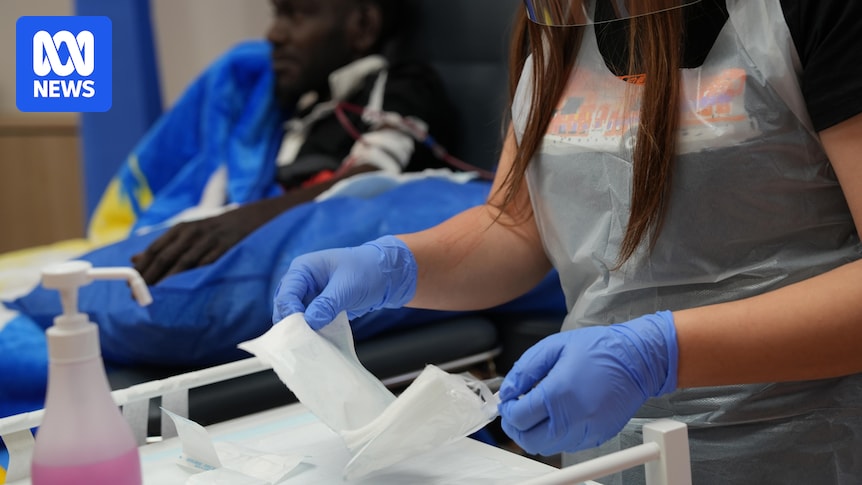
An outback doctor says GPs are being forced to wait more than a month in some cases for critical patient information, putting lives at risk.
Although patient histories and medication notes are now digital, most medical information is managed by each region’s hospital and health service and often hidden to other doctors.
Gidgee Healing chief executive Dr Manjit Sekhon said doctors have been left waiting for essential clinical handovers and denied access to basic patient information due to privacy barriers.

Manjit Sekhon believes doctors are flying blind and patients are at risk under the current information sharing systems. (ABC North West Qld: Tim Little)
“There’s quite often a delay in receiving clinical correspondence. I’m talking a few weeks, over a month at times,” Dr Sekhon said.
“You’re hiding patients’ data from health care professionals.
“It puts patients at risk and just leads to unnecessary interventions.”
‘Data belongs to the patient’
Dr Sekhon said GPs rely on discharge summaries and specialist notes to understand a patient’s condition, treatment and next steps.
But in regional areas that information often comes too late to treat the patient while they are in the clinic.
The experienced GP believed local hospital health services did exceptional work but were hamstrung by Queensland Health systems.
“We’ve got no visibility. We rely on receiving that letter [discharge summary] to get any information out on the patient,” Dr Sekhon said.
“What’s the matter with accessing that data which at the end of the day belongs to a patient?”
A 2025 study published in the BMC Health Services Research journal found patient data transfers and data access affected the entire Queensland health system.
But Rural Doctors Association of Queensland president and Longreach GP David Walker said regional doctors felt the burden more heavily because they saw a higher number of travelling patients, and those who rarely seek healthcare.

David Walker said it was common to see patients without records months after specialist and hospital visits. (Supplied: Central West and South West Hospital and Health Service)
“It affects us as rural GPs far more than probably our urban counterparts,” he said.
“There’s a variety of things that people need to travel for — whether that’s for planned admissions or for emergencies, and then when they come back.
“But it’s often a challenge for us to work out what exactly happened during that stay.
“It is often days or weeks or sometimes months before discharge summaries come back to the treating GP.”
Queensland Health already uses online systems that make some information available to GPs and healthcare workers in real time.
Some medicine scripts can be access through a portal called Qscript, while imaging, emergency department records and some referrals are on The Viewer platform.

Digital infrastructure enables information exchange across monitored medicines and clinical correspondence. (
ABC News: Matt Roberts
)
A Queensland Health spokesperson acknowledged information sharing was an issue across the state, and plans to improve current systems were underway.
“We recognise that seamless information sharing is essential, particularly in rural and remote communities,” the spokesperson said.
“Statewide digital programs, including integrated medical record systems and The Viewer, are helping to improve sharing of critical patient information from HHSs (hospital and health services) to eligible external healthcare practitioners such as GPs.”
A spokesperson for the Northwest Hospital Health Service did not believe delays in data transfers or access was a “widespread or systemic issue.”
‘No-one has ever died from a data leak’
Dr Walker said even with those digital portals, information was slow to be uploaded or, in the case of many specialists, hidden behind privacy barriers.
“There’s been plenty of times when you’ve got a patient back and they tell you they’ve had an appointment with a specialist last week … or even six months ago and there’s nothing to be found,” he said.
The Viewer platform allows for real-time data sharing, but some GPs say information often isn’t uploaded. (Supplied: Queensland Health)
Director of the Queensland Digital Health Centre at the University of Queensland, Professor Clair Sullivan, said the infrastructure was there but some attitudes towards patient data needed an update.
“Data is power. The traditional medical model was it was held in a filing cabinet in the doctor’s office and you only got to see it with special permission,” Professor Sullivan said.
“Going from a paper filing cabinet to a digital filing cabinet isn’t digital transformation.
“We need to think about it from the consumer’s perspective not a geographic location.”
Professor Sullivan said it was important to acknowledge why so many safeguards had been created in the first place.
“There’s no doubt that being more fluid with your data does expose you to greater risks of leaks,” she said.
“No-one’s ever died from a data leak. People do die from preventable illnesses all the time.”Changes ‘not rocket science’
In north-west Queensland, doctors from Cairns, Townsville, Brisbane and a local health service may all be treating patients in the same community depending on their specific health needs.
That can mean patient information is split between different hospital and health services which all have their own privacy requirements.

High chronic disease rates in north-west Queensland mean outside HHSs often deliver specialist care, complicating the flow of data. (Supplied: Kidney Health Australia)
After spending 12 years in metropolitan GP clinics, Dr Sekhon said the north-west’s fragmented medical system was the most confusing she had dealt with.
“There’s no centralised system. It was probably one of the most complex and convoluted systems that I have seen,” she said.
Dr Walker wanted to see an industry shift in how patient data and clinical correspondence is seen.
“Handovers occur all the time in hospitals. It goes between treating teams, it occurs when one shift goes off and another one starts,” he said.
“We just want to provide the best care for our patients. It’s not rocket science.”