The United States is grappling with a mental health crisis as rates of depression, anxiety and other conditions surge among Americans, particularly children and teens.
But most Houston residents live in “mental health deserts” where there are not enough providers to meet the demand for services, according to a study by University of Houston researchers.
More than 40% of Houston ZIP codes have no mental health providers, and the neighborhoods that lack access to those services typically have higher poverty rates and a greater share of minority residents.
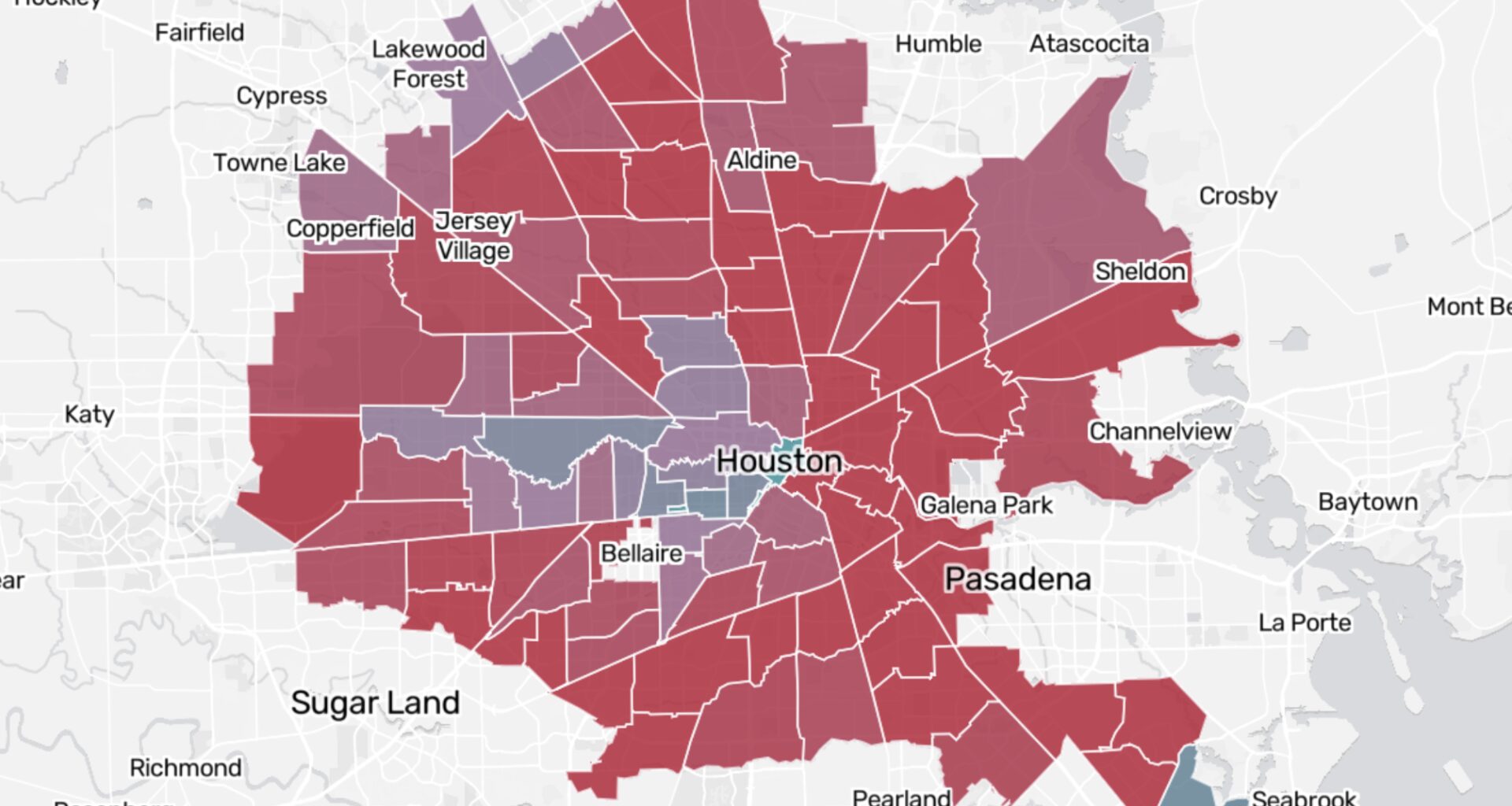
Most ZIP codes with more in-person providers per capita can be found on the west side, the western half of the Inner Loop and the areas just north and south of it — the area that forms the “Houston Arrow.”
Article continues below this ad
READ MORE: Houston leaders want to transform the city into a hub for brain health to spur economic growth
The study, published in the journal Frontiers of Public Health, highlights one of the many barriers that Houston residents may encounter while trying to access mental health care. It also illustrates how residents living in low-income communities are more likely to face obstacles compared to those living in prosperous neighborhoods.
Lead author Damien Kelly and senior author Chakema Carmack coined “mental health deserts” as a nod to “food deserts,” a term used to describe neighborhoods with limited access to nutritious and affordable food. They created a map of Houston’s mental health deserts for the study they conducted at UH’s HEALTH Center for Addictions Research and Cancer Prevention.
Article continues below this ad
“We were not surprised, but it was still startling to see it in black and white,” said Carmack, an associate professor in the department of psychological, health, and learning sciences at UH’s College of Education. “Us being mental health professionals and working in that line of work for the past 20 years, it was kind of jarring to see that in (Houston).”
The researchers shared the data from their study with the Chronicle, which used the data to produce its own map of Houston’s mental health deserts.
Living far away from any mental health providers can be a significant deterrent, along with other issues such as cost and a lack of transportation, said Angelina Hudson, the executive director for the National Alliance on Mental Illness’ Greater Houston affiliate.
Driving or taking public transportation to therapy can be more difficult for someone with a mental health disorder, or for a parent or guardian with more than one child, Hudson said.
“There’s no way in the world a (parent) with five children is going to take their kid all the way across town,” she said. “What are they going to do with the other kids?”
Article continues below this ad
What the data shows
In their research, Kelly and Carmack juxtaposed mental health provider availability with the socio-economic characteristics of Houston’s ZIP codes by using the Distressed Communities Index. The index takes census information about poverty rates, average educational attainment, and business development in a ZIP code to label the community on a scale from “prosperous” to “distressed.”
Stark differences emerge. Over half of “distressed” and “at-risk” ZIP codes have zero mental health providers, but the same is true for only about 17% of “prosperous” and “comfortable” ZIP codes.
READ MORE: UTHealth researchers hope lab-grown mini brains reveal clues about cause of schizophrenia
Article continues below this ad
The Chronicle also found similar trends when looking at race. Almost half of majority-minority ZIP codes — where racial minorities make up more than 50% of the population — have no mental health providers. On the other hand, only about 10% of majority-white ZIP codes have no providers.
Take, for example, the “prosperous” ZIP code 77024, which consists of Memorial Park and Greater Uptown, and the “distressed” ZIP code 77092, which includes the Fairbanks/Northwest Crossing neighborhood in northwest Houston.
Both ZIP codes have similar populations and sit west of downtown. But 32 mental health providers practice in 77024, while zero are in 77092.
Nearly nine out of 10 distressed ZIP codes like 77092 have fewer mental health providers than the average Houston ZIP code. Again, a similar trend is true for majority-minority ZIP codes, two-thirds of which have fewer providers than the average.
Article continues below this ad
Not all ZIP codes follow these trends, though. Downtown Houston — ZIP code 77002 — is “distressed” based on its socio-economic indicators, but has 32 providers, the most of any ZIP code in the metro area.
Kelly and Carmack explained that providers might choose to practice downtown due to its central location, and pointed to a large facility there, St. Joseph Center for Behavioral Health, that increases the number of providers in this area.
Limited access to telehealth
While many people benefit from telehealth, it may not be an ideal solution for residents in low-income communities who may not have reliable internet access or a computer or tablet they can use to meet with a provider, Kelly and Carmack said.
The availability of telehealth may also depend on someone’s insurance plan. Some providers do not accept Medicaid or plans that are more affordable but offer less coverage, which may be more common in lower-income areas, Kelly said.
READ MORE: Social media is ubiquitous among teens, but experts say it might pose risks to their mental health
Telehealth has other limitations, too. Someone in an abusive relationship may be unable to discuss their situation with a provider if the abuser can hear their conversation, Kelly said.
Providers also tend to form stronger connections with patients and observe clues about their mental health when they meet in person, Hudson said.
“There’s a lot to healing and recovery that doesn’t come from words. Sometimes it’s a nod. Sometimes it’s a sigh. Sometimes it’s the tapping of a foot,” she said. “You don’t get the full communication through a screen.”
Additional research in Houston
The map of Houston’s mental health deserts is intended to help community leaders and policymakers address disparities in accessing treatment, the researchers said.
Kelly and Carmack are now working with Harris County Precinct 4 Commissioner Lesley Briones’s office to conduct more research and develop policy recommendations for improving access to mental health care.
The partners are creating a dashboard that will provide information about mental health care available in Precinct 4 neighborhoods when it is released publicly within the next few months. They also held community meetings where residents cited cost, transportation and language differences as barriers to care, Briones said.
“It reinforced what we were seeing on the ground,” Briones said. “And frankly it just made us want to focus even further and deepen our commitment to expanding access to mental health care.”
Kelly and Carmack said they hope to work with other Houston and Harris County leaders on similar projects in the future.
Other barriers to mental health care
While proximity to a mental health provider can be a significant barrier to treatment, researchers and experts said other factors also play important roles.
Even if a provider is available nearby, parents or guardians may still need to take time off work to bring a child to an appointment, or find child care for their other children, Kelly and Carmack said. The cost of treatment can also be prohibitive for people who are uninsured or underinsured.
“If you need a therapy session every week, that can be very costly. And insurance doesn’t cover a lot of those (services),” Kelly said. “So there’s still lots of work that needs to be done in these areas.”
The UH study includes several recommendations for improving access to care, such as stipends for providers to practice in underserved areas and insurance reforms to cover the cost of transportation. They acknowledged that securing funding for those recommendations could be difficult, as the budgets for the city of Houston and Harris County are already strained.
However, Kelly and Carmack believe the recommendations could have broad community benefit, as studies have found mental health disorders can have a significant economic impact. Treatment can be costly, and indirect costs – such as the effects on a community’s workforce – can also be substantial.
Hudson, from NAMI Greater Houston, noted that improving access to services won’t fully address the problem. While attitudes toward seeking treatment have evolved over time, many people remain hesitant to do so, she said.
Still, she believes eliminating barriers to mental health care, either by enticing providers to practice in underserved areas or through other means, would benefit Houston residents who currently struggle to access treatment.
“Let’s just keep chipping away at the different barriers to access,” she said. “(Proximity) is one of them.”
About the data in this story
The data shown on this page was provided by the University of Houston and was sourced from a peer-reviewed study conducted at UH’s HEALTH Center for Addictions Research and Cancer Prevention. The researchers identified public and private mental health providers in Houston using Psychology Today’s database. The data was accessed by UH researchers in November 2024.
Distressed Community Index data for Houston ZIP codes was also provided to the Houston Chronicle by UH. The index was created by the Economic Innovation Group to measure economic disparities in U.S. communities and uses U.S. Census data.
Population counts for each ZIP code were sourced directly from the Census.