You’re reading Part 1 of Paying for AI, a series examining how new clinical artificial intelligence tools influence the affordability of health care and patients’ long-term health.
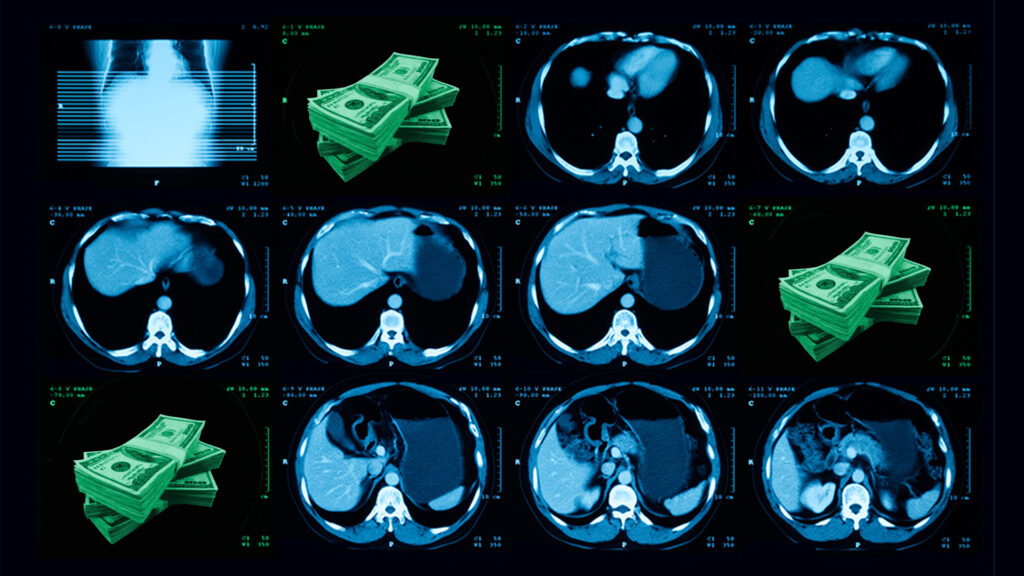
In a CT scan, coronary artery calcium shows up as distinct, bright pixels. It looks like salt in the pepper of the heart. The more calcium, the higher a patient’s risk of a heart attack.
Often, a cardiologist looks for those bright spots on purpose: They’ll grab snapshots of the heart between beats, to get the clearest possible view of the coronary arteries. But calcium is also visible on zoomed-out chest CTs that aren’t synchronized with the heart. Every year, patients receive 19 million of those more general scans — to screen for lung cancer, or investigate a persistent cough — and an eagle-eyed radiologist can report any incidental calcium they spot.
But even as heart disease remains the top cause of death in the United States, an estimated 20% to 40% of that incidental calcium goes unreported. “We need to find more of these patients,” said Ami Bhatt, chair of the Food and Drug Administration’s Digital Health Advisory Committee and chief innovation officer of the American College of Cardiology.
STAT+ Exclusive Story
Already have an account? Log in
This article is exclusive to STAT+ subscribers
Unlock this article — and get additional analysis of the technologies disrupting health care — by subscribing to STAT+.
Already have an account? Log in
Individual plans
Group plans
To read the rest of this story subscribe to STAT+.