February 4, 2026 — 11:30am
Save
You have reached your maximum number of saved items.
Remove items from your saved list to add more.
Save this article for later
Add articles to your saved list and come back to them anytime.
Got it
AAA
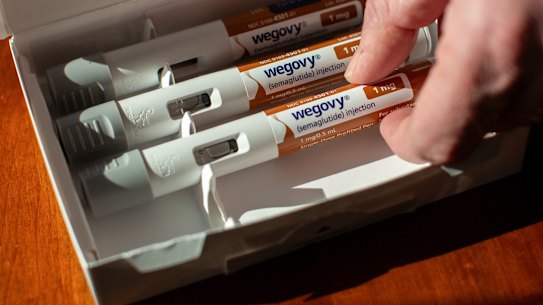
When Kacey Martin started taking weight-loss medication in June in consultation with her health providers, she experienced immediate relief.
“It reduced the food noise,” said Martin, who has previously experienced bulimia along with binge and restrictive eating. “I wasn’t so preoccupied in my head with food, which gave my brain space for all of the other things that happen in life.”
 Kacey Martin has a history of eating disorders and has started using GLP-1s.
Kacey Martin has a history of eating disorders and has started using GLP-1s.
But before long, the 33-year-old Sydney woman noticed the return of problematic behaviours such as purging.
“I did feel this strong urge to go back to body-checking and weight-checking … weighing myself almost daily, or multiple times a day,” she added.
“That psychological preoccupation with my weight has come back for me and gotten worse.”
As GLP-1 drugs become more widely available in Australia, experts are calling for stricter prescribing rules, eating disorder screenings and additional medical support for patients due to concerns they are triggering new eating disorders in some patients, while sending those with a history of anorexia into relapses that require hospital care.
Dr Terri-Lynne South from the Royal Australian College of General Practitioners is concerned about patients developing what’s known as atypical anorexia while using weight-loss medication.
Atypical anorexia involves someone who has a history of living in a larger body becoming preoccupied with weight and engaging in excessive dieting and exercising.
“We need to be very mindful of whether we are setting people up to have an unhealthy relationship with food,” said South, who specialises in obesity management.
“The medications can be prescribed appropriately and in doing so, actually cause someone to have disordered eating or an eating disorder.”
South also warned that inappropriate prescribing (particularly through telehealth) and a lack of support could also cause patients to shift from experiencing one type of eating disorder to another.
“We need to watch this space – that we’re not taking someone from a binge-eating disorder to atypical anorexia.”
She’d like to see patients have a face-to-face consultation with a doctor before being prescribed the medication as well as improving access to dietitians, psychologists and exercise physiologists.
 Josephine Money is a dietitian who specialises in eating disorders.Alex Coppel
Josephine Money is a dietitian who specialises in eating disorders.Alex Coppel
The Australian Health Practitioner Regulation Agency (AHPRA) has taken regulatory action against doctors, pharmacists and nurses who have inappropriately prescribed or supplied prescriptions to patients with eating disorders.
In some instances, the inappropriate prescribing of GLP-1 medicines – which has been primarily linked to telehealth providers – has suppressed the hunger of patients with anorexia, resulting in emergency hospitalisations.
“We have seen examples of patients admitted to hospital due to inappropriate prescribing of weight-loss medication when a thorough consultation would have identified that the prescribing [was] risky for that patient,” an AHPRA spokesperson said.
They said practitioners were required to undertake a comprehensive assessment of patients before prescribing weight-loss medication, which considers their vulnerabilities such as disorder eating or body image concerns.
Kacey Martin, who is completing a PhD at the University of NSW into eating disorders among Maori people in Australia, said she’d love to be able to afford a therapist to work through some of the return thoughts she has experienced since taking weight-loss medication.
“People often jump between eating disorders,” she said.
“We shouldn’t just assume there’s no risk for restrictive eating problems in people with binge-eating or bulimia.”
Dietitians Australia spokeswoman Josephine Money also said GLP-1 medications could make it difficult for many people to eat adequately.
“A starved brain has increased thoughts about food, increased anxiety, fear and drive for control; this can be the basis of typical anorexia cognitions,” she said.
Money, who runs a multidisciplinary clinic in Melbourne’s north that specialises in eating disorders, said current evidence in GLP-1 use with binge-eating was positive but that more extensive research was needed.
She said the medication could be useful in some people with binge-eating disorder if they were paired with “wraparound” support.
This might involve assistance from dietitians and mental health clinicians to minimise the risk of malnutrition and developing restrictive eating disorders such as anorexia.
In the short term, malnutrition can affect hormones and cognitions, while it can impact bone density in the long term.
Money estimates that about 40 per cent of her clients are either taking GLP-1s, considering taking them or curious.
Eating disorder groups say it’s too easy for patients with disordered eating to deliberately overestimate their body mass index in online questionnaires to gain access to the medication through telehealth.
“Anecdotally, we have heard reports of people exaggerating their weight when seeking these medications via telehealth, and that makes it difficult for providers to know if the medication is warranted, particularly if there is no face-to-face contact with the patient,” said Butterfly Foundation spokeswoman Melissa Wilton.
“We have also heard of cases where potential patients aren’t even screened by a doctor, but are ‘pre-approved’ and prescribed medications based on just a phone call with a purported nurse.”
The Butterfly Foundation’s telephone hotline has received a steady stream of calls from people using weight-loss medications who have an eating disorder, as well as from carers who are concerned about the mental and physical health of their loved ones who have been prescribed the medication.
For confidential & free support for eating disorders call the Butterfly National Helpline on 1800 ED HOPE (1800 33 4673) or visit www.butterfly.org.au to chat online or email.
Make the most of your health, relationships, fitness and nutrition with our Live Well newsletter. Get it in your inbox every Monday.
Save
You have reached your maximum number of saved items.
Remove items from your saved list to add more.
![]() Henrietta Cook is a senior reporter covering health for The Age. Henrietta joined The Age in 2012 and has previously covered state politics, education and consumer affairs.Connect via X, Facebook or email.From our partners
Henrietta Cook is a senior reporter covering health for The Age. Henrietta joined The Age in 2012 and has previously covered state politics, education and consumer affairs.Connect via X, Facebook or email.From our partners