For decades, insulin has been injected into the skin, a process that many diabetics find uncomfortable or even distressing. The introduction of a transdermal insulin delivery system represents a potential game-changer, allowing patients to manage their blood sugar levels without needles. The study, published in Nature, demonstrates how a polymer-based gel can carry insulin across the skin’s natural barrier and into the bloodstream, effectively normalizing blood sugar for hours.
The Challenge of Delivering Insulin Through the Skin
Human skin is designed to act as a protective barrier, preventing substances from entering the body. The outer layer, called the stratum corneum, is especially resistant to large, water-loving molecules like insulin. For years, scientists believed that insulin, being a large protein with a hydrophilic exterior, could not cross the skin without needles or specialized devices.
According to a new study from Zhejiang University in China, however, researchers have overcome this obstacle by designing a polymer that responds to the skin’s natural pH gradient. The polymer, known as OP (poly[2-(N-oxide-N,N-dimethylamino)ethyl methacrylate]), binds to the skin’s lipids at the acidic surface and gradually releases the insulin as it moves deeper into the skin’s neutral layers. This breakthrough may allow for more comfortable and non-invasive insulin delivery in the future.

Testing and Results in Animals
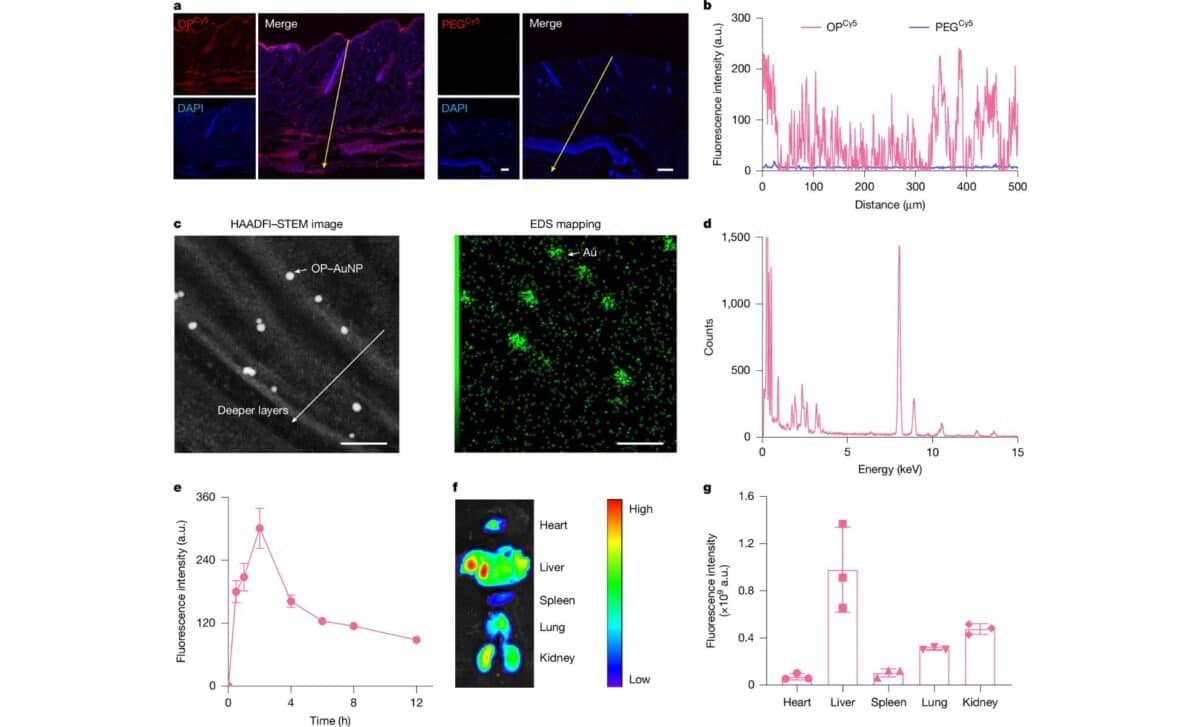
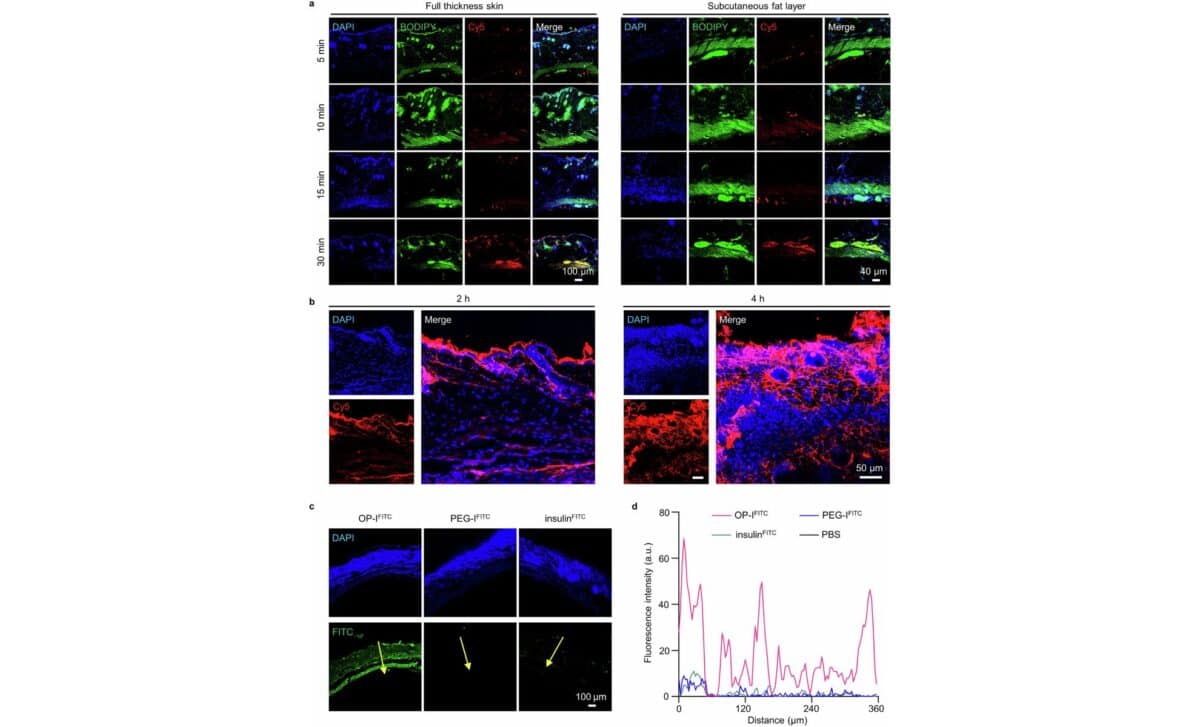
The researchers first tested the OP polymer on lab-grown human skin models and diabetic mice, where it showed promising results. Insulin paired with the OP polymer crossed the skin barrier much more effectively than insulin alone or when combined with other polymers like PEG. In mice with type 1 diabetes, a single topical application of OP-conjugated insulin lowered blood glucose levels to normal within an hour, with the effects lasting for about 12 hours.
The results were so encouraging that the researchers moved on to testing the OP-insulin gel on diabetic minipigs, whose skin and physiology are more similar to humans. According to the study, the minipigs’ blood sugar levels also dropped within two hours and remained stable for the same duration. This success in animal models represents a significant step toward eventual human trials.
A Future Without Needles?
While the research shows great promise, the OP-insulin gel is still in the experimental stage. It is far from ready to replace insulin injections entirely. However, if the gel proves effective in human trials, it could become an important part of diabetes management for many patients. The polymer could offer a slow, continuous release of insulin over several hours, potentially replacing or supplementing traditional insulin injections for people who need a basal dose throughout the day.
However, the gel may not be suitable for all forms of insulin therapy. Some people with diabetes require rapid insulin action at mealtimes, and a transdermal gel that works over 12 hours might not meet their needs. According to the study, the OP-based delivery system could be paired with other treatments, such as rapid-acting insulin injections, to create a more comprehensive management strategy.
This research is part of a broader effort to reduce the reliance on needles in diabetes care, a goal that has driven the development of microneedle patches and other alternatives. With millions of people worldwide living with diabetes, finding less invasive, more patient-friendly treatment options is crucial. If the OP-insulin gel is proven safe and effective for human use, it could significantly improve the lives of diabetics, providing them with a painless and convenient method of managing their condition.

