“Sláinte” will be on the lips of many millions of people around the world today as all things Irish are toasted to celebrate St Patrick’s Day.
The one-word utterance of “health”, is of course shorthand for the wish of good health (sláinte mhaith) to glass-chinking companions. The likelihood of enjoying good health in Ireland is above average, when compared with other developed countries.
Considering the State’s prosperity, high levels of education and relatively clean air, that is hardly a surprise. But a ranking of its healthcare at number six in the world might be.
In the space of just four years, Ireland has shot up 74 places in one of the leading international benchmarks for healthcare. The index is compiled for global investors, using data on how nations are investing in healthcare infrastructure, medical talent, and government readiness.
“Healthcare is no longer a domestic issue. It is a strategic asset that shapes global competitiveness, labour markets and capital flows,” CEOWorld magazine, which publishes the index, states. Back in 2021, Ireland was languishing in 80th place out of the 110 countries monitored. The 2025 table, which is topped by Taiwan, followed by South Korea and Australia, elevates us to sixth position.
“Living in Ireland, we definitely have a reasonable health system, but I don’t think anybody would say, ‘Gosh, this feels like the sixth-best health system in the world’,” says Martin Curley, professor of innovation at Maynooth University and former director of digital transformation at the HSE. This “extraordinary leap” in the index is primarily due to unprecedented investment in healthcare here over recent years but this is also masking some underlying problems.
Healthcare is not a linear system. Multiple, compounding changes and innovations have led to this jump, Curley explains. There is always a lag between policy decisions and investments, and seeing the fruits. He considers the addition of 51 primary-care centres since 2020 as one of the huge improvements.
“I think they are the jewel in what I call the shift-left strategy – moving care out of hospitals into the community.”
The chronic disease prevention and management programme has also been “very significant”. Overall, substantially increased investment in health resources has clearly lifted us up the ranking.
 Martin Curley, professor of innovation at Maynooth University and former director of digital transformation at the HSE
Martin Curley, professor of innovation at Maynooth University and former director of digital transformation at the HSE
Over the past 10 years, the State’s annual health budget has nearly doubled, from €14 billion in 2016 to €27.4 billion for this year, with more than 50,000 healthcare workers added to the public service over the decade up to 2024.
However, return on that scale of investment has been very low, says Curley, referring to a 2024 Department of Health report that looked at productivity in acute care between 2016 and 2022. In 2022, for every €100 spent on healthcare, €96 was for day-to-day costs and €4 on capital expenditure, according to the Central Statistics Office.
“For all of this spending and all of these resources, the output only went up 3.8 per cent,” he says. “So the [ranking] improvement has been driven by the investment, but that’s masking a lack of productivity improvement and a lack of development.”
Other contributing factors to positive assessments in international comparisons include increased life expectancy here. Those born in the State today can anticipate being alive for 82.9 years on average, according to Health at a Glance comparisons among 38 OECD countries published last November. That is 1.8 years longer than the OECD average. The Swiss can expect to live the longest, for 84.3 years on average, while those in Mexico and Latvia have the shortest likely lifespan of just under 76 years.
But as longevity increases, there is more focus on adding life to the years and not just years to the life. The World Health Organisation brings a more nuanced look at countries’ health outcomes with its Healthy Life Expectancy (known as Hale) rating. This is the average number of years that a person can expect to live in full health, free from disease and disability.
The Republic comes at number 17 out of 184 countries, with a Hale estimation of 70 years. Singapore (73.6 years) tops the list, while Lesotho is bottom, at just 44.6 years. Northern Ireland is listed as part of the UK rating, at 68.6 years. The US is ranked 71st, with an expected 63.9 years of full health.
Life expectancy is one of 10 key indicators measuring health status and risk factors in the OECD report. The Republic performs above average on eight of those, including preventable deaths ie premature deaths among people aged under 75 that could have been avoided through better prevention and healthcare interventions. The State’s estimated 109 preventable deaths per 100,000 population compares favourably with an OECD average of 145, and 156 in the UK.
The rate of death by suicide is also below average in the State, at nine per 100,000 population compared to the OECD average of 11 and a high of 23 per 100,000 people in South Korea. However, a Unicef report, Child Wellbeing at Risk in an Unpredictable World, published last year shows the Republic’s youth suicide rate is above the international average.
While Irish teenagers lead the world in academic skills, taking top spot in Unicef’s league table, their physical health is ranked at 11th, out of 41 countries, and their mental health is down in 24th place. Nearly one in three 15-year-olds here report low life satisfaction.
Describing these findings as “stark”, Peter Power, director of Unicef Ireland, said at the time of their release last May: “Ireland’s teens are succeeding in school, but struggling in life.”
Our reputation as an island of drinkers persists but alcohol consumption has declined over the past decade. However, our consumption of 9.4 litres (of pure alcohol) per person aged 15-plus years is still above the OECD average of 8.5 litres. Most worrying, Ireland, along with Greece and Sweden, is highest for binge drinking, with more than 40 per cent of individuals indulging at least monthly.
In access to healthcare and quality of care, Ireland performs better than the OECD average on seven out of 10 indicators. This includes a screening rate of 69 per cent of women for breast cancer, well above the 55 per cent average, and 65 per cent satisfaction with the availability of quality healthcare, marginally above the 64 per cent average.
 In access to healthcare and quality of care, Ireland performs better than the OECD average
In access to healthcare and quality of care, Ireland performs better than the OECD average
Where Ireland falls down is in avoidable hospital admissions, at 545 per 100,000 population, above the OECD average of 473; a considerably higher use of antibiotics and marginally lower vaccination rate for children against diphtheria, tetanus and pertussis.
But in this OECD comparison of health systems, Ireland has more resources than average on just three out of 10 indicators. Those three are health expenditure, and numbers of nurses and pharmacists – all calculated per head of population.
Noticeable shortfalls are 2.9 hospital beds (versus 4.2 average) per 1,000 population; 38 CT scanners, MRI units and PET scanners (average 51) per million population and 44 per cent share (average 56 per cent) of generics in the pharmaceutical market. Also, the number of long-term care workers per 100 people aged 65 years and over in Ireland is 3.5, lower than the OECD average of 5.0.
Our unusual, public-private system is “a complete outlier in Europe”, says Curley, with nearly half the population buying health insurance. “But that combination between the public health system and the private means we have proportionately more investment and the quality of care and the access is better.”
The OECD report notes that “duplicate” private health insurance is most widely used in Ireland and Australia. Some 47 per cent of the population here buy it to get faster access and a wider choice of providers of core services that are free under the public system.
The highly regarded CEOWorld rankings do not share their scoring methodology, says Curley, but what they look at includes survey data, publicly available health system metrics, experts’ assessments, medical infrastructure and professionals, and medicine availability.
[ Ireland’s drugs budget rising every year in ‘unsustainable’ trajectoryOpens in new window ]
“An area where we score highly, in my opinion, is the calibre of our medical professionals, their training. We’re in the top two or three for the highest nurse-to-patient ratio. We’re slightly lower on doctors, but we’re actually quite healthy there.
“Overall, this is really positive. It means care has definitely improved, but it’s masking the fact that we are such a digital laggard,” says Curley, who resigned as director of digital transformation in the HSE in 2023, due to his frustration with institutional inertia.
He had set up a national Master’s in Digital Health Transformation in 2019. About 250 senior clinicians have been trained on the programme since, each having to deliver a digital change project “instead of writing a dissertation that lies on a shelf”. That, he says, “became a stealth mechanism for introducing digital change in a system that was actually quite resistant”.
In conversation with HSE chairman Ciarán Devane, Curley says they had agreed a primary success metric for the programme would be to lift Ireland from 80 to the top 10 in the CEOWorld rankings within 10 years. It’s “astonishing” that has happened in five years, he adds, although he is not suggesting the master’s programme can claim a huge amount of credit. However, he believes that, as a catalyst for change, it has been one contribution to the improved standing.
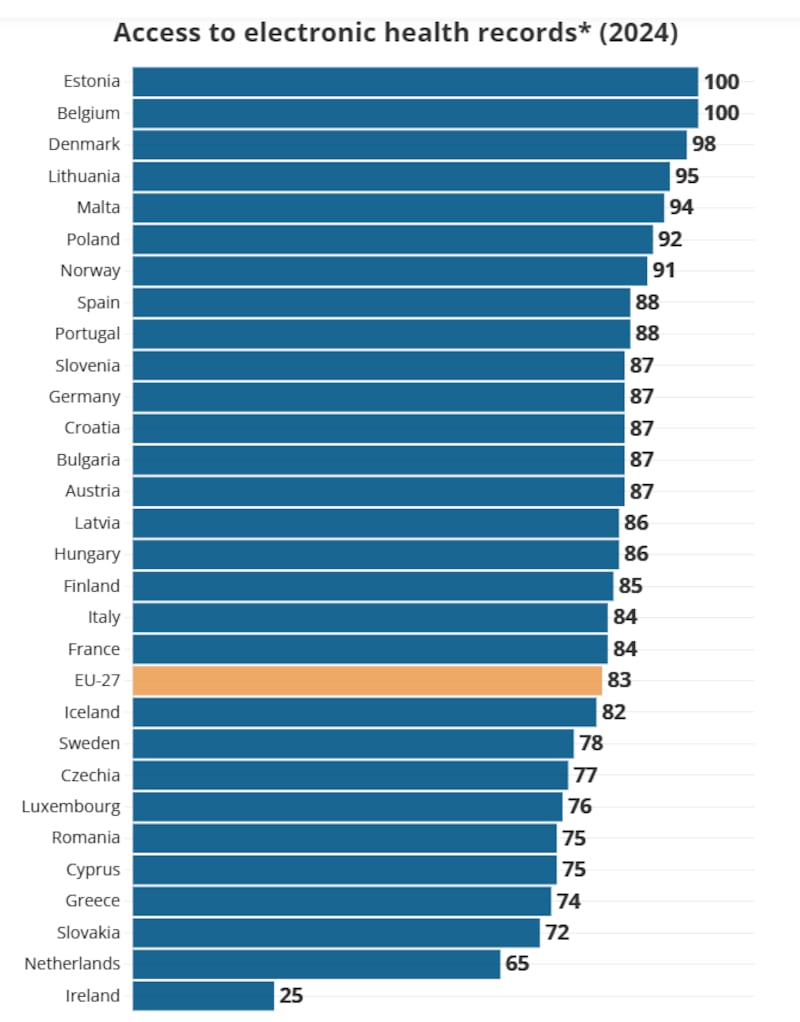 From the EU Commission’s Digital Decade 2025: eHealth Indicator Study. *The composite eHealth score (percentage). ‘Different systems that don’t talk to each other’
From the EU Commission’s Digital Decade 2025: eHealth Indicator Study. *The composite eHealth score (percentage). ‘Different systems that don’t talk to each other’
The Republic is very clearly bottom of the class in Europe when it comes to electronic health records.
An EU Commission study gives the State an eHealth maturity score of 25 per cent for 2024, while the EU-27 average is 83 per cent. Ireland is one of only two countries classed in the report as “beginners” on access to electronic health records. The other is the Netherlands, but its eHealth score is a considerably more respectable 65 per cent. Belgium and Estonia top the table, both on full marks.
However, the State’s 2024 rating was a vast improvement on just 11 per cent the previous year and further improvements are expected when the EU’s Digital Decade eHealth indicators for 2025 are published later this year. The HSE Health app, for instance, was launched in February 2025. But there is still a lot of catching up with the rest of Europe to do.
“We are, I suppose, a laggard in terms of digital systems,” says Rachel Flynn, director of health information and standards at Hiqa, the State’s health information and quality authority. The problem is that while various entities within public and private elements of the health system have their own digital services, “they’re not all joined up”.
For example, St James’s Hospital in Dublin has an electronic health record for its treatment of patients. “But once you go outside of St James’s Hospital, that’s where the difficulty arises. It’s not joined up with the community system because we don’t have a community system, etc.”
Patients may receive care from private hospitals as well as the HSE. They visit their GP, who may keep electronic records, and they might also be seen by a public-health nurse, who is under HSE governance and still using paper. “They’re all different systems capturing information that don’t talk to each other. And that’s where the problem lies for Ireland,” she says. Anybody wanting to access their health record has to ask each provider separately for their information.
“Most other countries would have a centralised system in place that allows patients to access that data. That is what we’re trying to achieve in Ireland, to be fair,” says Flynn.
 Rachel Flynn, Hiqa director of health information and standards. Photograph: Julien Behal
Rachel Flynn, Hiqa director of health information and standards. Photograph: Julien Behal
However, there is little optimism that we will meet a European Union target of 100 per cent of EU citizens having access to their electronic health records by 2030. Just last month the HSE received Government approval to begin vendor shortlisting for a national electronic health record (EHR).
“We have pockets of very good systems in place, but the problem is that we need this national EHR to bring it all together,” she says.
An EHR would ensure clinicians across all parts of the health service have timely access to accurate information, thereby improving safety and reducing duplication. It is also seen as a way of empowering patients to manage their care more effectively. The EU also aims to create a standardised health data space that would allow individuals to control and use their records at home or in another member country.
Legislative as well as infrastructural change is needed to advance digital progress here, to enable the HSE to request data from voluntary and private entities for an EHR. The Health Information Bill 2024 was before the Seanad earlier this month .
[ Ireland ranks worst for digital health policies in developed world, says reportOpens in new window ]
Hiqa has devised national standards and guidance around what information should be included in a national health record and what information should be accessible to different disciplines. There also has to be compatibility with other countries, “so that we can share that information with Europe eventually, when we have our infrastructure in place”, says Flynn.
There have been public consultations, which found that the vast majority of people are comfortable with their health information being stored and shared electronically. They see the benefits of moving towards a more integrated digital healthcare system, once safeguards are in place to protect their privacy.
Data quality might not be a hot topic, she says, but without really good data-collection protocols, it would be difficult to share information nationally and across Europe.
“You could have absolutely fantastic digital systems but, if you don’t have a regime around data quality, then people won’t rely on those digital systems to make clinical judgments,” adds Flynn. “And you’re back to square one, where they’re recording locally again.”
Another ambition under the European Health Database Regulation is for Ireland to set up a health data access body, which would allow researchers, policymakers and service planners to draw on anonymised data from a centralised source.

