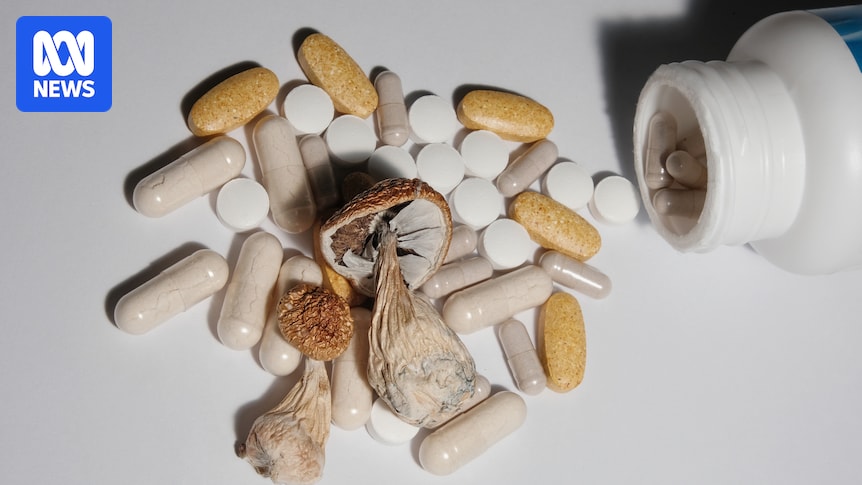
Prescriptions for psychedelic drugs and cannabis are on the rise in Australia, particularly for treatment of mental health disorders like depression.
But experts are urging caution, after three new studies have found scant evidence they can help to treat these conditions.
Two studies published in JAMA Psychiatry today investigated the effectiveness of psychedelics compared to traditional antidepressants.
The first study, which reviewed clinical trials that looked at LSD, psilocybin, peyote and ayahuasca, concluded these performed no better than traditional antidepressants for treating depression.

The trial found inconclusive long-term effects from testing psilocybin for depression, and some small risks from taking the drug. (ABC South West: Roxanne Taylor)
Results from the second study, which trialled psilocybin, the active ingredient in magic mushrooms, was inconclusive.
The studies come after another study published in The Lancet this week found there was no evidence from 54 clinical trials that cannabis and cannabinoids were effective treatments for depression, anxiety, or PTSD.
Jack Wilson, lead author of the cannabis study and a research fellow at the University of Sydney, said that the lack of evidence did not mean the treatments had no potential.
“But when we have access to medicines, we want to make sure that they’re safe and effective, and we want to make sure that there’s adequate evidence for them,” he said.
“The absence of evidence here really does not justify the widespread use of these medicines.”Challenges studying cannabinoids and psychedelics
The “gold standard” in medical research is a double-blind clinical trial, where participants don’t know whether they’re receiving a treatment or a placebo.
But cannabinoids and psychedelic drugs are difficult to study because they can’t easily be substituted for placebos, according to Dr Wilson.
“Participants usually know what they’re taking. So this can influence the results.”
Psychedelic mental illness treatment in state of confusion
To compare like for like, the authors of first JAMA Psychiatry study examined all publicly available clinical trials on psychedelics and depression.
Then they compared these trials only with antidepressant trials where participants knew what they were being prescribed so everyone was aware of what they were taking.
Sam Moreton, a lecturer in psychology at the University of Wollongong, said it was not surprising the psychedelics did not outperform antidepressants.
“The hype around psychedelic therapy has consistently run ahead of what the evidence actually supports,” Dr Moreton said.
“There are good theoretical reasons to think psychedelic-assisted therapy could help with depression and other mental health conditions, and I think it’s absolutely worth researching properly.
“But the field has serious methodological problems that have been well documented.”
Psychedelic therapy’s ‘slippery slope from hope to hype’
He said the second JAMA Psychiatry study was “methodologically careful”, using a low dose of psilocybin as a control, as well as a full dose and a placebo, to try and keep patients ignorant of which treatment they were receiving.
But 86 per cent of participants could still accurately guess which group they belonged to.
Dr Wilson said more research, such as the trial published in JAMA Psychiatry, was important for understanding the effects of these treatments.
The TGA rescheduled psilocybin and MDMA in 2023, making it easier for patients to access the drugs as medicines.
“I think we should be very wary of psychedelic-assisted therapies going down the same path as medicinal cannabis,” Dr Wilson said.
Combining psychedelics with psychotherapy
Susan Rossell, a neuropsychologist at Swinburne University of Technology who has run trials on psychedelics and depression, said she wasn’t surprised by the first JAMA Psychiatry paper’s findings.
Professor Rossell said current research on psychedelics needed to focus more on identifying which conditions, and which patients, would respond best to these therapies.
If you or anyone you know needs help:Lifeline on 13 11 14Kids Helpline on 1800 551 800MensLine Australia on 1300 789 978Suicide Call Back Service on 1300 659 467Beyond Blue on 1300 224 636 or its COVID-19 support service 1800 512 348Headspace on 1800 650 890ReachOut at au.reachout.comCare Leavers Australasia Network (CLAN) on 1800 008 774Brother to Brother on 1800 435 799
She added that many clinical trials of psychedelics the study reviewed lacked appropriate psychotherapeutic support.
“Having watched at least a hundred people go through this, making sure that you have qualified psychotherapists that can really help them unpack their experiences, and they don’t go away more lost than they were originally, is absolutely critical,” Professor Rossell said.
“We’ve had a couple of people come through our programs and actually relapsed. So I guess we could say that we’ve made them worse, which is awful.”
She predicted that research that included thorough psychotherapy alongside psychedelics would produce more evidence in their favour.
While she supported psychedelics as a potential therapy for depression, Professor Rossell said the treatments needed to be approached with caution and after other treatments had failed.
“There are safety issues, whichever intervention that you take on board. And there are some very tried and tested interventions already existing for a lot of mental health conditions,” she said.
“The reason why we’re working on these experimental interventions is because there are people that are not getting better with what we’ve got, but this is should certainly never be a person’s first foray into a mental health intervention.”
Cannabis prescriptions for depression lack evidence
Medicinal cannabis was first legalised in Australia in 2016.
“Medicinal cannabis originally had many hoops to jump through, like psychedelic-assisted therapies do in Australia now. But in 2021, things streamlined and it became much easier to access,” Dr Wilson said.
His study followed a similar process to the first JAMA Psychiatry study, examining clinical trials on cannabis and cannabinoids published between 1980 and 2025.

Australia allows use of cannabis-derived pharmaceuticals within strict guidelines. (ABC North Coast: Catherine Marciniak)
While they found tentative evidence that suggested cannabinoids could help treat some conditions, such as Tourette’s syndrome and insomnia, they found no evidence it could treat depression, anxiety or PTSD.
“Those three are quite important because they’re three of the leading mental health conditions for which they’re prescribed,” Dr Wilson said.
“In fact, there was actually not a single randomised controlled trial that examined cannabis use for the treatment of depression, which is really concerning.”
Both cannabis and psychedelics can make some mental health conditions, such as psychosis, worse, according to Dr Wilson.
“There are risks in taking these medicines, so we need to make sure that we get this one right.”