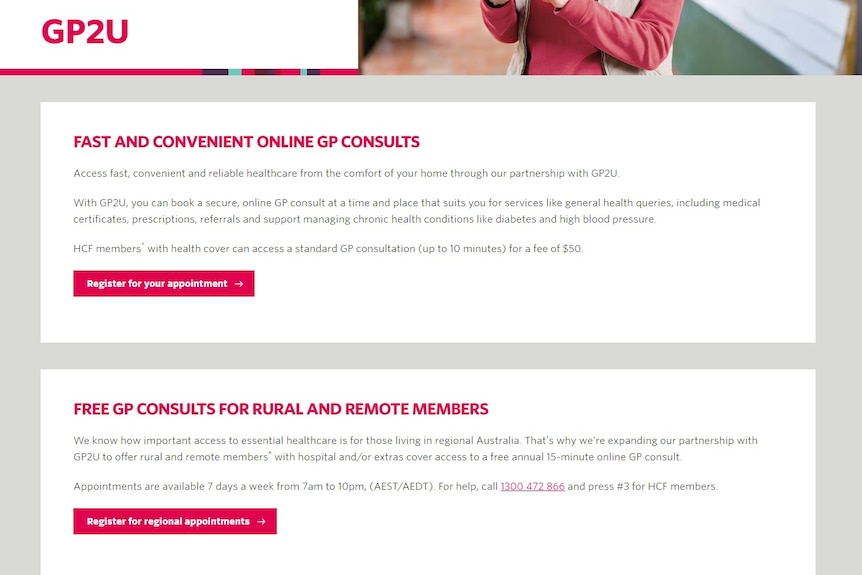 HCF partners with GP2u to offer free and discounted consults.(ABC News: Supplied)
HCF partners with GP2u to offer free and discounted consults.(ABC News: Supplied)
The AMA’s Dr Rait said if these clinics start hiring up all the GPs or paying them more per consult, it could draw doctors away from standard clinics funded via Medicare rebates.
“In a situation where there is supply shortage of GP’s … that does pose a particular risk for two-tiered health system,” he said.Insurer influence already being felt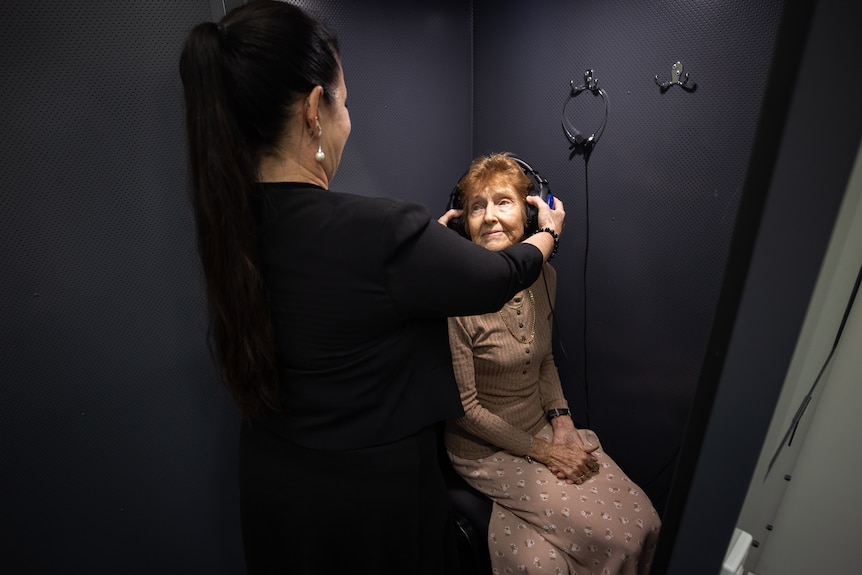 Audiologists say patients can struggle to shop around if their insurer refers them to a preferred provider.(ABC News: Luke Bowden )
Audiologists say patients can struggle to shop around if their insurer refers them to a preferred provider.(ABC News: Luke Bowden )
Concern about insurer encroachment on patient choice is being felt in the audiology sector.
Rachel Gibson represents Independent Audiologists Australia, whose members are struggling to compete with hearing giant Amplifon, which partners with Bupa.
She said they were hearing from patients that they were being told by Bupa they must go to Amplifon to receive a rebate, when it is not true; they can get a rebate at many providers, albeit smaller.
“We are seeing a lot of hearing services that are now operating through health fund storefronts and partnerships that promote member offers,” she said.
“This can sometimes then funnel the patient into a pathway without really understanding their alternatives.” Rachel Gibson says smaller audiology operators struggle with insurer referrals to preferred providers.(ABC News: Luke Bowden)
Rachel Gibson says smaller audiology operators struggle with insurer referrals to preferred providers.(ABC News: Luke Bowden)
One member reported a case to them of a parent who needed a hearing test for their child and was told to go to Amplifon by Bupa, even though that service does not do paediatric cases.
“That provider did not do paediatric services, nor did they do the auditory processing assessment.”
Bupa said in a statement that its partnership with Amplifon allowed its customers to save money and avoid out-of-pocket costs, and anyone could access Amplifon, not just Bupa customers.
“Bupa’s Medical Centres, Optical & Hearing stores, mental health clinics, and dental practices are open to all Australians, not just Bupa customers, which reinforces that these are not closed or insurer‑directed services.”
Amplifon has been contacted for comment.
Insurers questioning decisions: ombudsman
It is not just in extra policies where there is concern that insurers are trying to exert control over decision-making.
The Ombudsman in 2024 released a report concerned about private health insurer tactics when it came to Type C certificates.
These are a special form that doctors use when a procedure normally done in their rooms needs to be done in a hospital for medical reasons.
It noted in many complaints “the insurer questioned whether the clinical procedure was necessary but did not decline the claim outright, effectively leaving the claim in limbo — and in some cases the patient was left out of pocket”.
The AMA said complaints had reduced since the review, and Julian Rait said while managed care was not commonplace these “are some disturbing signs” it was being adopted.
“These are the first sentinel events that suggest that it’s seriously being considered by the private health insurers.”Medical associations say more oversight is needed
The Australian Medical Association and Catholic Health Australia are calling for a dedicated industry regulator to oversee insurers.
At the moment, there are APRA, the ACCC and the Ombudsman, who have narrower prudential and consumer oversight.
 Brett Heffernan says vertical integration is happening “willy nilly”.(ABC News: Tobias Hunt.)
Brett Heffernan says vertical integration is happening “willy nilly”.(ABC News: Tobias Hunt.)
Brett Heffernan from the Australian Private Hospitals Association said hospitals have firsthand experience trying to fend off insurer pressure in realms like rehabilitation and prosthetics, and it needed closer inspection.
“It certainly needs to be looked at in great detail by the government. At the moment, it’s just happening willy nilly,” he said.
 The AMA and Catholic Health Australia are calling for a dedicated industry regulator to oversee insurers. (ABC News: Luke Bowden)
The AMA and Catholic Health Australia are calling for a dedicated industry regulator to oversee insurers. (ABC News: Luke Bowden)
In a statement, Health Minister Mark Butler said the government had no plans to allow private health insurers to move into general practice services — despite the existence of the telehealth services and GP clinic buy-ups.
It said it supported “innovation” by insurers in “prevention and complementary services” so long as they operated within Medicare’s rules.
“Australia has a long standing and deliberate policy to prevent a two-tier system in general practice and access to primary care,” he said.
“Any move by insurers into GP services would be a significant change to Medicare and is not being considered.”
Hospital in the home battleground Katharine Bassett says vertical integration has not happened in a coordinated way.(ABC News: Dan Irvine)
Katharine Bassett says vertical integration has not happened in a coordinated way.(ABC News: Dan Irvine)
Catholic Health Australia have raised concerns about Medibank’s hospital in the home services, saying Amplar was competing with Catholic hospital offerings.
“The challenge is that these models have been able to continue and there’s been no conscious design around what we actually want the system to.”
If it wants to offer no gap, it must contract back through Medibank’s Amplar, as opposed to having the program directly funded.
“So some of the patients that we see, they want to choose a Catholic provider because of the values we have,” she said.
What the funds told us
NIB said in a statement that any member of the public could access hub.health telehealth services, and its 10 per cent discount to NIB members was “modest” on a $49 consult.
“Telehealth provides access to GPs for patients, especially those in regional or remote Australia, where getting access to a doctor can be difficult,” the statement read.
It said GPs could refer to any doctor, and it had a specialist search tool on its website to help patients shop around.
HCF said its partnership with GP2U was one of many and designed to “improve convenience, access, and continuity of care — not to direct healthcare choices or influence clinical decision making”.
“Participation in any program is optional, and clinical decisions remain independent.”
BUPA said it does not support managed care, believes in the autonomy of doctors, and its clinics and telehealth services were open to the public.
“We want to empower all Australians to manage their own health and wellbeing with greater access to more preventative, personalised, and innovative health care to keep people healthier, earlier,” it said in a statement.
Medibank said it was committed to “driving the broader health transition” and its focus extends beyond the needs of its customers to “system-wide change”.
It said it wanted to invest in prevention but would not influence GP decisions or referrals.
“The clinics will continue to be open to everyone, regardless of whether they are a Medibank customer.”
It said it funds Amplar Health for some hospital in the home services but also funds a range of third-party providers.

