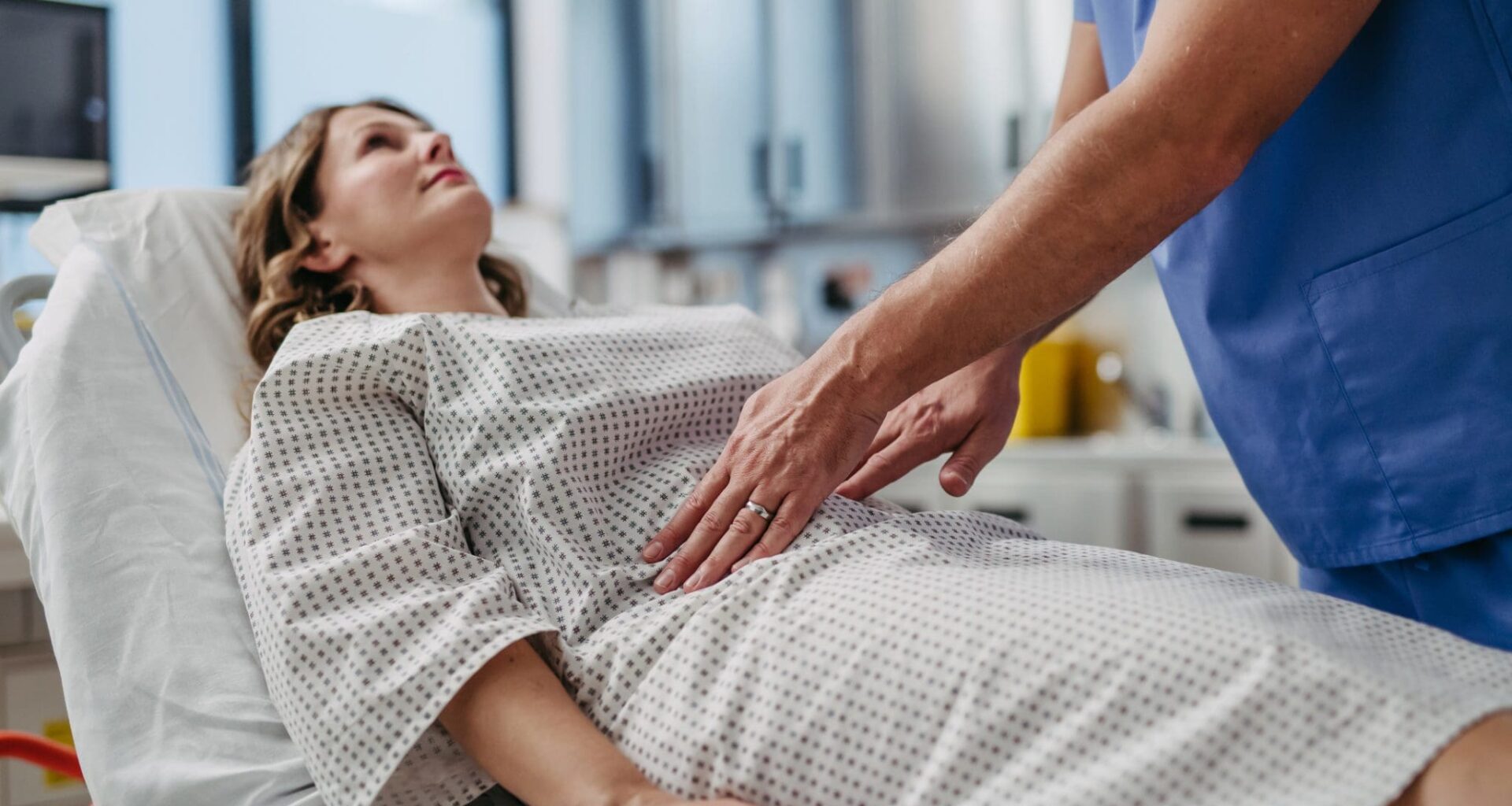
 image: ©Halfpoint | iStock
image: ©Halfpoint | iStock
New guidance from NICE explains the new fertility pathway for endometriosis, including natural conception, surgery, and IVF
The UK health body has revealed an updated fertility guideline. It now provides specific support for patients with endometriosis who are struggling to conceive. Following public consultation, NICE recognises, for the first time, the need for a dedicated and tailored fertility pathway for endometriosis. This is separate from other causes of infertility.
Endometriosis affects around 1.5 million people in the UK. It occurs when tissue, similar to the womb lining, grows in other parts of the body. It is one of the leading causes of fertility problems.
Patient and expert feedback shape the guidelines
NICE’s independent committee sought feedback from patients, patient groups, clinicians, and professional bodies.
Endometriosis UK and others told NICE during consultation that endometriosis was being grouped with unexplained infertility, even though it is a diagnosed condition. The committee agreed that this grouping was inappropriate and that a distinct fertility pathway for endometriosis was necessary.
Respondents also told NICE that terms such as “mild” and “severe” endometriosis were clinically ambiguous and did not reflect the complexity of the condition or its impact on fertility. The committee agreed, and these terms have been removed from the final guideline.
New guideline sets out fertility pathway for endometriosis
The guideline will outline new recommendations for clinicians, ensuring they discuss a wide range of fertility support options. For example, patients with endometriosis who are trying to conceive should take into account individual factors, including how long they have been trying to conceive, the severity of their symptoms, their age, their ovarian reserve, and any male fertility factors.
The guideline sets out a clear fertility pathway for endometriosis. Expectant management (time to try to conceive naturally) may be offered, or surgical treatment to address endometriosis, in line with NICE’s existing endometriosis guideline (NG73). If neither approach is suitable or successful after 2 years, fertility treatment options, including intrauterine insemination (IUI) or IVF, will be discussed.
The guideline aims to offer a more personalised pathway for endometriosis patients. It seeks to ensure fertility services are tailored to individual needs, reduce variation in care, and support equitable access across England.
Voices from the front lines of endometriosis care
“For too long, women with endometriosis who wanted to start a family have navigated a fertility system that did not fully recognise the distinct challenges their condition presents. This new guidance changes that,” commented Eric Power, interim director of the Centre for Guidelines at NICE.
Eric continued: “We listened carefully to what patients, clinicians and patient groups told us during consultation. They described how complex endometriosis is, how they felt existing labels were misleading, and that the condition needed its own pathway. The committee agreed and acted on that feedback.
“By creating a dedicated section for endometriosis, we are giving clinicians a clear, evidence-based framework to have better, more personalised conversations with their patients, ensuring that everyone, regardless of the cause of their fertility problems, has access to the right care at the right time.”
Emma Cox, chief executive of Endometriosis UK, said: “This year’s Endometriosis Action Month theme is ‘Endometriosis Doesn’t Wait’ – and our new State of Endometriosis Care report shows just how urgently change is needed. With average diagnosis times now standing at 9 years and 4 months — and 11 years for those from ethnically diverse communities — many have already waited far too long by the time they reach fertility services.
“Today’s guidance marks a step change in the fertility support that anyone with endometriosis should receive. For years, those with endometriosis have told us they felt invisible within the fertility system – grouped with unexplained infertility despite having a diagnosed condition. We welcome NICE’s decision to listen to patient voices during consultation, to create a dedicated pathway, and to remove misleading labels like ‘mild’ and ‘severe’ endometriosis.”
Sanchia Alasia, trustee and support group leader for Endometriosis UK, said: “I have lived with endometriosis for many years and have been through a number of IVF treatments. Because my endometriosis also affects my bowel, I required care from a multidisciplinary team – including a bowel surgeon, fertility consultant, and endometriosis specialist. Having coordinated input from all these clinicians was crucial in helping me understand my options and ensuring that decisions about fertility treatment took the full complexity of my condition into account.
“Not everyone has access to this level of joined-up care, and navigating the fertility system with endometriosis can be confusing and overwhelming. That is why the updated NICE guidance is such a welcome development. It provides clearer, more consistent direction so patients can be placed on the right fertility pathway sooner, with recognition of how endometriosis can affect multiple systems and require multi-specialist involvement.”