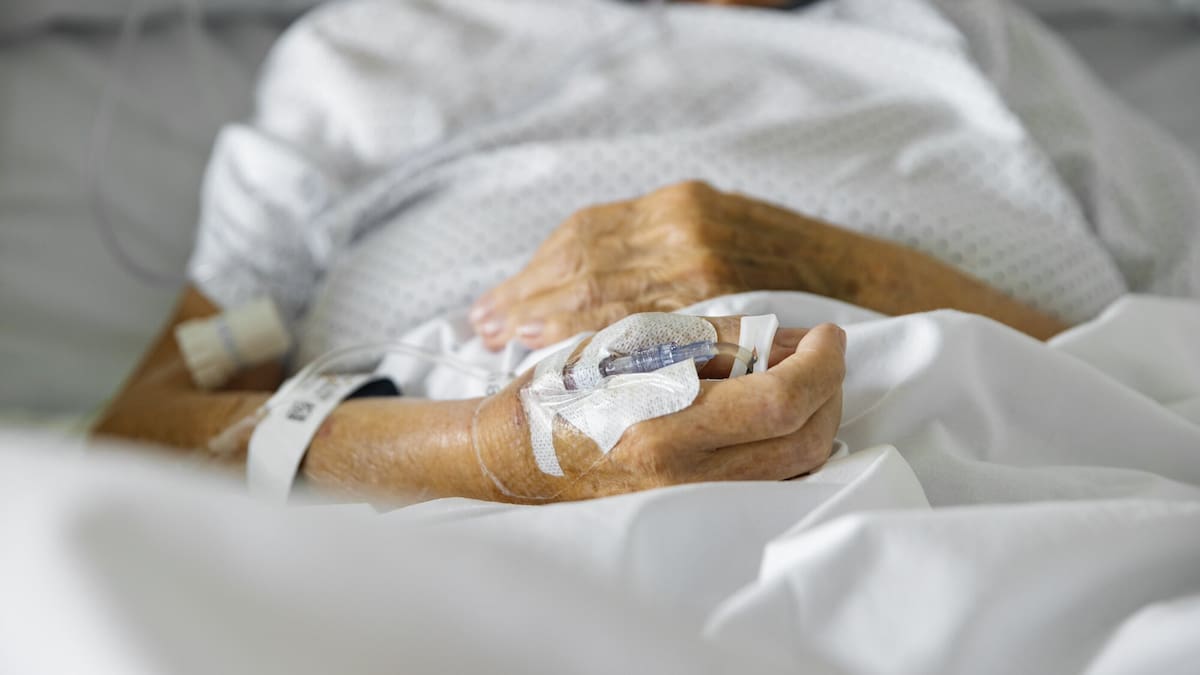
“Hospitals can be really dangerous places for older people,” says geriatrician Dr Cheryl Johnson.
It is a confronting statement, but anyone who has spent time around frail older patients will understand exactly what she means. The risk is often not the illness or injury that brought someone to hospital in the first place. It is what happens next.
An older person arrives unwell but is still functioning. Then, almost immediately, their normal routine disappears. Meals arrive on trays. Walking is reduced to the distance between the bed and the bathroom. Long stretches of the day are spent lying down while tests are run, medications are adjusted and observations are taken. It can look like rest. But the body experiences it differently.
In geriatric medicine there is a term for what follows: deconditioning.
Muscles that are not used weaken quickly, and older bodies lose strength faster than younger ones. A few days in bed can be enough to change how safely someone walks, whether they can stand from a chair unaided, or whether they can manage the basic tasks of daily life. Johnson sees this all the time on rehabilitation wards, where older adults are transferred once the acute phase has passed.
“We take older adults who have been through the acute wards because they’re weak and not walking well,” she says. “Our job is to try to get them back on their feet again.”
But lost strength is not always easily regained. It can take weeks or months to come back – sometimes it doesn’t come back at all. This is why hospitalisation can become a turning point.
Hannah McQueen. Photo / Michael Craig
Families understandably focus on the infection, the fracture, the fall or the stroke that caused the admission. But the more important question often becomes whether that person will still be able to function well enough to return home afterwards. If mobility and independence decline too far, home may no longer be considered safe. That is when the conversation shifts from recovery to care, and how a hospital stay can become the road to the rest home.
It’s often not one dramatic, single moment, but a series of small losses that accumulate while someone is in a hospital bed, out of routine, not sleeping properly, not moving enough, and exposed to risks that younger patients may weather more easily.
Families do not always see that risk clearly. Johnson says it is common for relatives to ask for “just another week” in hospital, assuming more time there will help their parent recover before going home. But she has often seen the opposite. She says “that extra week can mean an infection picked up from the ward. It can mean another week of muscle loss, another week of reduced mobility, another week further away from independence”.
Hospitals are, after all, full of infections. Respiratory viruses, winter illnesses and antibiotic-resistant bugs are part of the hospital landscape. For younger people, these may be a complication. For older adults, especially those already frail, they can be a major setback. Johnson’s point is not that hospitals are unsafe because people are careless. It is that older bodies have less margin for error.
Dr Cheryl Johnson, Geriatrician.
Then there is delirium, one of the most distressing complications of hospitalisation in older adults.
Delirium is a sudden state of confusion that can develop during illness or hospital stays. It can appear quickly and be frightening for families to witness. A previously sharp parent may suddenly seem agitated, disoriented, suspicious or unable to recognise familiar faces. It is often mistaken for dementia, but delirium is different. It is usually triggered by a combination of factors: illness, infection, medications, dehydration, lack of sleep, and disruption to normal routines.
And hospitals, by their nature, disrupt routines.
Older adults are removed from familiar surroundings and placed in busy wards filled with unfamiliar sounds, faces and interruptions. They may be woken throughout the night for observations or tests. Sleep becomes fragmented. Days and nights blur. For older brains, that kind of disruption can be profound.
Sleep deprivation is an underappreciated part of the problem. Hospitals are rarely restful places. Alarms sound. Lights switch on. Staff move between beds. Patients share rooms with people who are also unwell. For younger people, poor sleep is unpleasant. For older people, it can contribute to confusion, weakness and a much greater risk of falling. Another hazard in plain sight.
Medications commonly used in hospital, including sedatives and strong pain relief, can affect balance. Add weakness, poor sleep and confusion, and the risk climbs quickly. Research has shown that patients who are moved between wards multiple times during a hospital stay are significantly more likely to experience adverse events and have longer stays, reinforcing how destabilising the hospital environment itself can be.
None of this is an argument against hospitals. When serious illness or injury strikes, they remain the safest place to be. But geriatric medicine increasingly recognises that older adults often recover best once the immediate crisis has passed and they are back in familiar surroundings.
“Success,” Johnson says, “would be managing more care in the community and supporting people where they function best – in their own homes.”
That makes intuitive sense. At home, people move more, sleep better and follow familiar routines. They maintain a sense of agency and the ordinary demands of daily life – making a cup of tea, getting dressed, walking to the letterbox – become part of recovery, rather than something postponed until later.
Hospitals will always play an essential role in healthcare. But when it comes to ageing well, the goal is often not simply surviving a hospital stay. It’s avoiding one wherever possible.
Because for many older adults, the admission that begins with something small – a fall, a fever, a wobble that didn’t seem like much at the time – can become the moment everything after starts to look different.
Cheryl Johnson’s top tips for avoiding hospital admissions
Review medications carefully. When starting a new medication, ask your doctor about possible side effects and interactions with current medicines, as new prescriptions can sometimes lead to harm or hospital admission. If you take several medications, consider an independent medication review.
Keep vaccinations up to date (eg, shingles, influenza, Covid-19).
Act on new symptoms early – see your GP rather than waiting for them to worsen.
Protect bone health by assessing and managing fracture risk.
Get a comprehensive health assessment to identify risks early and improve health proactively.
Hannah McQueen is the founder of EnableMe and Age Brightly, and the host of The Next Bit podcast. Dr Cheryl Johnson is Age Brightly’s lead geriatrician.