For the first few years after Victoria Stephens had the contraceptive implant Nexplanon placed just under the skin in her left arm, it was ‘perfect’, she says.
‘I had no periods, no pain and I didn’t have to remember to take the Pill every day,’ says Victoria, 28, a married retail assistant from Gosport in Hampshire.
The plastic, rod-shaped device, roughly the size of a matchstick, is used by around 400,000 women in the UK as a form of birth control.
Once in place, it releases the hormone progestogen, which inhibits ovulation and thins the lining of the womb – making it hard for a fertilised egg to embed.
The implant has soared in popularity over the last decade, largely thanks to the convenience factor; it only needs replacing every three years and, in most cases, can easily be removed if a woman decides to start a family.
The implant has soared in popularity over the last decade, largely thanks to the convenience factor; it only needs replacing every three years and, in most cases, can easily be removed if a woman decides to start a family.
What’s more, it’s just as effective as oral contraception.
Victoria was happy to move on to her third successive implant in 2020 – but before her appointment she noticed a problem with the existing one.

Like 400,000 women in the UK, Victoria Stephens used birth control in the form of a contraceptive implant, which had been placed just under the skin in her left arm
The contraceptive implant is a rod-shaped device, roughly the size of a matchstick. Once in place it releases the hormone progestogen, which inhibits ovulation and thins the lining of the womb – making it hard for a fertilised egg to embed
‘I had always been able to make out a little bump where it sits just beneath the skin,’ she says. Suddenly, however, she realised there was no sign of it.
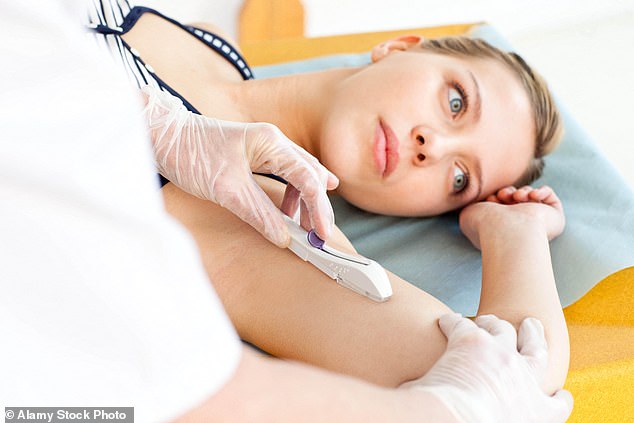
Victoria rang her GP and was told to come in as soon as possible. A nurse examined her and said the implant had become lodged deep in her upper arm.
‘She looked concerned and said it was going to be difficult to remove,’ says Victoria. She was ushered into another room, where a GP injected local anaesthetic and made a 2cm-long incision to try and reach the device. A very ‘scared’ Victoria endured ‘the doctor tugging away at my arm trying to retrieve it’.
The GP managed to get it out – but Victoria needed ‘four external and two internal stitches and had to wear my arm in a sling for several days while it healed’.
A report in 2020 by the Medicines and Healthcare products Regulatory Agency (MHRA) – which vets the safety of drugs and medical devices, such as implants – revealed that at least 126 women in the UK had been affected by wandering Nexplanon implants since the device was approved for use in 2010.
Eighteen of these women needed emergency treatment for devices that had become stuck in or around their lungs, causing severe breathing problems.
More recently, in December 2025, surgeons at Royal Papworth Hospital in Cambridge described in the journal BMJ Case Reports how they had to operate on a woman in her 20s, cutting a hole in her chest wall, after her Nexplanon implant travelled from her arm to her pulmonary artery – which connects the lungs to the heart. She needed five days in hospital recuperating.
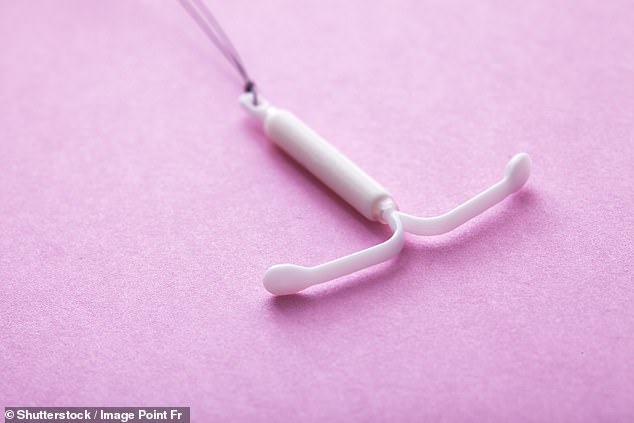
Studies show another contraceptive – the IUD (a device placed inside the womb) can move around the body, with potentially devastating consequences
The Nexplanon is implanted using a ‘gun’ that fires it into the arm. Dr Kathryn Clement, a consultant gynaecologist at the Royal Victoria Hospital in Newcastle upon Tyne, says it’s ‘very rare’ for it to become stuck in blood vessels in the lungs, for example.
But if implants have migrated, ‘it’s not always possible to remove them if they have been there for a prolonged period of time, as scar tissue can develop’.
What can make it worse for the women affected is the fact that the implants keep working as long as they are intact, meaning they are highly unlikely to be able to conceive until all the progestogen has been released.
‘For the unfortunate women who have implants in their lungs that cannot be removed, this means they will have effective contraception for several years ahead – that might not be what they intended if they were planning a family,’ says Dr Clement.
She says problems with the Nexplanon implant usually arise when it is mistakenly inserted into the basilic vein – a blood vessel which runs up the length of the arm – rather than between the skin and other tissues.
This means it can get swept along in the bloodstream, potentially navigating its way down to bigger blood vessels around the heart and lungs.
In December 2024, Danielle Jarrett, from Dartford in Kent, hit the headlines when she described how she had lost the use of her left arm because her Nexplanon implant, which was inserted in 2019, had got stuck so deep in the surrounding tissue that it caused nerve damage.
Doctors at St Thomas’ Hospital in London tried to remove it for two hours, before telling Danielle that they couldn’t and would have to leave it where it was.
She said at the time: ‘I can’t use a knife and fork. I have to get someone else to cut up my food.’

Danielle Jarrett lost the use of her left arm after her Nexplanon implant got stuck so deep in the surrounding tissue that it caused nerve damage
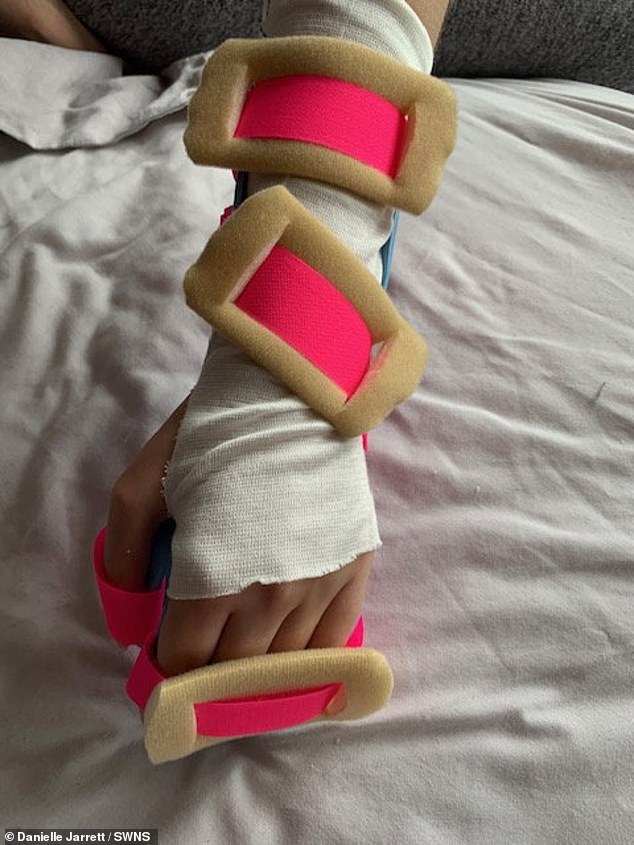
Doctors tried to remove Danielle’s implant for two hours, before telling her that they couldn’t and would have to leave it where it was. She said at the time: ‘I can’t use a knife and fork. I have to get someone else to cut up my food’
In another case, a woman from Essex was shocked to discover she was 22 weeks pregnant, months after raising concerns that she could not feel a replacement implant she’d had inserted in 2018. Doctors had assured her it had just been put in slightly deeper than previous ones.
The woman gave birth to a baby boy, but Nick Leahy, a solicitor who represented the woman through law firm Osbornes, told Good Health: ‘Neither she nor her husband wanted children – so this had a massive impact on her psychologically and she even needed psychiatric counselling.’
Nexplanon is not the only implant reported to ‘migrate’.
Studies show another contraceptive – the IUD, or ‘coil’ (a device placed inside the womb) – as well as implantable loop recorders (tiny devices placed under the skin to monitor heart rhythms in patients with dizziness or fainting) and dental implants can also move around the body, with potentially devastating consequences.
A main issue is human error. The five-minute procedure to place the Nexplanon involves a local anaesthetic being used to numb the area before a gun-like device punctures a tiny hole in the skin.
The implants should be placed just under the skin in the non-dominant upper arm, over the triceps muscle, says Dr Clement, adding highly trained staff doing hundreds a year can still make occasional mistakes.
The doctor or nurse inserting the implant should have completed training run by the College of Sexual and Reproductive Healthcare (patients can check by asking staff).
Incorrect insertion is much more common when the fitter has not been appropriately trained, when the woman is very slim or has very little fat, says Dr Clements.
According to the MHRA: ‘Women should be shown how to locate the implant immediately after insertion and advised to check it occasionally to ensure it has not migrated.’
In the case of the woman in Essex who became pregnant after having the procedure, subsequent investigations revealed there was no trace of the implant, or the progestogen it should be releasing, anywhere in her body.

In 2024, TV personality Dani Dyer revealed she needed surgery to remove her contraceptive implant after it migrated. Scans showed it was in her pelvic area
The conclusion was that it was never inserted in the first place and had possibly fallen out of the device before it was used.
She pursued a claim of wrongful birth against Central London Community Healthcare NHS Trust, which ran the implant service, and received an out-of-court settlement for £35,000.
In the case of IUDs, migration occurs in around one or two cases per thousand patients, according to the NHS – roughly 700,000 women in the UK are thought to have an IUD implant.
In 2024, TV personality Dani Dyer revealed she needed surgery to remove her contraceptive implant after it had moved. The mother-of-three, 29, developed agonising stomach cramps and heavy periods after being fitted with a Mirena coil – which can provide birth control for up to eight years.
Scans showed it had migrated into her pelvic area and prompt surgery was needed to remove it.
In the most severe cases, an IUD that has moved can lead to appendicitis, bowel obstruction and life-threatening sepsis. The NHS advises women to check every three to four months that they can locate the two threads attached to the bottom of the IUD.
Implantable loop recorders – tiny devices that sit beneath the skin in the chest, attached by leads to nearby muscle, to monitor heart rhythms for up to four years – can also migrate.
These are used to pinpoint what’s causing repeated dizziness or fainting, as well as to diagnose atrial fibrillation (an irregular heartbeat).
But in some cases – under 1 per cent – the devices (which are about the size of a USB stick) move, ending up in the chest or lungs, which can be lethal.
Meanwhile, studies show that in about 5 per cent of pacemaker instalments (which are used to regulate heartbeat), the leads themselves become displaced, often puncturing a lung or damaging the heart.
As Good Health has previously reported, thousands of women have been damaged by surgical mesh – used to treat stress urinary incontinence – breaking up and lodging into muscles and nerves.
Even tooth implants can dislodge. A 2021 paper in the journal Scientific Reports, described 11 cases where patients had artificial teeth fixed into their upper jaw – only for them to disappear over the following months.
Later X-rays showed that the teeth, propelled by chewing, had lodged in patients’ sinuses. All 11 had the implants surgically removed.
For Victoria, the extraction of her Nexplanon implant should have been the end of the matter. But in January 2023 she decided to have a fourth implant – this time inserted in her other arm.
To her horror, last October Victoria realised she could no longer see or feel the implant and the area where it had been situated was painful.
She says: ‘I have also been getting strange sensations. If I’m cold, the area around it feels ice-cold. If I’m warm, it feels like a burning pain inside my arm.’ Worse still, her periods have restarted, suggesting the implant has stopped working. She is now waiting for a GP appointment to have it removed.
‘And I’ve decided I will not have the contraceptive implant again. This isn’t worth the risk,’ she says.
Organon, the pharmaceutical company which makes Nexplanon, declined to comment when approached by Good Health.
Case study interview: JULIE COOK
