This month, in April, the International Diabetes Federation formally recognized a new, distinct form of the disease: type 5 diabetes.
Roughly 25 million people worldwide live with this condition, predominantly in low- and middle-income nations where food is sometimes a luxury. For these individuals, the historical misinterpretation of their illness has been dangerous. Medical professionals have repeatedly treated them with therapies designed for entirely different metabolic breakdowns, sometimes triggering fatal blood sugar crashes.
By giving the disease an official designation, researchers can finally start designing treatments that actually fit the biology of these vulnerable patients.
Lost in Taxonomy
The human body requires precise chemical signals to extract energy from food. When that system breaks down, we call it diabetes. Type 1 diabetes is an autoimmune disease that destroys the pancreas’s ability to produce insulin. Type 2 diabetes involves insulin resistance and progressive beta-cell dysfunction, with risk shaped by genetics, environment, body weight, and lifestyle. Gestational diabetes arises from hormonal shifts during pregnancy. Type 3c results from direct physical damage to the pancreas—such as pancreatitis, pancreatic cancer, or surgery.
Amidst these well-defined categories, another variant lingered in the shadows. In 1955, a physician named P. Hugh-Jones documented young, undernourished people in Jamaica suffering from a strange form of diabetes that did not fit the usual categories of the time. They rarely suffered from ketoacidosis—a severe complication where the blood becomes dangerously acidic—which is what usually happens when type 1 diabetes goes untreated. He labeled the anomaly J-type diabetes.
The World Health Organization (WHO) briefly acknowledged the condition in 1985, classifying it as malnutrition-related diabetes mellitus. By 1999, however, the WHO erased the classification. The agency cited a lack of hard physiological evidence proving that malnutrition directly caused the disease. Without a formal name, research attention dwindled. Patients were forced into diagnostic boxes that simply did not fit their biology.
Not Enough Insulin
Solving the mystery required looking past the symptoms and into the metabolic machinery. Meredith Hawkins, an endocrinologist at the Albert Einstein College of Medicine’s Global Diabetes Institute, spent years pursuing the biological mechanisms of this underreported form of diabetes.
“Malnutrition-related diabetes is more common than tuberculosis and nearly as common as HIV/AIDS, but the lack of an official name has hindered efforts to diagnose patients or find effective therapies,” Hawkins said in a 2025 statement.
×
Thank you! One more thing…
Please check your inbox and confirm your subscription.
In 2022, Hawkins and her team published a key study establishing a unique metabolic profile for these patients. Operating out of South India, the researchers subjected patients to advanced metabolic testing, including clamp-based studies used to assess insulin sensitivity and insulin secretion.
The results showed that these patients were fundamentally different from conventional diabetes. Unlike type 1 patients, their immune systems had not destroyed their insulin-producing beta cells. Unlike type 2 patients, the 2022 study suggested they were not primarily insulin resistant.
Instead, their bodies suffered from a severe defect in insulin secretion. Their pancreases simply failed to produce enough of the hormone.
“Type 5 diabetes stands apart with its unique pathogenesis, theorized to involve compromised pancreatic development resulting from extended periods of nutritional insufficiency,” Rahul Garg, a physician at F.H. Medical College and Hospital in India, wrote in a 2025 review. Chronic starvation in early life may stunt the pancreas, leaving it unable to manage glucose later in adulthood—though the exact mechanisms are still being worked out.
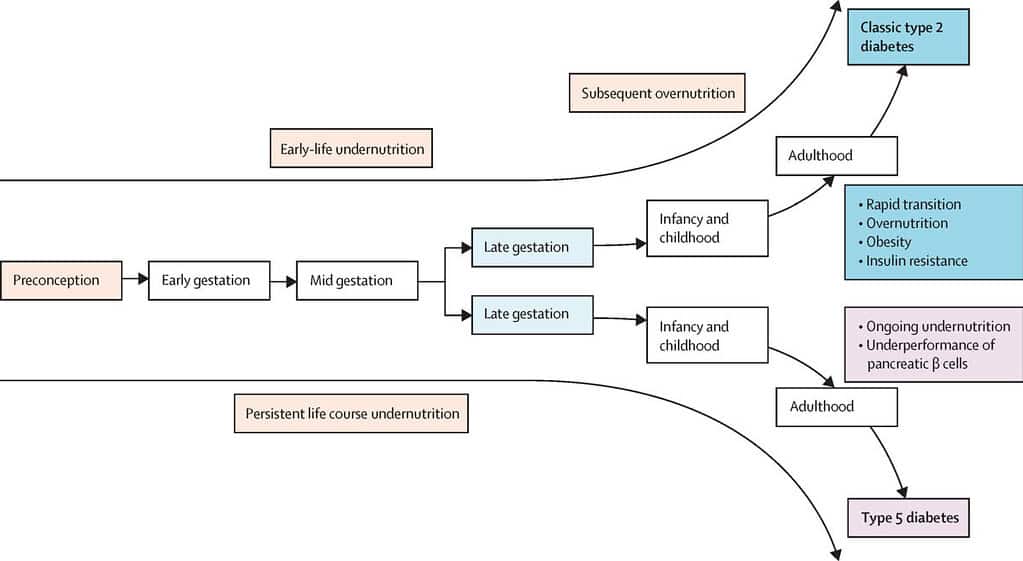 Life course evolution of adult diabetes phenotypes in different socioeconomic conditions. Credit: Wadivkar et al., The Lancet Global Health
Life course evolution of adult diabetes phenotypes in different socioeconomic conditions. Credit: Wadivkar et al., The Lancet Global Health
The Cost of the Wrong Label
With the biological mechanism exposed, the danger of misdiagnosis became much clearer. Treating an undernourished type 5 patient like a type 1 or type 2 patient can lead to major problems.
Standard type 1 management relies on injecting continuous doses of insulin. Because many patients appear not to be primarily insulin resistant, standard insulin treatments may raise the risk of hypoglycemia—a catastrophic plunge in blood sugar—if used inappropriately.
“Inappropriate insulin treatment could induce hypoglycemia [low blood sugar levels], which can be a particular risk in settings with food insecurity and where glucose monitoring might not be affordable,” Hawkins and colleagues explained in a 2025 review.
On the other hand, treating them like type 2 patients presents another hazard. Standard medical advice for newly diagnosed type 2 diabetes includes aggressive weight loss recommendations. For individuals surviving on the brink of starvation, with minimal muscle mass, deliberately losing weight accelerates their physical decline. Management may include nutritional rehabilitation, oral agents that stimulate insulin secretion, and low-dose insulin where appropriate.
“Understanding the specific types of diabetes someone has is crucial to providing the right treatment,” Craig Beall, a diabetes researcher at the University of Exeter, explained in The Conversation.
A New Chapter in Global Health
 Anterior view of a human male pancreas 3D model. Credit: Wikimedia Commons
Anterior view of a human male pancreas 3D model. Credit: Wikimedia Commons
The turning point arrived in January 2025 in Vellore, India. Thirty-nine international experts convened to review the metabolic data and unanimously agreed that this distinct, non-autoimmune condition needed its own classification. They drafted the Vellore Declaration, leading directly to the International Diabetes Federation’s historic announcement months later.
The International Diabetes Federation immediately launched a type 5 diabetes working group, appointing Hawkins as the chair. The group is currently developing strict diagnostic criteria, building therapeutic guidelines, and establishing a global research registry. The scope of the crisis reaches far beyond Asia and Africa as cases have also been reported in parts of Latin America and the Caribbean.
“I’m hopeful that this formal recognition as type 5 diabetes will lead to progress against this long-neglected disease that severely debilitates people and is often fatal,” Hawkins stated.
The recognition of type 5 diabetes forces the medical community to confront the long-term metabolic consequences of undernutrition on the human body. Acknowledging the disease is merely the first step.
“There is no quick fix, and so we expect the fight against this disease to require substantial further research and advocacy,” Hawkins said. “Once you have seen young patients dying from inappropriate treatment of a neglected form of diabetes, there’s no turning back.”