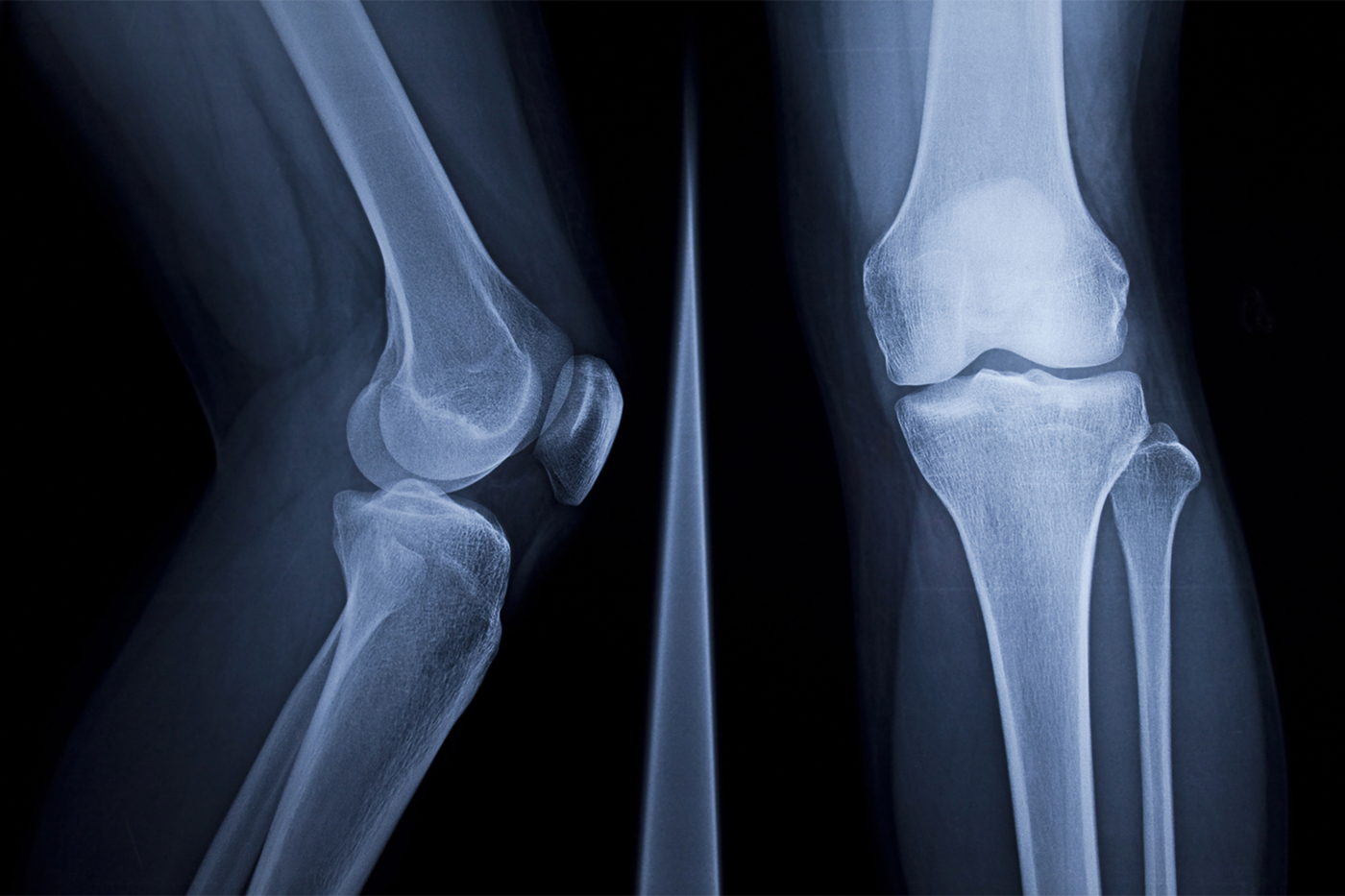
A doctor orders an X-ray for a patient with a knee ache. The bones look fine, and the most likely prognosis is arthritis, which occurs when the soft tissue between joints breaks down.
But X-rays are much better with hard tissues like bone, which absorb X-rays and turn white in an image, while soft tissue allows most of the X-rays to pass through. Without an appropriate contrast agent, which makes it easier to see soft tissues under X-rays, the best a doctor can do is look at the distance between the thigh and shin bones and make an estimate about the severity of the patient’s arthritis.
A professor at Northeastern University has come up with a solution that may help — turn the contrast agent into a magnet attracted to soft tissue.
In her lab, Ambika Bajpayee, an associate professor of bioengineering, focuses on basic property of the human body, which is that most of the soft tissues in our body are negatively charged.
“Everything is charged around us,” she continues, saying these charges are “the most fundamental thing in nature.”
 Ambika Bajpayee calls charged particles “the most fundamental thing in nature.” In her drug delivery research, she leverages this fact to create chemicals that will travel naturally to different parts of the body, drawn by tissues’ innate charges. Her latest patent is a contrast agent that is 100 times more efficient than those currently in use. Photo by Ruby Wallau/Northeastern University
Ambika Bajpayee calls charged particles “the most fundamental thing in nature.” In her drug delivery research, she leverages this fact to create chemicals that will travel naturally to different parts of the body, drawn by tissues’ innate charges. Her latest patent is a contrast agent that is 100 times more efficient than those currently in use. Photo by Ruby Wallau/Northeastern University
Many molecules in soft tissues — like proteins, cell membranes — carry net negative charges.
The negative charge in our soft tissues is important for both structure and function, she says. In cartilage, which is the soft tissue that acts as a cushion between the joints, the negative charge actually helps the cartilage spring back into its original shape after bearing a load, like in the knee after we take a step.
Northeastern Global News, in your inbox.
Sign up for NGN’s daily newsletter for news, discovery and analysis from around the world.
In fact, she continues, “more than 50% of the tissue’s stiffness comes because of this” effect.
Importantly, and like a magnet, negative particles repel other negative particles, while they are drawn toward positive particles.
It’s why Bajpayee and her collaborators chemically engineered a new, positively charged contrast, for which they recently received a new patent.
Because the contrast carries a net positive charge, negatively charged particles in cartilage attract and pull the contrast into the joint and hold it there more efficiently than the current method, Bajpayee says.
Currently, imaging a joint means injecting contrast — commonly an iodine-based chemical — so that X-rays can image the joint. But cartilage doesn’t get much blood flow, which means most of any contrast agent injected into the joint doesn’t stay there to be picked up by the X-ray machine, but instead leaks into the surrounding tissues.
This means that to obtain images of a small area, physicians must inject a relatively large amount of contrast to increase the chances that some of the liquid sticks around in the joint. That in turn poses other problems. The iodine often used in contrast agents can be harmful for people with pre-existing kidney problems.
Bajpayee’s method, thanks to how efficiently the contrast sticks to the joint, can be performed with 40 times less the usual amount of contrast.
Once injected, the joint absorbs the positively charged contrast in about two hours, after which the X-rays can be performed. She expects that the contrast would break down in the body after about 24 hours, though further tests are needed.
Their first tests were performed in mice, but Bajpayee thinks that, because this particular patent is for contrast agents and not drug delivery, experiments in human subjects are next. “I do believe that some of this will come into the market” soon, she says.
Noah Lloyd is the assistant editor for research at Northeastern Global News and NGN Research. Email him at n.lloyd@northeastern.edu. Follow him on X/Twitter at @noahghola.