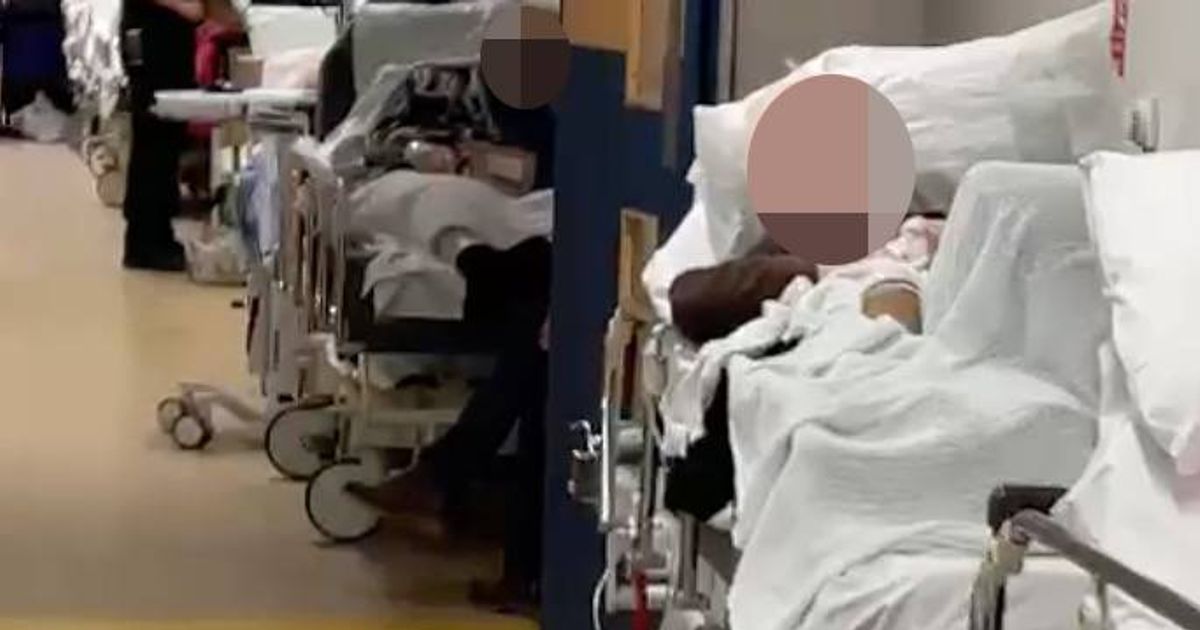
One man says he was left on a trolley with no blanket or pillows for 16 hours after a heart attack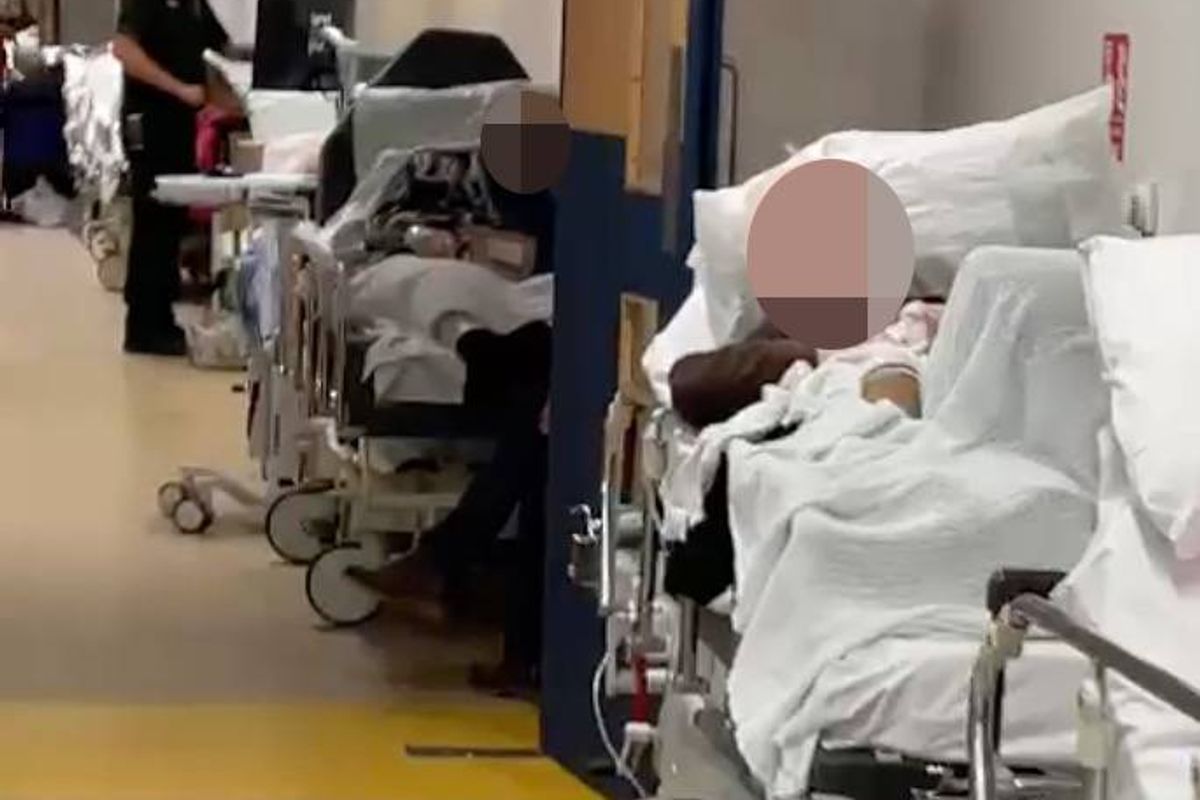
Patients in a corridor at an NHS hospital(Image: )
More than 100,000 pensioners were stuck for between one and three days in A&E corridors and waiting rooms before being moved to a bed on a hospital ward last year.
New analysis from Age UK has found more than half of these patients – 53,870 – were over the age of 80 with some forced to lie on the floor and told to wash in toilet sinks as they waited to be seen.
The charity said extremely unwell patients were being left for hours “day in, day out” at some NHS hospitals, with the situation becoming “routine”. It also shared doubts that the Government “really appreciates the seriousness of this situation and has the grip to turn it around”.
The figures obtained by Age UK under a Freedom of Information request related to unplanned attendances at major, consultant-led A&E departments where patients were admitted to hospital between April 2018 and March 2025. The analysis found that in 2024/25, some 101,972 people aged 65 or over waited for a bed for between one and three days after a decision to admit them to hospital had been made.
Caroline Abrahams, Age UK charity director, described the figures as “staggering”.
“Waiting for more than 24 hours, often on a hard chair in a corridor or other overspill area, when you are extremely unwell, in pain, probably alone, maybe fearing for your life, would be horrific at any age, let alone if you are in your eighties or beyond,” she said. “And yet this is happening day in, day out in the worst affected hospitals, to the extent that it’s become routine.”
One 77-year-old patient named David told Age UK he spent 30 hours waiting in A&E and “could barely move”. He was told there were no beds or trolleys, and ended up lying on the floor. “Someone gave me a coat to put under my head. I’d been awake for three nights by then. It was horrendous.”
Another man, Michael, 80, was left on a trolley for 16 hours after having a heart attack with no blankets or pillow while Jennifer, 76, waited 36 hours with no washing facilities. She was told to wash herself in a toilet sink with no plug. “I felt like something that had been left on the streets,” she said. Ms Abrahams added: “We should all be ashamed that this is what we’ve come to in some hospitals, it’s utterly soul destroying for doctors and nurses, and extremely frightening for older people who know they may need to go to A&E one day.
“Of course, no-one is happy with conditions like these, including ministers, but at Age UK we are yet to be convinced that the Government really appreciates the seriousness of this situation and has the grip to turn it around.”
Ms Abrahams said the situation “can be turned around, as some hospitals have shown”. “There is much that they can do themselves to reduce their long waits and corridor care, learning from the example of the best, but they can’t do it all on their own and there’s a pressing need for Government to show leadership and publish a comprehensive, costed plan,” she added.
The Age UK analysis comes after a probe by the Health Services Safety Investigations Body found some NHS hospitals are adapting corridors and other spaces to provide care by installing plug sockets and emergency call bells in a bid to minimise patient safety risks.
Senior staff told the watchdog the changes were made as medics “could not avoid using these spaces”.
A report published last week by the Royal College of Nursing also warned that collapsing care standards in the NHS are pushing staff morale almost “past the point of no return”. Age UK is calling for the Government to create a funded plan with specific deadlines to slash long A&E waits and end corridor care, as well as establishing a system to collect regular data on corridor care.
It also said a minister should be appointed to be accountable for tackling these issues, with a requirement to report to Parliament every six months. Ms Abrahams said: “It certainly isn’t possible to eradicate corridor care and long waits with the stroke of a pen, it will take time and commitment, but the sooner the Government makes a start the quicker we’ll restore a sense of decency in and around our A&Es, which is the least that our older population and hard-pressed hospital staff deserve.”
The latest monthly performance figures published by NHS England show the number of people waiting more than 12 hours in A&E departments from a decision to admit to actually being admitted stood at 50,775 in December, up slightly from 50,648 in November.
The number waiting at least four hours from the decision to admit to admission also rose to 137,763, up from 133,799. Some 73.8% of patients were seen within four hours in A&Es last month, down from 74.2% in November.
The Government and NHS England have set a target of March 2026 for 78% of patients attending A&E to be admitted, discharged or transferred within four hours.
Get daily headlines and breaking news emailed to you – it’s FREE