Brain organoids were first developed in 2013 by researchers in Austria. Over the past decade, they’ve become a widely used tool for studying some of the most treatment-resistant disorders of the human mind, including autism spectrum disorder, schizophrenia, and Alzheimer’s disease. Their value lies in offering a window into human brain biology that would otherwise be entirely inaccessible to researchers.
These structures begin as single cells, sometimes stem cells, sometimes skin cells that undergo a chemical process to become stem cells, before developing into structures containing millions of neurons. They typically represent specific regions of the brain, such as the thalamus, in simplified form. Scientists have since gone further, connecting multiple organoids together into what are called assembloids, interconnected systems designed to model broader biological features. One of the most advanced, built by Stanford University professor of psychiatry and behavioral sciences Sergiu Pașca and his team, connects four types of organoids to replicate a pain sensory pathway, linking brain organoids to a spinal organoid.
“Mini Brain” Is a Misnomer Scientists Are Quick to Correct
Despite the nickname that has attached itself to these structures in the popular imagination, researchers who work with organoids are consistent in pushing back against it. According to Pașca, “these models are not miniature versions of the brain. They are simplified, developmentally immature, and lack many defining features of an actual brain“, among them a vascular system and any form of sensory input.
The numbers make that distance concrete. Madeline Lancaster, the developmental neurobiologist at the Medical Research Council Laboratory of Molecular Biology in the UK who developed the first organoids during her postdoctoral work in Austria, notes that these structures contain at most only 0.002 percent of the neurons found in a human brain.
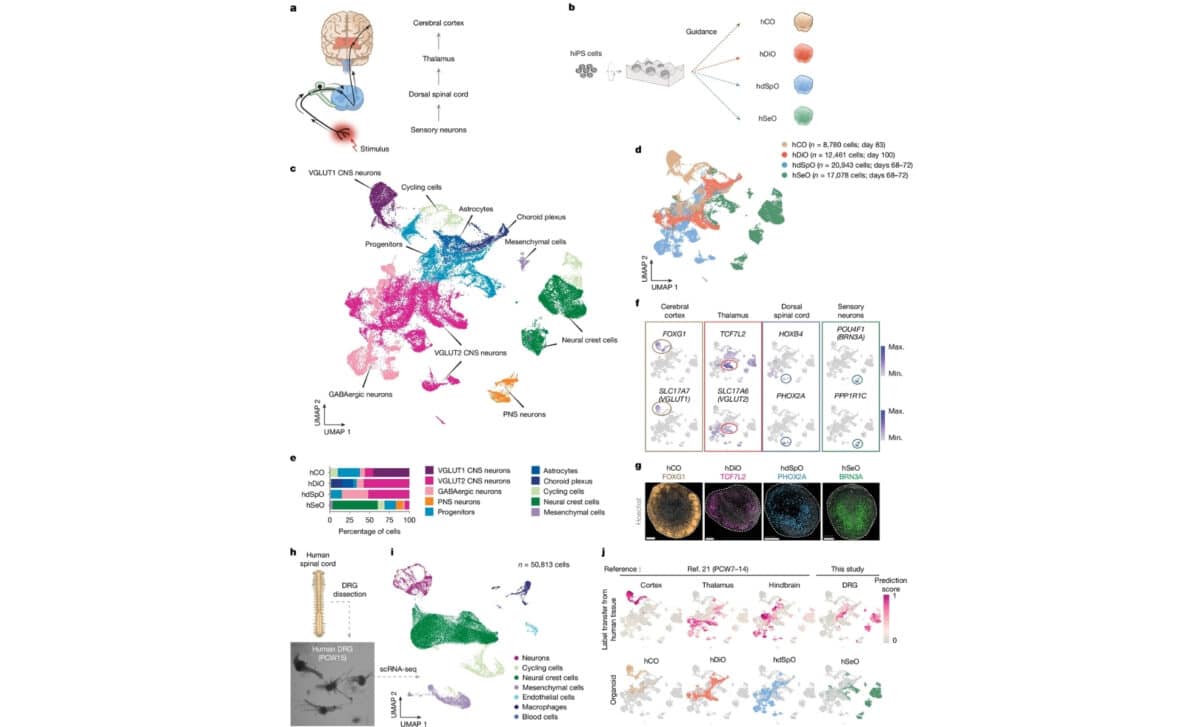 Generation from hiPS cells of components of human ascending sensory pathway – © Nature
Generation from hiPS cells of components of human ascending sensory pathway – © Nature
For Lancaster, scale and physical integration are two of the thresholds that matter most as the technology develops. “If technology arose that could enable organoids to develop to a much larger size, say 1,000-fold larger, and start to form the proper shape and structure, and be integrated in some sort of embodied context, then we should reconsider this,” she said.
On the question of consciousness, a word that follows organoid research like a shadow, the current scientific position is cautious but firm. Alta Charo, professor emerita of law and bioethics at the University of Wisconsin Law School, acknowledges that “there is still substantial debate about both the definition of consciousness and, however defined, what methods could be used to measure it.” But as organoids currently exist, she says, “we can comfortably say there is no reasonable possibility of anything remotely like consciousness.“
The More Pressing Concern: Putting Human Organoids Into Living Animals
Organoid consciousness may dominate public discussion, but experts point to a different frontier as the more immediate ethical challenge, the transplantation of human organoids into the brains of living animals. In 2022, Pașca and his team published research describing the first successful transplantation of human organoids into the brains of newborn rats, where the organoids integrated into the animals’ neural tissue and influenced their behavior. The resulting organisms are referred to as chimeras.
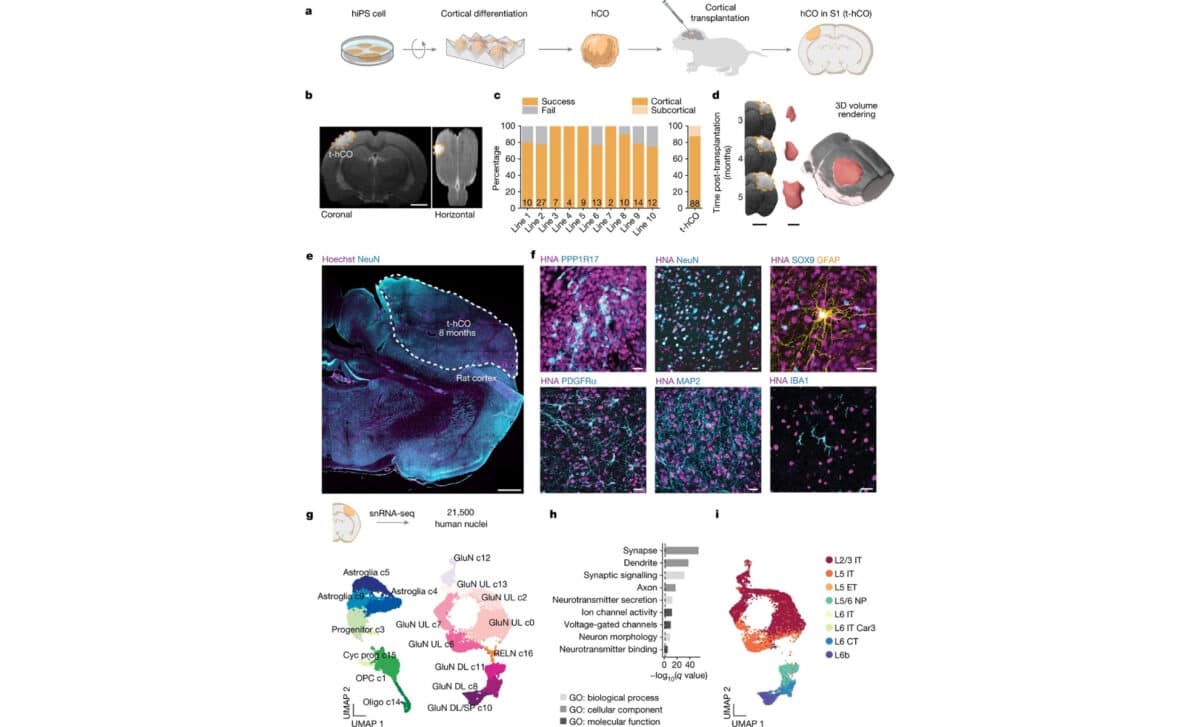 Transplantation of human cortical organoids in the developing rat cortex – © Nature
Transplantation of human cortical organoids in the developing rat cortex – © Nature
According to Lancaster, “transplanting organoids into living animals does carry important ethical concerns, mainly around animal welfare. That’s not because of the organoids themselves, but rather because of course animals do have those features of actual brains that we should care about and that suggest at least some level of consciousness.”
The public perceives this differently still. John Evans, professor of sociology and co-director of the Institute for Practical Ethics at U.C. San Diego, has observed that lay audiences tend to view organoids as extensions of the individual humans who originally provided the cells, a view consistent, he notes, with how people regard donated blood, tissue, and solid organs. On chimeras specifically, Evans points out that “while scientists and ethicists tend to not consider there to be a fundamental moral divide between humans and animals, the general public does.” “Therefore, mixing humans and animals — particularly in the brain that is seen as the core part of the human — is more ethically fraught,” he added.
A Scientific Community Watching Its Own Work Closely
Institutional oversight has not been absent from this conversation. In 2021, the U.S. National Academies of Sciences, Engineering, and Medicine published a report addressing the ethics and governance of human brain models, organoids included. The report concluded that current organoids “do not meet any current criteria for consciousness and awareness,” while stating that as they become more complex it will “be essential to revisit these questions.”
In 2025, Pașca, Charo, and Evans co-authored a paper calling on the global scientific community to monitor the field’s progress as it moves forward. The paper reflects a collective recognition that the pace of laboratory innovation demands structured, ongoing oversight rather than reactive policymaking.
Running alongside the calls for caution, though, is a parallel argument for why the research must continue. According to Popular Mechanics, experts describe a genuine ethical imperative on the other side of the ledger: modeling the brain and its disorders has the potential to alleviate significant human suffering. Pașca puts it directly. “Their unique value comes from giving us access to human brain biology that is otherwise inaccessible,” he said, “allowing us to study disease processes directly in human cells and tissues and to test potential therapeutics.“