
Get Watchdog news delivered free to your email inbox!
Sign up for free email updates from The Watchdog. You’ll be notified whenever we publish our latest award-winning investigative reporting, John Boyle’s Answer Man and Opinion columns, Tom Fiedler’s Democracy Watch, and more!
HCA Healthcare took control of Asheville’s nonprofit Mission Hospital seven years ago, on Feb. 1, 2019, but Groundhog Day seems the more appropriate anniversary. As in the 1993 film, the people of western North Carolina are trapped in a time loop. They’re forced to revisit the same hospital failures year after year.

At least four times since the sale — 2021, 2024, 2025, and now 2026 — inspectors from the state and federal Centers for Medicare and Medicaid Services have concluded that HCA/Mission’s noncompliance with federal health and safety regulations “has placed the health and safety of recipients in its care at risk for serious injury, serious harm, serious impairment, or death.”
Mission was also cited in 2020 following the suicide of a man discharged from the hospital without being evaluated by a psychiatrist, despite telling emergency services personnel who brought him there that “he was attempting to commit suicide by walking into the river because he could not bring himself to jump off the bridge.” It’s unclear if the incident, which occurred less than six months into HCA’s management, led to an immediate jeopardy citation.
Each time, Mission Health executives draft a plan to correct the deficiencies.
Each of the previous four times, CMS has accepted the plans and lifted the sanctions, only to be called back again.
Each time, HCA/Mission quickly returns to its profit-optimized management system, without addressing broader systemic and procedural issues, like staffing. Doctors and nurses complain. Many of them quit in frustration. Local officials express deep concerns. Patients and their families flood the North Carolina Department of Health and Human Services with complaints. Weary investigators return to Asheville, and the cycle is repeated.
The Groundhog Day routine is typically accompanied by an announcement that an independent ratings group has named Mission one of “America’s 50 Best” hospitals (11 years in a row, the only hospital in North Carolina so honored). The sanctions also seem to coincide with yet another HCA/Mission lawsuit to prevent rival hospitals from challenging its effective monopoly in western North Carolina.
Sign up for free Watchdog news alerts straight to your inbox.
And each time, the immediate jeopardy sanctions are followed by an HCA announcement of soaring profits.
HCA is a money machine
In its latest earnings filing, Jan. 27, Nashville-based HCA reported that net income — essentially profits — increased more than 30 percent in the quarter ending Dec. 31, 2025, over the same period a year earlier.
Did they add more hospitals to the 190 they already own? Nope. Did patient admissions rise 30 percent? More like 3 percent, according to HCA. Inpatient surgeries, outpatient surgeries, and emergency room visits were all essentially flat.
A cursory look at the 4Q 2025 report suggests that HCA is boosting profitability the old-fashioned way, by cutting costs and raising prices.
From a shareholder perspective, it’s a win. Total HCA revenue for calendar 2025 grew to $75.6 billion, up $5 billion over 2024. The HCA share price, $330 one year ago, peaked at $519 after the earnings report before settling back at the end of the week.
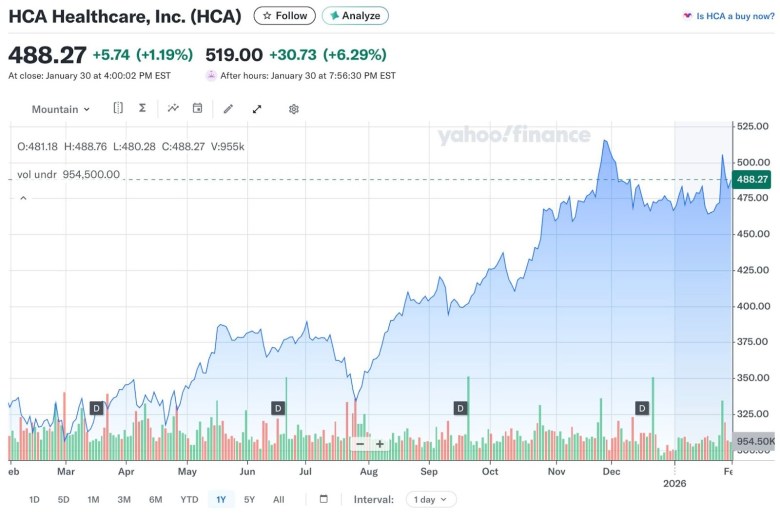 HCA Healthcare’s stock has increased 46 percent over the past year. On Feb. 2, 2025, it stood at $334.30 per share; it closed Friday at $488.27 per share. // Source: Finance.yahoo.com
HCA Healthcare’s stock has increased 46 percent over the past year. On Feb. 2, 2025, it stood at $334.30 per share; it closed Friday at $488.27 per share. // Source: Finance.yahoo.com
The company also provided guidance that revenue could hit $80 billion in 2026, despite anticipated headwinds from expiring “Obamacare” tax credits and greater restrictions on Medicaid.
Roughly 25 percent of the population in Republican U.S. Rep. Chuck Edwards’s 11th Congressional district — some 189,000 people — rely on Medicaid and the Children’s Health Insurance Program (CHIP), according to the American Community Survey and CMS. Mission Health’s footprint covers the same territory.
Last July, Edwards voted for the “One Big Beautiful Bill Act” that altered eligibility and administrative rules for Medicaid and CHIP, stripped minimum staffing transparency for some Medicaid services, and reorganized some funding priorities that health policy analysts said could reduce federal Medicaid funding access over time.
As a result, fewer people in western North Carolina will be able to afford healthcare, or qualify for Medicaid, which in turn will increase the number of uninsured and underinsured patients showing up at Mission. To compensate, HCA said it plans to be even more stringent on “cost discipline” in 2026. “We have confidence that we’ll be able to achieve $400 million of incremental cost savings in ’26 versus ’25,” the company’s chief financial officer said.
Sanctions and secrecy
Asheville’s Mission has become one of the most profitable hospitals in HCA’s portfolio, even as it has been repeatedly sanctioned for endangering patients.
These are not trivial deficiencies, like trash baskets not emptied or a meal tray not delivered. Fewer than 3 percent of all hospital health and safety violations rise to the level of immediate jeopardy, a situation that is “clearly identifiable due to the severity of its harm or likelihood for serious harm and the immediate need for it to be corrected to avoid further or future serious harm,” CMS regulations state.
There is no official database listing all the immediate jeopardy citations of U.S. hospitals since 2019 — neither the hospital itself nor CMS are required to tell the public that patients are endangered — but an Asheville Watchdog review of the most comprehensive listings suggests that under HCA, Mission must be a contender for the highest number of severe sanctions at one facility since 2019, certainly in North Carolina, if not the entire country.
On this Groundhog Day, we woke up once again wondering when our elected officials will finally make it mandatory for CMS and NCDHHS to inform the public when the healthcare systems they oversee are putting patients at risk. We find out about the dangers only through public records requests and, in some cases, when insiders leak the information to The Watchdog or other media.
By the way, our secure Signal account provides a way to send us news tips that no one but we can see. It’s AVLWatchdog.14.
Because of the secrecy and lack of a public reporting requirement, we don’t even know for sure how many times Mission and other HCA-managed hospitals in western North Carolina have been placed in immediate jeopardy, or the total human cost in patient health and safety.
Nancy Lindell, public relations manager for HCA’s North Carolina division and Mission Hospital, did not immediately respond to The Watchdog’s question: How many times has Asheville’s Mission been placed in immediate jeopardy since HCA took over management on Feb. 1, 2019?
Besides Mission, two other hospitals acquired by HCA in the 2019 sale — Blue Ridge Regional Hospital in Spruce Pine and Mission Hospital McDowell in Marion — also received immediate jeopardy citations, McDowell in 2021 and Blue Ridge Regional in 2023, records show.
We asked Lindell about the others: Angel Medical Center in Franklin, Highlands-Cashiers Hospital in Highlands, and Transylvania Regional Hospital in Brevard. Have they also received immediate jeopardy sanctions?
Nor did Lindell respond to a reminder that it has now been 2,099 days — more than five and a half years — since The Watchdog first requested a sit-down interview with Greg Lowe, HCA North Carolina Division president and Mission CEO. We’re still waiting.
Mission CEO cites ‘outside pressure‘
Details of the January 2026 immediate jeopardy citation are still secret, but Lowe’s letter to staff appeared to place some of the blame on patients and staff for “taking their concerns directly to CMS and bypassing the hospital.”
“We are committed to working with CMS to help ensure grievances are routed to Mission Hospital so we can work directly with our patients and colleagues to resolve any concerns,” Lowe wrote.
 It’s now been 2,099 days since Asheville Watchdog first requested a sit-down interview with Greg Lowe, HCA North Carolina Division president and Mission CEO. We’re still waiting. // Photo credit: Mission Hospital
It’s now been 2,099 days since Asheville Watchdog first requested a sit-down interview with Greg Lowe, HCA North Carolina Division president and Mission CEO. We’re still waiting. // Photo credit: Mission Hospital
After the October 2025 immediate jeopardy citation, Lowe criticized unspecified “misinformation that has been circulating online and in the press” and what he described as “outside pressure on these surveyors to find a problem.”
The CMS surveyors found multiple problems, actually, determining that two patients who came to Mission in need of help died because of “deficiencies in care.”
The 2024 Immediate Jeopardy citation (four patients dead) prompted Rep. Edwards to blame the deaths on “the failures of Obamacare.” His office did not immediately respond to a request for comment on the more recent sanctions.
The June 2021 citation (one patient dead) came to light only recently, which The Watchdog found buried in a footnote in a legal brief.
Another footnote in the same document asserted that HCA-owned Transylvania Regional was also placed in immediate jeopardy in 2021, but Asheville Watchdog has been unable to verify it.
Whether it’s four immediate jeopardy sanctions or five, or seven or more, the Groundhog Day pattern is playing out again. How many sanctions does a hospital system have to get — how many patients harmed are too many — before local, state, and federal regulators demand lasting changes, like minimum staffing levels, prompt public release of safety inspections, and greater competition for healthcare services?
As we mark the seventh anniversary of the sale of nonprofit Mission to HCA, it’s useful to remember that lawyers for HCA — asking a court to dismiss then-Attorney General Josh Stein’s lawsuit alleging broken commitments in the purchase — argued in 2024 that HCA never promised to provide quality healthcare.
As for Groundhog Day, the movie was funny. The recurring healthcare deficiencies at Mission are not. It’s time to stop HCA’s carousel of patient endangerment, promises and reprieves, and cost-cutting to serve investors rather than patients.
 The 1993 ‘Groundhog Day’ movie was funny. The recurring healthcare deficiencies at Mission are not.
The 1993 ‘Groundhog Day’ movie was funny. The recurring healthcare deficiencies at Mission are not.
Editor’s note: Despite the federal sanctions, if you are in a serious accident, or suspect you might be having a heart attack or stroke or other emergency health crisis, Asheville’s Mission Hospital is by far the best option for care in the Asheville area. It’s the only Level 1 Trauma Center in western North Carolina.
Asheville Watchdog welcomes thoughtful reader comments on this story, which has been republished on our Facebook page. Please submit your comments there.
Asheville Watchdog is a nonprofit news team producing stories that matter to Asheville and Buncombe County. Peter H. Lewis is executive editor and a former New York Times senior writer, editor and columnist. Email plewis@avlwatchdog.org. The Watchdog’s local reporting is made possible by donations from the community. To show your support for this vital public service go to avlwatchdog.org/support-our-publication/.
Support The Watchdog
Every dollar you donate to the nonprofit Asheville Watchdog stays in our community and goes directly to producing more award-winning coverage of important local issues.
Related

