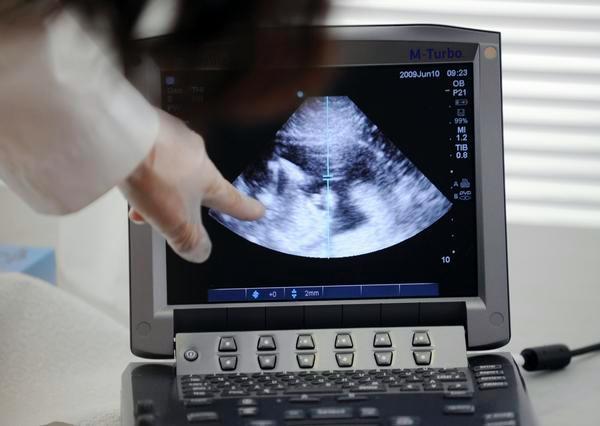
A Denver company has received federal approval to market an artificial intelligence program it says can predict when babies will arrive based on their ultrasounds, raising the possibility of flagging premature births.
Delivery Date AI predicts when a baby will be born, with an 11-day margin of error in either direction, based on second- and third-trimester ultrasounds.
While the U.S. Food and Drug Administration doesn’t allow maker Ultrasound AI to advertise the product as a premature birth detector, an earlier-than-expected predicted birth date would signal to parents and their doctor that the baby might arrive sooner than is optimal.
The FDA process for approving relatively low-risk medical devices requires the manufacturer to show that it works as promised and to collect data about any adverse effects when providers begin using it. Companies don’t have to prove that patients treated with it fared better than those who weren’t.
About one in 10 Colorado babies is born prematurely, which is in line with the national average, according to the March of Dimes. Black and Native American women are at higher risk, even if they are healthy.
Babies born prematurely are at an elevated risk of lung problems and infections in their first months of life. They also have increased odds of disabilities as they grow, including hearing or vision problems.
The American College of Obstetricians and Gynecologists defines a full-term pregnancy as 39 to 40 weeks, dated from the mother’s last menstrual period before conception. With current technology, babies have a slim chance of survival at 21 weeks, with the odds that they’ll live to go home rising as they get closer to full-term.
The AI was trained on millions of ultrasound images from the University of Kentucky that had information about how long the pregnancy lasted, with the patients’ personal data removed.
Eventually, it found eight measures that correlated with how long a pregnancy would last, including seven that human experts hadn’t previously linked to preterm birth, founder Robert Bunn said. Those included abnormalities in the mother’s placenta, uterus and ovaries, as well as the fetus’s kidneys and heart rate, he said.
One of the problems, an unusually fast fetal heart rate, specifically correlated with early induced births because the mothers developed high blood pressure during pregnancy, known as preeclampsia, Bunn said. While it isn’t approved to predict preeclampsia at this point, the AI could eventually help flag which patients need more monitoring or preventive treatment, such as low-dose aspirin, he said.
“We’re going to save the lives of mothers in the future, too,” he said.
Obstetricians already check for the eighth measure, which is the length of the bottom of the uterus, or cervix. The cervix shortens and opens as birth approaches, so doctors sometimes use a stitch to keep it closed in patients at high risk for premature birth.
A tool that could reliably predict when babies will be born would be extremely valuable in obstetrics care, said Dr. Nicholas Behrendt, who works in the neonatal intensive care unit and treats mothers carrying babies with relatively rare high-risk conditions at Children’s Hospital Colorado. He isn’t sure if the AI is ready for routine clinical use as-is, but thinks its predictions will keep improving over time.
Now, providers go down a list of common risk factors to identify which pregnancies need more monitoring, but they aren’t perfect predictors, Behrendt said. Patients with many risk factors may have uneventful pregnancies, while others who seem perfectly healthy have dangerously early deliveries, he said.
“We know it’s more complicated than a cervix issue,” he said.
Doctors can only delay a preterm birth by a day or two, but that allows them to give the mother steroids, which speed up the fetus’s lung development, Behrendt said. It can also buy time for families that live in areas without a neonatal intensive care unit to transfer to a hospital that can give the baby their best shot at survival and good outcomes, he said.
“If we can get better at predicting (preterm birth), we can potentially improve neonatal outcomes,” he said.
Providers may not immediately have treatments specific to the newly flagged risk factors, but knowing about them will open up research opportunities, Bunn said. Right now, the primary recommendations for preventing preterm birth are getting checked for certain infections and avoiding smoking, alcohol and other drugs — not terribly useful to patients who’ve had a premature birth despite a healthy lifestyle.
The FDA approval allows providers to use the AI with adult patients between 14 and 37 weeks of pregnancy with a single fetus that doesn’t have any known anomalies, such as an irregular number of chromosomes. For a typical patient, the AI scan would cost $100 to $200, Bunn said.
The product is new enough that insurers likely haven’t decided whether to cover it.
Typically, doctors don’t attempt to predict a baby’s birth date, beyond the “due date” of 40 weeks past the mother’s last period. A study from Australia found about one in 20 babies arrives on their due date, though more than half make their debut within a week before or after the expected date.
They often check the cervix for signs that labor is near as the anticipated end of pregnancy approaches, but those also aren’t a perfect indicator. Some women give birth within a few days of an exam that finds no evidence their cervixes are starting to open.
Bunn had previously used AI to search for new sources of oil underground, but pivoted to medical work after his wife had a series of miscarriages. They’ve since had five children.
When he started a decade ago, doctors didn’t think ultrasounds could offer meaningful information about premature birth, though they started to come on board and help improve the AI after it found risk factors they hadn’t expected, he said.
“Humans can’t sit there and learn from millions and millions of images” in the way that AI can, he said.
Risk factors for preterm birth include:
Previous early deliveries
Carrying twins or triplets
Having a short cervix (the lower portion of the uterus)
Conceiving via in-vitro fertilization
Certain infections, including sexually transmitted ones
High blood pressure or blood-clotting problems
Having obesity or being underweight at the start of pregnancy
Conceiving again within six months of a birth
Having diabetes
Being younger than 18 or older than 35
Skipping prenatal care
Smoking
Drinking alcohol
Using illicit drugs
Experiencing domestic violence
Working a physically demanding job
Having exposure to unsafe chemicals or radiation
Experiencing high levels of stress
Source: National Institute of Child Health and Human Development
Sign up for our weekly newsletter to get health news sent straight to your inbox.