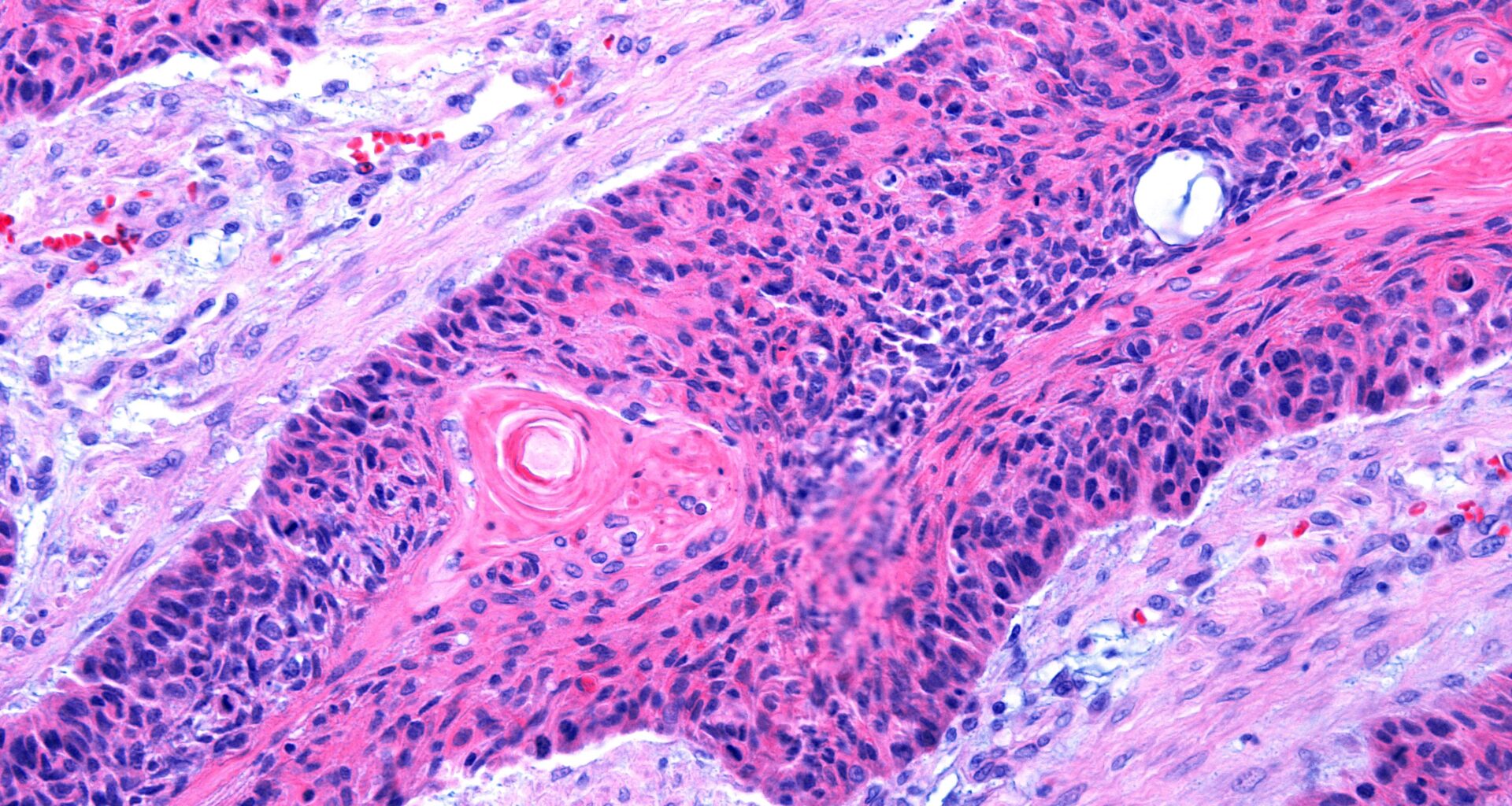
A topical cream that activates the skin’s immune defences has been shown to suppress tumour growth in early models of cutaneous squamous cell carcinoma.
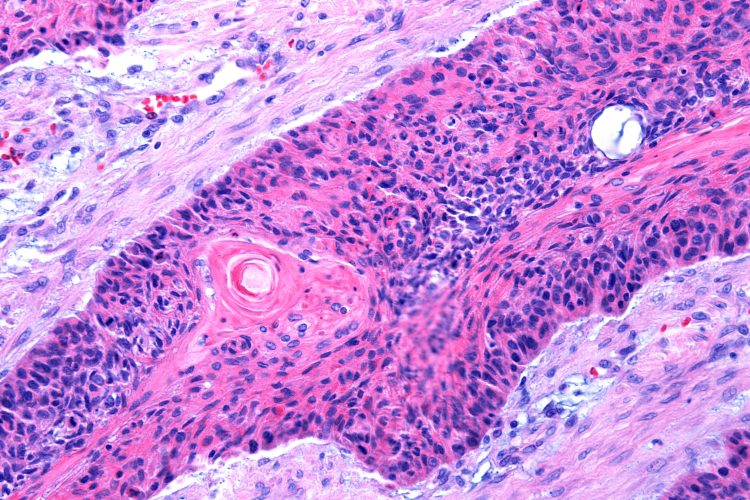
A topical cream that activates the skin’s own immune defences has demonstrated tumour suppression growth in two preclinical models of cutaneous squamous cell carcinoma (cSCC), one of the most common cancers worldwide.
The findings come from researchers at the Perelman School of Medicine at the University of Pennsylvania. The experimental cream works by blocking LSD1, an enzyme that normally suppresses immune-activating pathways in the skin.
Scientists say the treatment could one day be applied directly to cancerous or precancerous skin lesions, potentially reducing the need for surgery and other invasive procedures.
“What’s striking is that a simple topical cream can use the skin’s own machinery to recruit and activate immune cells that attack tumours,” said Dr Brian Capell, MD, a senior author of the study and an assistant professor of Dermatology at Penn. “We are carrying out some more studies to refine the formulation this coming year and we hope to begin a Phase I clinical trial in the next one to two years. Ideally, this cream could be used directly on cancerous and precancerous spots.”
A common cancer with limited treatment options
Cutaneous squamous cell carcinoma is among the most frequently diagnosed cancers. Around one million Americans are diagnosed with the disease every year and its incidence continues to rise as populations age and sun exposure increases.
Cutaneous squamous cell carcinoma is among the most frequently diagnosed cancers.
In most cases the cancer can be successfully treated with surgery. However, up to five percent of tumours spread beyond the original site, leading to thousands of deaths each year in the United States.
For many patients, particularly older adults or those with weakened immune systems, the condition can involve dozens of precancerous lesions appearing across large areas of skin. Treating each lesion individually can require repeated procedures that are both physically demanding and impractical.
Existing treatments for widespread lesions also have limitations. Chemotherapy is not targeted specifically at the cancer while some targeted therapies can cause significant pain. Surgery remains effective but carries risks such as infection and scarring.
Researchers believe a topical therapy that stimulates local immune responses against tumours could reduce the need for repeated procedures and help prevent early lesions from developing into invasive cancers.
‘Waking up’ the skin’s immune system
In their study, the research team created a low-dose topical inhibitor of LSD1. This enzyme normally acts as a brake on certain immune-activating pathways in epidermal cells.
By blocking LSD1 and effectively ‘lifting the brake’, the cream encouraged skin cells to send signals that recruit immune cells. Those immune cells then helped slow tumour growth in the experimental models.
By blocking LSD1 and effectively ‘lifting the brake’, the cream encouraged skin cells to send signals that recruit immune cells.
Further experiments helped clarify how the process works. When researchers blocked retinoic acid signalling – a naturally occurring cellular communication pathway that guides cell growth and development – many of the skin-level changes caused by the cream were reversed. In addition, eliminating CD4⁺ T cells, a type of immune cell, removed the treatment’s tumour-suppressing effect.
Together, the results indicate the therapy works by strengthening communication between skin cells and the immune system, allowing a more targeted anti-tumour response.
Potential for prevention as well as treatment
While treating existing skin cancer would be a major advancement, the researchers believe the greatest impact could come from preventing tumours from developing at all.
An estimated 58 million Americans live with skin precancers or early squamous cell carcinomas each year. A topical treatment that can be applied to large areas of affected skin could significantly reduce the need for repeated surgeries and lower the number of lesions that progress to invasive cancer.
The team is also exploring whether LSD1 inhibitors delivered orally or by injection could improve the effectiveness of immune checkpoint therapies. These treatments are currently beneficial for only a subset of patients with advanced cSCC.
If future clinical trials confirm the findings, the approach could offer a new strategy for using the skin’s own immune system to fight one of the world’s most common cancers.
Related topics
Cancer research, Clinical Trials, Drug Development, Drug Discovery, Drug Targets, Enzymes, Immunology, Immunotherapy, Oncology, T cells, Translational Science