Key Insights
Health-care systems around the world are trying to decrease the use of inhaled anesthetics without impacting patient care.
Some of the gases, including fluorinated ether anesthetics, are potent greenhouse gases, while others also deplete the ozone layer.
Bans on desflurane have reduced the greenhouse gas impact from medical anesthesia emissions by 27% between 2014 and 2023, but desflurane’s use is now going up in some countries.
Noe Woods cares deeply for people and the environment. An obstetrician-gynecologist by training, she has invested in rooftop solar panels and completely electrified her house, and she bikes or drives her electric vehicle to work.
So when Woods first heard that some of the anesthetic gases she and her colleagues use to ease patients’ pain are bad for the planet, she set out to change things. She presented the issue to the anesthesia department at the University of Pittsburgh Medical Center (UPMC), where she works, and her colleagues listened. “The chair of the department of anesthesia at Magee-Womens Hospital said, ‘This is the nail in the coffin for desflurane,’ and he proceeded to remove desflurane until its last use at Magee in 2013,” she says. Desflurane is an anesthetic that is 2,540 times as potent a greenhouse gas as carbon dioxide.
Woods didn’t stop there. Along with several like-minded physicians at UPMC, she formed Clinicians for Climate Action in 2022—more than 500 clinicians are part of the group today—and a year later, the group encouraged UPMC to launch its Center for Sustainability.
The center hired an engineer, who calculated the hospital’s greenhouse gas footprint from anesthetic gas use. That data gave the group powerful leverage to make the case for changing behavior, Woods says. In 2024, UPMC banned the use of desflurane across all 40 hospitals in its vast western Pennsylvania network.
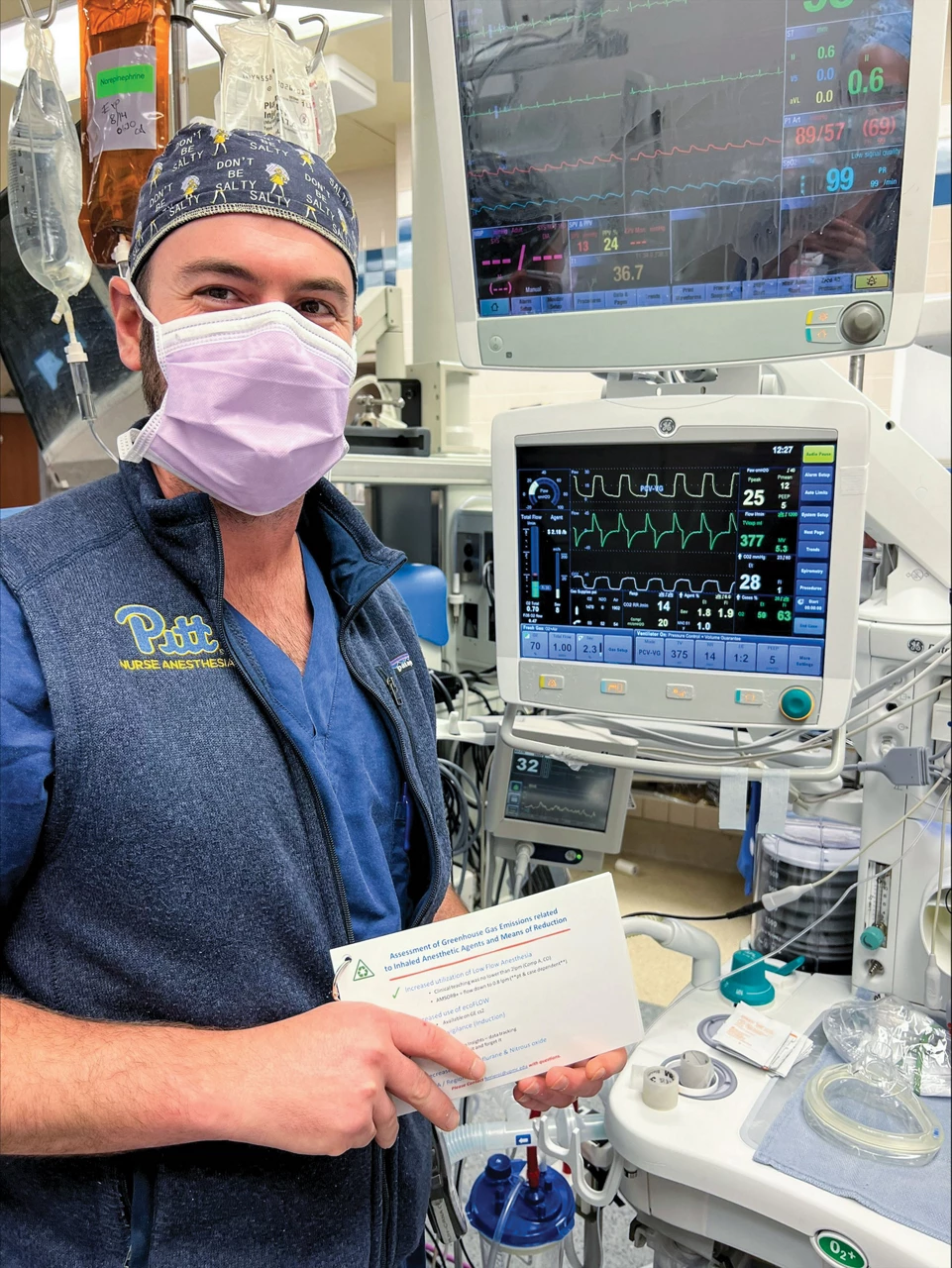
A person wearing a face mask and head covering stands beside a counter containing various pieces of medical equipment, including IV bags and two screens that display data curves.
Anesthetist Joseph Ferriero, seen here standing beside an anesthesia machine at the University of Pittsburgh Medical Center Presbyterian hospital, has been instrumental in decarbonizing anesthesia throughout the UPMC system.
Credit:
University of Pittsburgh Medical Center
UPMC isn’t the only one. A number of hospitals and health-care systems in the US, Canada, Europe, and Australia are starting to phase out desflurane. Across the Atlantic, Scotland banned desflurane anesthetics in 2023. And on Jan. 1 this year, the European Union prohibited its use unless medically necessary. These efforts, often driven by medical professionals, are part of a growing push to cut the environmental impact of anesthesia—whether by banning the worst offenders or reducing the use of others—without altering the quality of patient care.
“Whether you are in the car industry or in the airline industry or hospitality, there are planetary health consequences to what you do,” Woods says. “And there are people in all these fields who care and who are trying to remediate the damage they do. I happen to be in health care. And these aren’t things that are part of being a physician, per se, but they’re part of being a global citizen.”
The global harms of anesthetic gases
Globally, inhaled anesthetics are responsible for 3% of the total carbon footprint of national health-care systems, according to the American Society of Anesthesiologists (ASA). These gases are critical for patient comfort and safety during medical procedures. But patients’ bodies metabolize only about 5% of the anesthetic they breathe in through a mask; they exhale the rest of the gas, mostly unchanged, and it is vented into the atmosphere.
Those vented gases can have an outsized impact. The exact carbon emissions for hospitals vary, depending on emissions from electricity and heating, staff commutes, and whether a facility uses helicopters. But “anesthesia is a disproportionate contributor to a hospital’s greenhouse gas footprint,” says Douglas A. Colquhoun, a professor in the University of Michigan (U-M) Medical School’s Department of Anesthesiology. “Depending on numbers, it’s 6 to 10%, potentially, of a hospital’s carbon dioxide footprint.”
Packing a punch
These common inhaled anesthetics, all fluorinated ethers, are potent greenhouse gases.
Desflurane
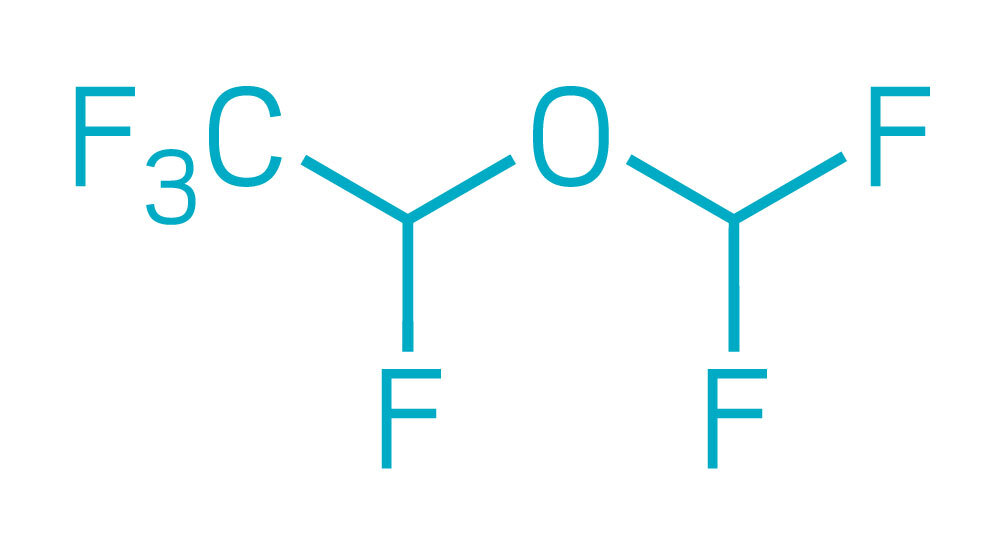
Mean alveolar concentration: 6.70%
Atmospheric lifetime: 14 years
Global warming potential*: 2,540
Equivalent auto miles** driven at anesthetic use of 1 L/min per hour: 190
Isoflurane
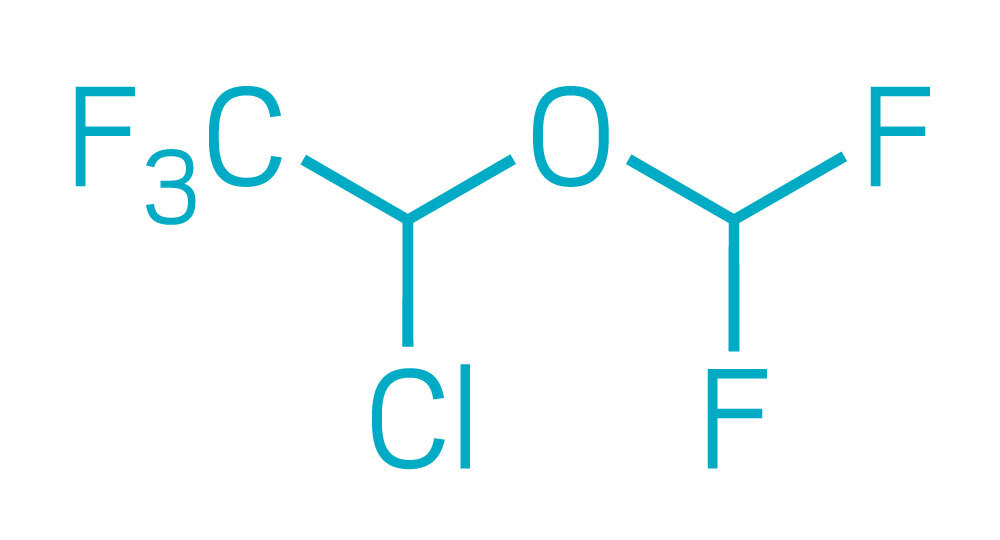
Mean alveolar concentration: 1.20%
Atmospheric lifetime: 3.6 years
Global warming potential*: 539
Equivalent auto miles** driven at anesthetic use of 1 L/min per hour: 8
Sevoflurane
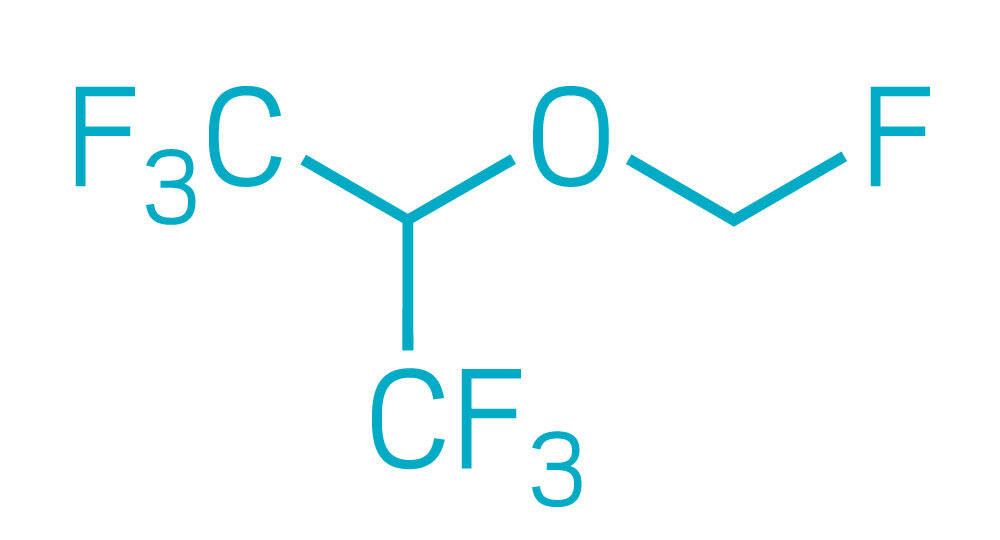
Mean alveolar concentration: 2.20%
Atmospheric lifetime: 1.9 years
Global warming potential*: 144
Equivalent auto miles** driven at anesthetic use of 1 L/min per hour: 4
*GWP100; global warming potential relative to carbon dioxide over a 100-year period.
**Based on EPA 2022 emission factor of 4.03 x 10-4 metric tons of CO2-equivalent/mile.
Commonly used anesthetics, such as desflurane, sevoflurane, and isoflurane, are halogenated ethers and potent greenhouse gases. The degree to which they warm the Earth’s atmosphere depends on how much infrared radiation they absorb and how long they last in the atmosphere.
Desflurane is the biggest climate culprit. Each hour of its use produces the same warming potential as driving a gasoline-powered car for about 300 km. For sevoflurane, that number drops to around 6 km. These fluorinated gases also react with oxygen and water in the atmosphere to produce trifluoroacetic acid, a potentially harmful contaminant that persists in the environment. Meanwhile, another major anesthetic, nitrous oxide—known as laughing gas—is the next-worst planet-warming offender after desflurane and also depletes the ozone layer.
The positive impact of anesthetic action
Bans on desflurane use are having a positive climate impact. Researchers at Lund University recently found that greenhouse gas impact from anesthetic gases has decreased by 27% between 2014 and 2023. Globally switching to using just sevoflurane, they estimated, could have decreased the impact of anesthetics by 73% (Lancet Planet. Health 2025, DOI: 10.1016/S2542-5196(25)00027-0).
In addition to switching to sevoflurane, many medical systems are cutting the volume of anesthetics they use.
Critically, this comes at no cost to patient care. To go under, patients breathe in anesthetic agents mixed with oxygen, air, and N2O in a closed circuit. Machines scrub CO2 from the exhaled air, add some fresh oxygen and anesthetic agent, and send the mixture back to the patient. It is possible to lower the flow of fresh gas added each time without affecting patient care. “This is just eliminating waste,” says Lucinda Everett, a pediatric anesthesiologist at Massachusetts General Hospital. “It does not result in providing less anesthesia to the patient.”
“These aren’t things that are part of being a physician, per se, but they’re part of being a global citizen.”
Noe Woods, obstetrician-gynecologist, University of Pittsburgh Medical Center
A recent study by Colquhoun and his colleagues at U-M proved this with solid numbers (Lancet Planet. Health 2025, DOI: 10.1016/S2542-5196(24)00331-0).
The U-M medical system launched its Green Anesthesia Initiative in 2022. This included shifting to sevoflurane, reducing the use of N2O, and increasing the use of intravenous sedatives. Using electronic health-record data from before and after the initiative was launched, Colquhoun and colleagues measured the amount of anesthetic used, climate impact, and patient outcomes. The team found that the initiative halved CO2 emissions, saving the equivalent of 2.7 million km of driving in a standard passenger car, without compromising patient safety or outcomes.
Reducing desflurane use brings cost benefits as well. Liter for liter, the gas costs more than sevoflurane and isoflurane. And it requires an expensive, more complex delivery device.
Yet another low-hanging fruit up for grabs in minimizing a hospital’s carbon footprint is changing the way N2O is distributed. Hospitals typically buy a big tank of N2O and put it in a central location, from where the gas is piped to various units. But, Woods says, “nitrous oxide is a really tiny molecule, and it can seep out of things.”
“Multiple groups have shown that up to 90% of what is bought cannot be shown to be delivered to a patient, so it’s just leaking out to the environment,” Colquhoun says. To reduce that leakage, several hospitals, including UPMC and Mass General, have stopped using centralized tanks and instead use small N2O cylinders at the anesthesia site.
A need for global alignment in anesthesia use
Many of the steps outlined above are listed in the ASA’s 2024 guidelines to reduce healthcare’s environmental impact: avoid desflurane and N2O unless necessary, cut fresh gas flows, and move to portable N2O tanks.
Newer waste-gas capture and photochemical destruction technologies seem promising, the guidelines say, but they need more validation. For now, the ASA encourages focusing on reducing anesthetic use and emissions.
Knockout nations
Countries with highest greenhouse gas impact of halogenated anesthetic agents from medical use in 2023.
A wider global conversation might be necessary. The Lund University study found that while desflurane use is going down in some countries, in others, such as Japan, China, India, and Russia, its use is on the rise.
In the end, patient comfort is the number one priority for doctors. For certain clinical applications, such as pediatric care and labor and delivery, clinicians say there is no substitute for inhaled anesthetics.
“We’re lucky to have a lot of different options for anesthetic medications currently, some of which are intravenous,” Everett says. “But there are specific situations where anesthesia gases might be preferable.” Each gas has particular properties that might be more suitable for a given patient or situation, she adds. “But whichever gas we might choose, standard practice in the past was very wasteful, and there are ways to use them more responsibly.”
Prachi Patel is a senior editor and physical sciences reporter at C&EN based in Pittsburgh.
Chemical & Engineering News
ISSN 0009-2347
Copyright ©
2026 American Chemical Society