
Outside Wellington Hospital. (File photo)
Photo: RNZ / REECE BAKER
Healthcare staff in Wellington’s Emergency Department will have to wait until 2029 for a bigger space, with one nurse describing corridors crowded with patients waiting for beds.
Renovations to add much-needed space to the ED were underway, as Health New Zealand worked to increase the capacity of the already stretched department by 34 “points of care” – that is, a combination of bed spaces, resus rooms, consult rooms, and treatment spaces – taking it from 53 to 87.
One New Zealand Nurses Organisation (NZNO) delegate, who didn’t want to be named, said the main problem was space.
“It’s too small. We get to the point where we can’t move. Corridors are full. We’ve had up to 26 patients in the corridor – that’s a lot of patients. That’s more than the little areas we see people in.”
ED’s weren’t allowed to turn anyone away, they said, no matter how full the department got – but sometimes, although they were not supposed to, staff would give ambulances a heads up that it might be some time before they could offload patients, and if there was anywhere else they could take them, they should do so.
“Our Wellington [patients] wouldn’t like to go out [to the Hutt] because they might not have any way to get back,” they said.
“If it’s an ambulance that’s taken them out there, and they’ve got no family, that can be a bit hard.”
The delegate hoped the renovations would mean parts that were spread out would be brought closer together – observation and pediatrics beds, even perhaps a mental health area.
The new ED was part of a $1 billion hospital-wide upgrade announced in Budget 2025, with the ED expected to open in 2029.
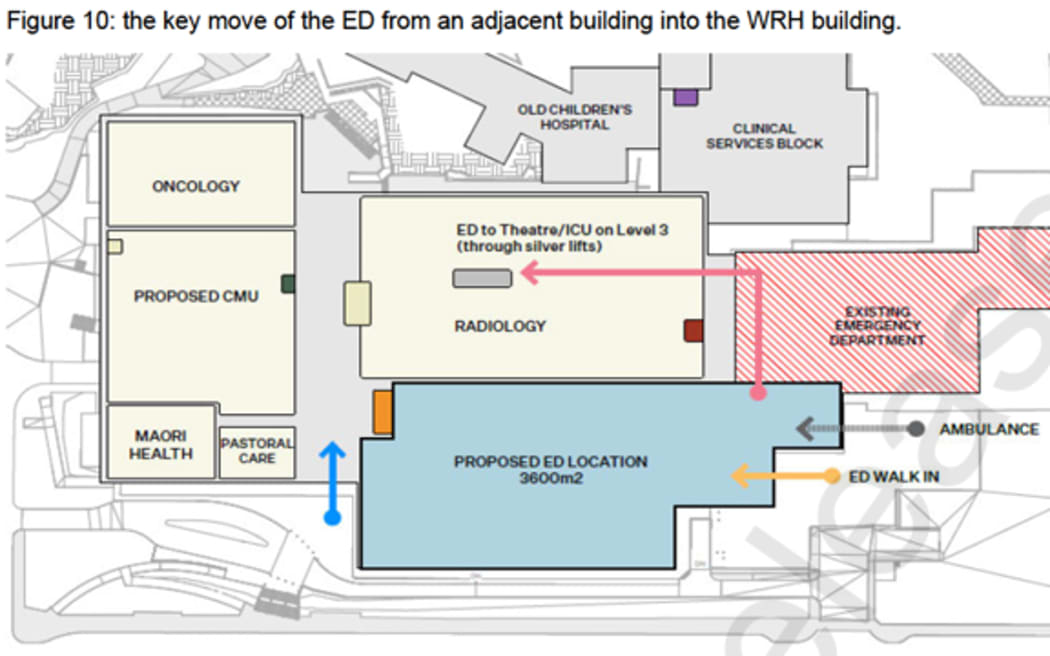
The plan for Wellington Hospital’s emergency department.
Photo: HEALTH NZ / SUPPLIED
Health NZ’s group director of operations for Capital, Coast and Hutt Valley, Jamie Duncan, said the “front of whare” refurbishment was progressing well.
The ED was to be moved within the main hospital building, with renovations underway elsewhere in the hospital to make space.
A number of both clinical and non-clinical spaces were being relocated, Duncan said, but the work should improve other acute clinical spaces, too.
According to Health NZ, work underway at the moment included:
Refurbishment of levels 6 and 7 of the Grace Neill Block in preparation for the relocation of the main Outpatients Department and other clinical services
Construction of a new main reception area and a new Security Orderly Service base
Creation of a new and improved Medical Assessment and Planning Unit (MAPU) to support patient flow throughout the wider hospital
Future work included the expansion of MAPU, along with the Surgical Assessment and Planning Unit (SAPU), and the Intensive Care Unit (ICU) to further increase inpatient capacity.
The case for more space
Documents from as far back as December 2021, when Health NZ was still operating as separate District Health Boards, detailed the need for a “front of whare” project to address the lack of capacity.
Between October and January this year, Wellington Hospital’s ED went into its most critical code red status on average nearly twice a day (code red means hospital occupancy is forecast to exceed 100 percent – it does not indicate services are closed).
The detailed business case for the hospital upgrades, dated October 2024, said “without progressing the project, the hospital’s ED is in an unsustainable situation and will continue to be unable to meet the health needs of the region”.
“The ED is clinically and culturally unsafe, spaces are cramped, inadequately designed, fragmented and inefficient. Around 1/3 of patients are receiving treatment in a corridor. It is difficult to maintain consultant supervision and oversight of patients in five different areas,” it reads.
One of the government’s health targets – 95 percent of patients to be admitted, discharged or transferred from an emergency department within 6 hours – would not be met without this work, it said.
One in ten people, facing long queues, did not wait to be seen by a clinician – making them more likely to come back later in a worse condition.
A lack of beds elsewhere in the hospital meant people were stuck in ED, taking up those beds.
Seismic assessments rated the current ED at 15 percent of the National Building Standard (NBS). Some strengthening work had increased that to 34 percent, but that was still below the recommended rating 67 percent.
Duncan said since the time of the report’s writing, HNZ remained focused on improving wait times.
“The significant work and investment made in this area has seen Wellington Regional Hospital’s performance against the Shorter Stays in ED (SSED) target improve by 11.6 percent points between January and December 2025 – a testament to the ongoing hard work and professionalism of our dedicated and fantastic staff,” he said.
But at the same time, there was growing demand for services and patients with more complex and acute needs.
“We acknowledge that there is still a long way to go and much work to do – however people can remain assured that ED is the safest place for them when experiencing a healthcare emergency, and that we remain committed to doing all we can to continue responding to the needs of our communities.”
Sign up for Ngā Pitopito Kōrero, a daily newsletter curated by our editors and delivered straight to your inbox every weekday.

