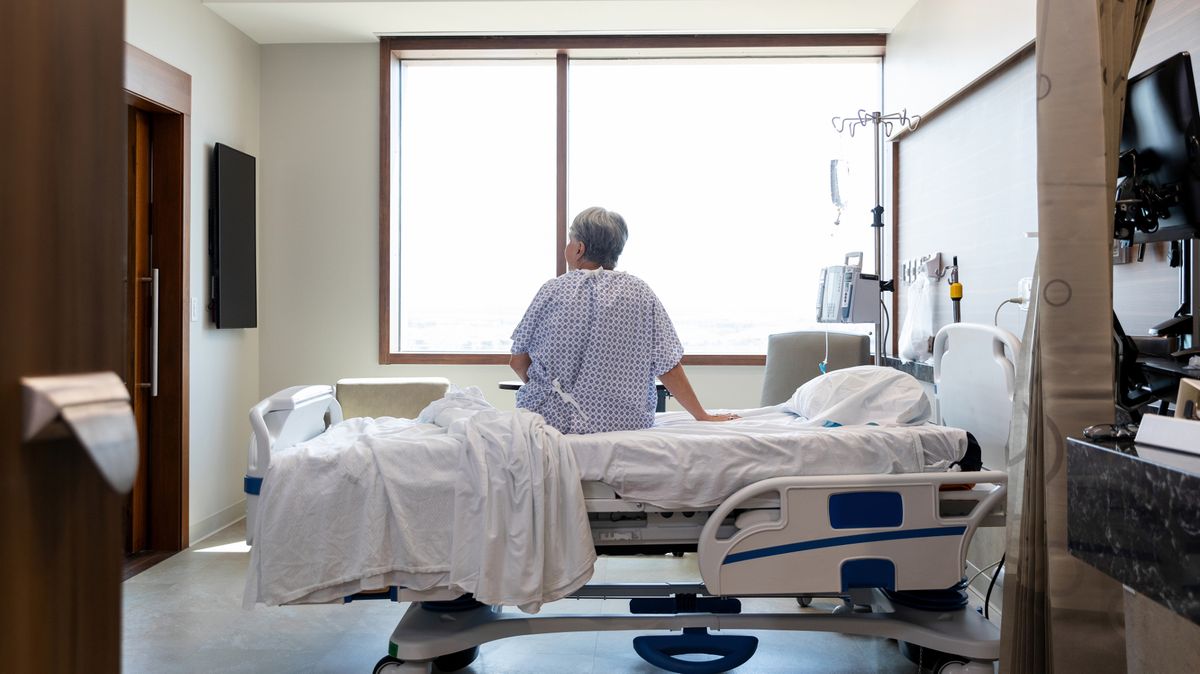
Landmark review of NHS dementia care reveals ‘culture of containment’ where patients are drugged and prevented from leaving their bed – sometimes for weeks
21:00, 15 Mar 2026Updated 23:07, 15 Mar 2026
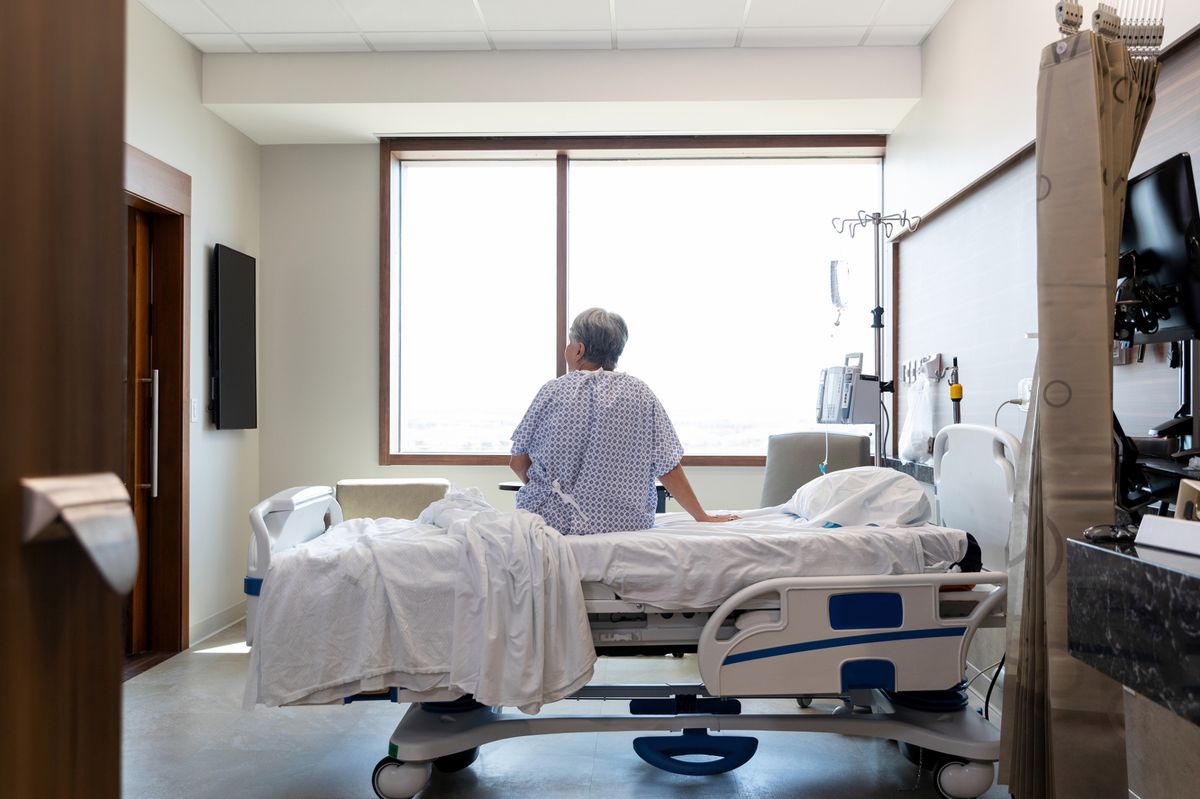
Dementia patients are subject to a ‘culture of containment’ in the NHS(Image: Getty Images)
Dementia patients are routinely sedated and forcibly prevented from getting out of bed according to the first ever national review of their NHS care.
A landmark report following 18-months of observations at six hospital trusts identifies a “culture of containment” on wards where dementia patients are prevented from leaving their bed, sometimes for weeks. Restrictive practices start with raised bedside bars that prevent dementia patients getting out of bed. If they try to get out of bed they can be physically restrained and be given sedatives or antipsychotic drugs.
The report’s authors say confused patients reported feeling like they were in “prison”, “kidnapped” and “held hostage”. If they try to forcibly leave the bed or push a member of staff they can be labelled “aggressive in their medical notes. This can lead to social care packages being withdrawn, meaning they can never go back to living independently at their home or return to their care home.
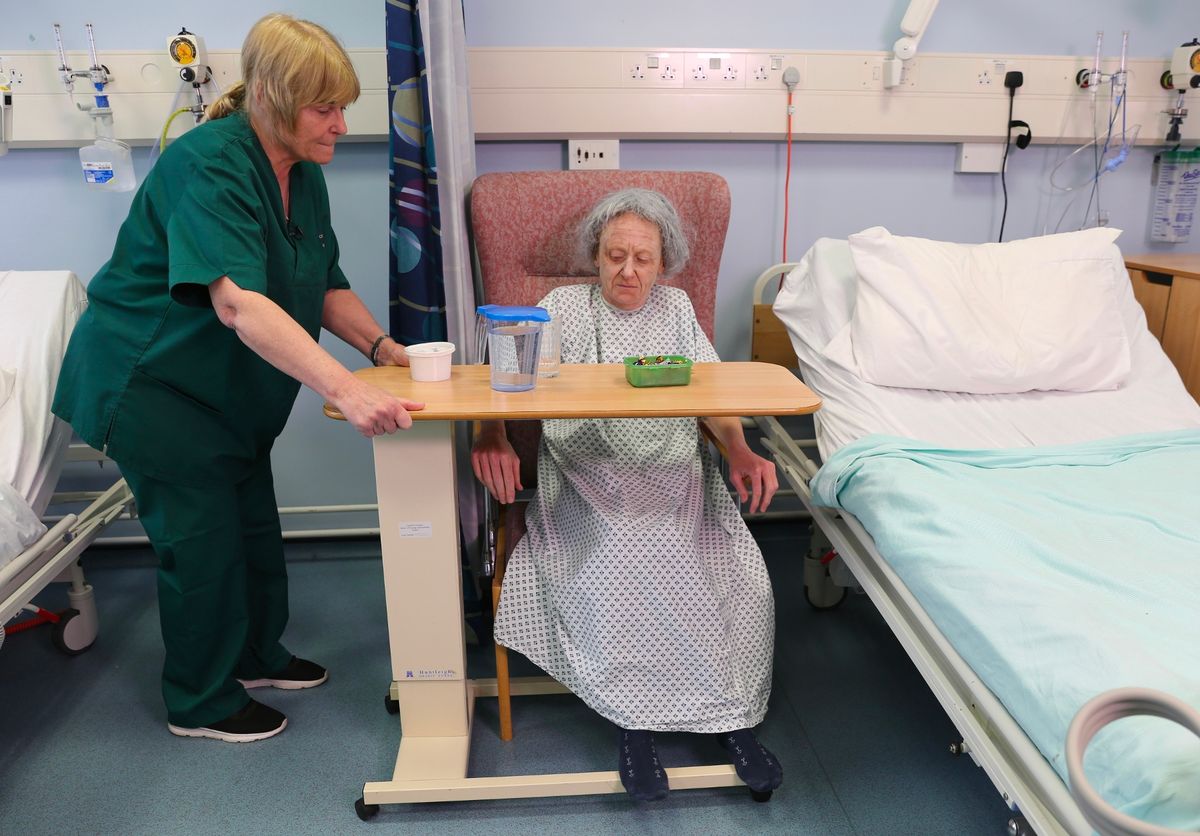
Attached table tops are used to keep frail dementia patients in a chair(Image: nick@nickdaw.com)
READ MORE: ‘NHS hospital secretly sedated me and wouldn’t let me leave my bed for a week’READ MORE: Dementia 63% surge – smart homes and how we could live independently for longer
Lead author Professor Andy Northcott, of the University of West London, said: “They wake up and realise they don’t know where they are, they are in a bed that is essentially a cage and they can’t get out. What is happening every day to dementia patients doesn’t fit with what the NHS should be doing.
“These are people. We think about dementia being a kind of end-of-life stage but these are often people living pretty independently at home with their partner who come in with a fairly mundane illness like a urinary tract infection. If they had not got that they would have lived at home with their families for years.”
A million Brits have dementia with cases expected to surge in the next decade as the UK population ages. The report, funded by the National Institute for Health and Care Research (NIHR), will be launched on Thursday and has major implications for how the NHS cares for people living with the condition in the years to come. It looked at how dementia patients are cared for during an urgent or unplanned hospital admission such as after a fall or when suffering a sudden illness or injury. Such admissions of dementia patients make up between 25% and 50% of all acute hospital admissions.
The review exposes “taken-for-granted practices that have over time become part of the everyday ward cultures”. Containment typically involves blocking patients in their beds with furniture and repeated verbal commands to “sit down” or “go back to bed”. Often they are unable to go to the toilet and patients could be told to go in a bottle.
Minor ward misunderstandings can escalate rapidly, with a patient quickly becoming labelled as “aggressive” or “challenging” – leading to them being physically restrained and sedated. Such patients end up filling hospital wards as they become bed blockers because there is nowhere safe to discharge them to.
Prof Northcott, a professor of medical sociology at the university’s Geller Institute of Ageing and Memory, said: “If a patient starts pushing a security guard or member of staff they can get labelled as aggressive and it means they can’t go home. They may lose their home visits care package or the care home will say they can’t accept them. Once it’s in the NHS notes it has become medicalised and because of these practices they never go home.”
The 18 month study observed nine acute wards across six NHS hospital trusts chosen to be representative of the country as a whole. Some 168 patients and medics agreed to participate in over 1,000 detailed interviews.
Restraint used to restrict the movement of dementia patients typically starts with raised bedside bars that prevent them getting out of bed. Another measure sees patients in a bedside chair with a table attached at the front which has the effect of trapping them in.
The report says restraint can then escalate so that spaces next to the bed and doors are blocked with furniture. This comes alongside verbal commands telling patients to “sit down” or “go back to bed”.
One-to-one supervision was the next step with a nurse or security guard sat in a chair next to the bed. If a patient then tried to get out of the bed they were physically restrained and could be injected with antipsychotic drugs. Patients also had sedatives added to their daily medication.
Professor Andy Northcott explained: “People with dementia can typically be in hospital for as long as two weeks. Over time they tend to start to push against being kept in bed all day, every day. That one-to-one nurse sitting next to their bed is replaced by a security guard. You have an old person wondering why they are not allowed to stand up and why there is a big man dressed all in black in front of them. You get patients talking about being in ‘prison’ or being ‘kidnapped’.”
The report, seen by the Mirror, found restrictive practices go unrecognised and unrecorded as restraint. Almost every dementia patient observed experienced some form of restraint. The endemic practices are justified to minimise risk of falls, absconding or violence. Researchers insist staff have patients’ best interests at heart but worry about “reprisals” professionally or from families if they leave the bedside and come to harm.
Prof Northcott said: “It’s not the old fashioned asylums of people being strapped down, but you might have a security guard hold someone down in a chair. You get patients lifted up by their arms and walked back to their bed. That does happen quite frequently.
“The nurses and care staff are trapped in a horrible situation because there will be instances of violence against them. There will have been cases where patients leave, get lost and come to harm. Staff feel they are acting in the patient’s interests. They are also terrified of the risk that if something happens it will be on them.”
The report says NHS dementia care amounts to depriving patients of their liberty – interfering with their rights under Article 8 of the European Convention on Human Rights. Its authors said being confined to a bed for long periods can cause dementia to progress while patients deprived of toilet breaks can become incontinent.
The review recommends that any restrictive measures for dementia patients be recorded and justified by the NHS. It says staff should be supported in recognising that distress in patients is linked to their confinement and the often chaotic and frightening ward setting rather than an inevitable feature of their dementia. Staff guidance should allow them to support patients to leave their bedside without fear of liability.
Coping with dementia is a generational challenge for developed nations and the Alzheimer’s Europe report in January estimated that patient numbers will double in Britain by 2050. It forecasts there will be two million people living with dementia – meaning one in every 26 Brits over 30 will have the degenerative brain disease.
Prof Northcott added: “For the first time we are actually making progress with dementia. We are starting to diagnose earlier and slow its progression. We are going to have more and more people diagnosed who come to hospital and we need to prepare for that. Because once that diagnosis is there it is a very powerful label that these people have. Dementia patients are already the bulk of people in hospitals and that’s only going to get bigger.”
A spokesman for NHS England said: “People living with dementia should always be treated with dignity in every care setting – restrictive practices should only be used as a last resort and if absolutely necessary for patients’ safety. The NHS has provided staff with guidance and training resources to on how to keep patients safe with the least restrictive practices.”