Arthur Ransom was a history maker before he was born. The boy was the size of an avocado, still in his mother’s womb, when he became the UK’s youngest ever blood transfusion patient.
Arthur’s mother, Maisie Ransom, was 16 weeks pregnant when her baby developed a life-threatening infection that caused his organs to begin shutting down due to a lack of oxygen.
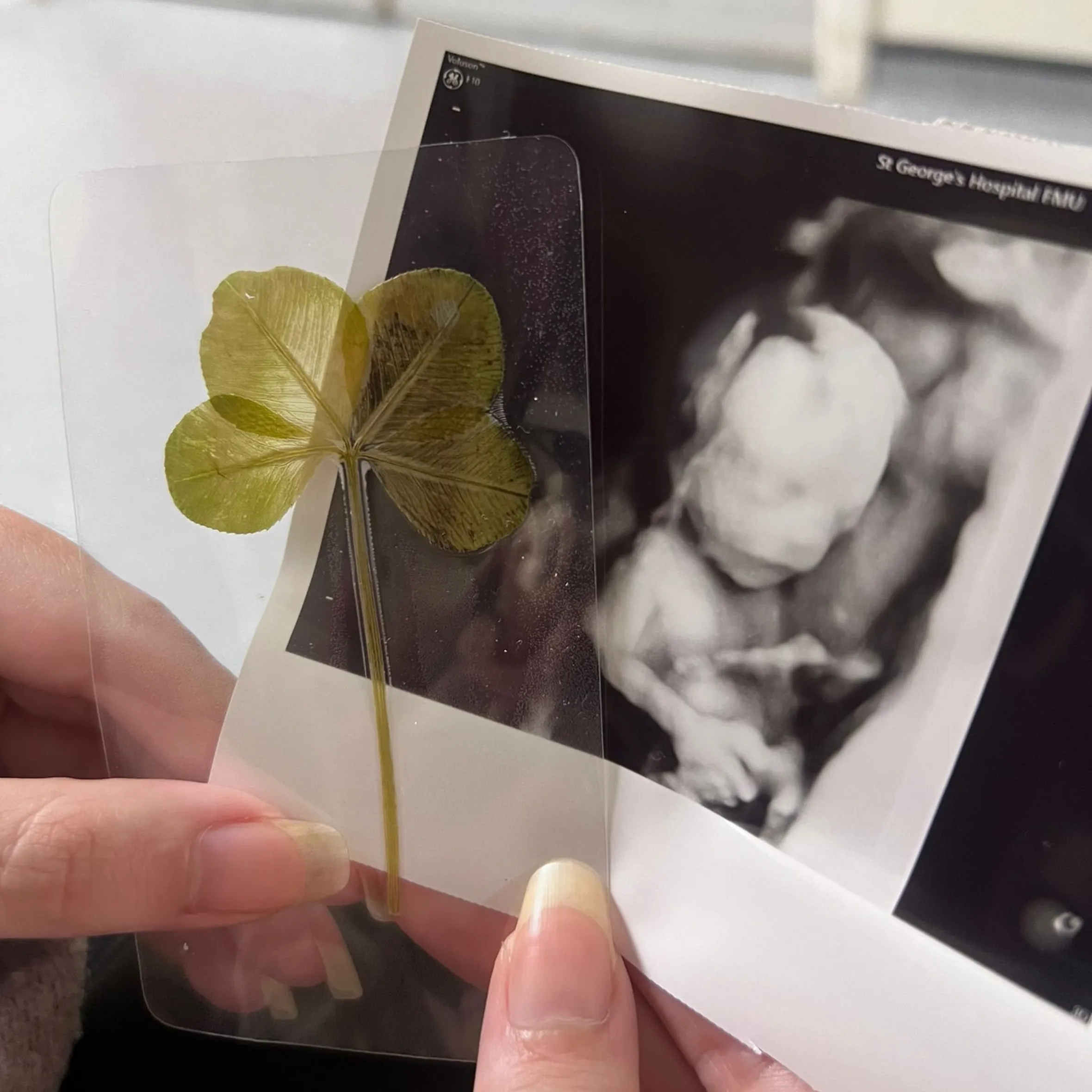
The only hope of survival for Arthur was a rare and high-risk procedure called an intrauterine transfusion (IUT), relying on blood from NHS donors. Doctors use a needle to transfuse concentrated red blood cells directly through the uterus and into the baby.
 Maisie and Keith RansomPA
Maisie and Keith RansomPA
“He was so small the doctors were working within millimetres,” recalled Ransom, who had the procedure in 2024 at St George’s Hospital in London. “The experience was absolutely terrifying. The doctor said it was 50/50 whether he would make it or not.
“The doctor had to be incredibly precise and I am still baffled at what she was able to do in that room. There were a lot of people. It took a lot of skill and steady nerves. The room was silent other than when the lead surgeon was speaking. Once the procedure was over it felt like everyone was frozen, waiting to see if he would survive that initial step.”
The blood delivered oxygen to Arthur’s body, meaning the fluid that had surrounded his heart and organs could be reabsorbed and normal function could resume. He was born in January last year and is now a “really chirpy little” one-year-old who has reached all his key milestones.
“Without that blood he would not have made it — his organs were failing, his heart was completely enveloped in fluid and it was struggling to pump,” Ransom, 30, a primary school teacher from Cranleigh in Surrey, said.
“If nothing was done, he would not have made it much longer. The doctor said to the best of her knowledge there was no one younger to get an intrauterine transfusion.”
The NHS performs fewer than 200 IUTs on babies per year who have severe anaemia, the condition where a person has a lack of red blood cells that carry oxygen around the body. They are usually not performed until 18 weeks of pregnancy, as before then babies are too small.
Arthur’s anaemia was caused by an infection called parvovirus, which is usually harmless to children but can cause severe illness in unborn babies.
Ransom, who is married to Keith, 36, added: “Arthur’s doing great now. He’s a really chirpy little boy, reaching all the milestones. He’s very handsome and developing normally. He keeps us on our toes. I think every day about how lucky I am.”
 PA
PA
She said that there were “no words to express the gratitude” she has for the blood donors who had “given my boy the chance to be here”.
The blood used in IUTs is provided by NHS Blood and Transplant (NHSBT), which specially selects it from donors who meet several strict criteria. Donors need to be men and have type O blood which is “Kell negative”. Their blood is made into small packs of extremely concentrated red cells, which are then transfused via needle and guided by ultrasound, usually into a vessel in the umbilical cord.
Dr Luci Etheridge, consultant paediatrician and chief medical officer at St George’s, said: “For babies like Arthur, a blood transfusion while still in the womb can mean the difference between life and loss.”
Dr Anne Kelly, paediatric transfusion and components clinical expert for NHSBT, said: “Intrauterine transfusions are very rare. They are only done in specialised units when absolutely needed to help save a life. While they can be given as late as 34-35 weeks gestation, most are given earlier. The procedure is carried out under continuous ultrasound guidance.”
NHSBT has identified eight blood donors whose blood has been used three times each to make blood for this special type of transfusion.
Paul Bickley, 45, who has been identified as one of the men who has donated the most for IUT procedures, said he started donating blood because of his mother’s “generous heart”.
 Paul BickleyPA
Paul BickleyPA
The father of four from Richmond, southwest London, who is a vice-president of an insurance company, said: “I started donating because my mum and dad donate. My mum told me it is a good thing to do to give back literally and metaphorically to society.
“She just has a generous heart. As the years went on and we had our own children I just realised life is very precious and that kept me donating. Hearing my blood was used in this way almost made me cry. To think a very small act of kindness on my part could have such a massive impact. It was mind-blowing and miraculous.”
David Smith, 64, from Westminster, has also been identified as a donor whose blood has been used the most for these specialist transfusions.
 David SmithPA
David SmithPA
The retired heating and ventilation engineer, who has donated more than 80 times overall, said: “You can’t not do it if you can help babies. You have to. It’s always a pleasure to donate, whether it’s used for babies or for anyone.”
Graeme Kay, 70, a classical music journalist, choir conductor and former BBC Radio 3 and 4 music producer, from Orford in Suffolk, has donated more than 60 times.
He said: “I find it quite relaxing to donate. Once the needle is in, you can do nothing except look at your phone or daydream. The whole environment is really nurturing, being with the donation team and seeing other people stepping in to donate.
“Knowing you are helping an unborn baby does add extra value to the feeling of donating. It makes you feel good. It’s amazing to know my blood has been used for this the joint most in the country.”

