 Image: © SimoneN | iStock
Image: © SimoneN | iStock
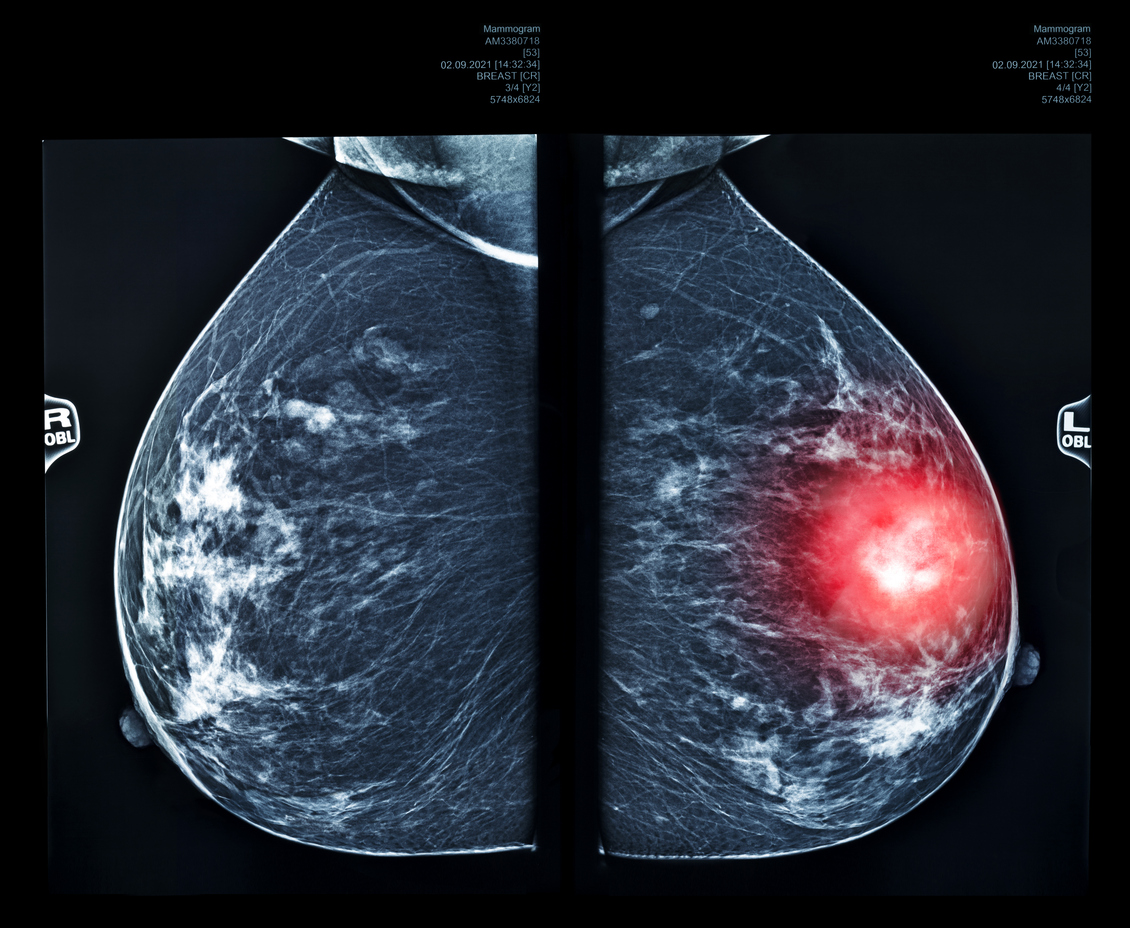
New research from Imperial College London shows Google AI can match or exceed radiologists in detecting breast cancer from mammogram scans, highlighting its potential to improve screening and early diagnosis
New research from Imperial College London has found that a Google-developed artificial intelligence system can match, and in some cases exceed, radiologists in detecting breast cancer on mammogram scans. The study suggests that AI could improve screening accuracy and support doctors by identifying subtle cancer signs that might otherwise be missed, potentially speeding up diagnoses and easing pressure on healthcare services.
The findings are published in two linked papers in Nature Cancer.
Breast cancer: One woman is diagnosed every ten minutes
In the UK, breast cancer scans are assessed by two readers, usually specialist radiologists. Each reads the scan separately, with the second reader either knowing or not knowing the first reader’s decision.
The latest study compared two human readers with one human reader and one AI reader, using AI software developed by Google.
Groundbreaking AI study: Transforming breast cancer screening
In the largest NHS study to date, 175,000 women participated in a three-part trial evaluating the use of AI in breast cancer screening.
The first study involved 125,000 women, aged 50 to 70, from five NHS screening services. They were screened in 2015-16 over a 39-month follow-up period. The final analysis included 115,973 breast cancer scans.
The researchers found that AI, as the second reader, achieved better results than the first human reader, with the cancer detection rate (CDR) rising from 7.54 (human) to 9.33 (AI) per 1,000 women.
AI also identified more invasive cancers, significantly reduced false positives, and detected 25 per cent of interval cancers (cancers detected between healthy scans).
AI performed particularly well for first screens – with 39.3% fewer recalls and an 8.8%. With AI, the time taken to read a scan was reduced by almost a third (32.1 per cent, or 195,983 vs 288,616 reads), representing a significant reduction in workload.in workload.
The second part of the study examined 9,266 current cases from two screening services at 12 sites in London.
During the first two weeks, AI achieved a higher recall rate than humans and exceeded the study’s target, prompting the researchers to adjust the criteria. Despite this, AI maintained a higher recall rate. Furthermore, across both sites, the average time for AI to complete a read was 17.7 mins, compared to 2.08 days for the first human reader, a significant time-saving.
The third part of the study looked at the use of AI in arbitration in 50,000 women. Arbitration is when the first and second readers disagree on the diagnosis, and a third reader analyses and makes a final decision. The AI tool had a higher arbitration rate, but reduced the overall screening workload.
“This is the closest AI has ever come to helping reduce breast cancer deaths within the NHS, so the potential for the NHS to take this forward is significant, particularly in light of the National Cancer Plan for England’s recognition that ‘there are few clearer signs of the failure of the status quo than our inadequate cancer outcomes’ and its appetite to embrace new technologies to address that,” added Dr Hutan Ashrafian, Institute of Global Health Innovation, author on both papers.
Dr Susan Thomas, Clinical Director at Google and an author on both papers, added: “Early detection is our most powerful tool in the fight against breast cancer, and these findings mark a genuine turning point.
“This is the first time that we’ve been able to rigorously test doctors and AI working alongside each other in a clinical setting.
“These findings have the potential to support the transformation of the NHS, and the experiences of the people on both sides of the scan, bringing us one step closer to a future where this technology strengthens entire healthcare systems and, ultimately, saves lives.”
Professor Deborah Cunningham, a consultant radiologist at Imperial College Healthcare NHS Trust and another author, added: “This study provides good evidence for the potential use of AI in the real world of screening mammography, where staffing is particularly difficult. Its introduction could provide support for the successful NHS breast screening programme, reducing breast cancer mortality.
“The time saved will free up radiologists to perform more hands-on tasks such as needle biopsy, an essential part of the cancer diagnostic pathway. This should not be regarded as a threat to radiologists’ livelihood, rather an opportunity to allow us to spend more time deploying our skills and working with colleagues and patients to improve cancer diagnosis and outcomes.”