The Covid Inquiry’s latest reports have made one thing brutally clear: the first year of the pandemic – particularly the second Covid wave in the winter of 2020/21 – was devastating. And much of that devastation was avoidable. Taken together, the evidence from NHS staff, bereaved families and the Inquiry’s findings on government decision-making show both how bad it was and how it could have been different.
In this post I look at four things: what the first year did to the NHS, what it did to the people working in it, what it did to the families left behind, and what the Inquiry shows about how much of it could have been prevented.
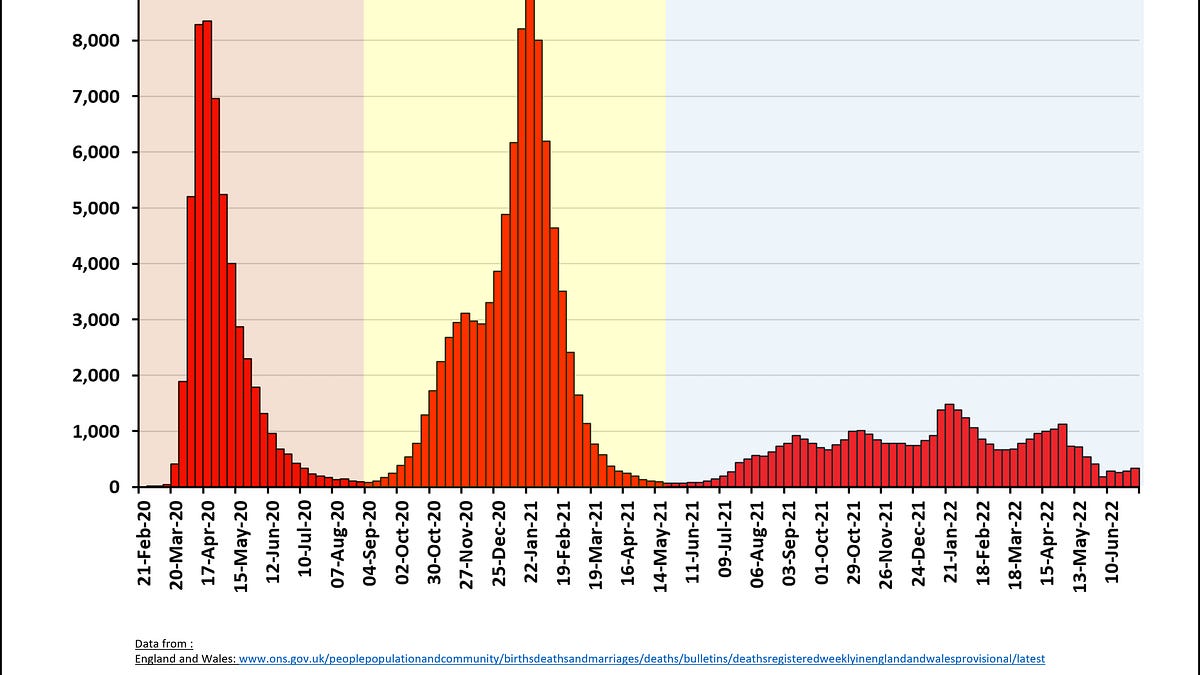
However bad the first wave was in England – and it was awful – the second wave was worse. More than twice as many people were admitted to hospital with Covid in the second wave compared to the first wave.
Critically-ill Covid patients filled our ICUs, pushing the units over their limits, and staff over theirs.
“The healthcare systems coped with the pandemic, but only just. On a number of occasions, they teetered on the brink of collapse and only coped thanks to the almost superhuman efforts of healthcare workers and all the staff who support them.” – Baroness Hallet, Introduction to the Module 3 report, page x.
The word “coped” is doing a lot of work in that sentence. Baroness Hallet goes on to say:
“Healthcare workers and support staff were obliged … to work under intolerable pressure for months on end. Some patients suffering from Covid-19 did not get the quality of treatment they needed and some non-Covid-19 patients had their diagnoses and treatments delayed to the point where their conditions became untreatable.”
NHS staff were among the most exposed people during that first year of the pandemic. They had neither the protection of effective treatments or – for the first 9 months – a vaccine. And this had consequences.
Healthcare workers were much more likely to have been infected – the ONS infection survey found that by June 2020 16% of healthcare workers in England tested positive for Covid antibodies compared to 7% of the overall population.
Compared to non-key working age adults, healthcare staff were much more likely to die in that first year. For those who survived, Long Covid was a risk. According to the gold standard ONS infection survey, by April 2021, 4% of all healthcare workers reported ongoing symptoms for at least 4 weeks and almost 3% for more than 12 weeks. Healthcare workers were the occupation with the highest rates of reported Long Covid out of all employment sectors. It contributed (and still is contributing) to thousands of NHS staff unable to work for months.
Beyond the physical tolls of Covid infection, the mental health of NHS staff suffered during those terrible first two waves. Module 3 reports that by April 2021 half of NHS staff said work or study had harmed their mental health; and by November 2021 64% were suffering from a work- or study-related mental health condition.
Among intensive care staff in England in January 2021, 52% reported symptoms consistent with severe depression and 47% with probable PTSD. Repeated surveys found 12% to 15% reporting suicidal ideation or thoughts of self-harm. Not only is this a tragedy for NHS staff, but it is directly associated with worse patient care.
The distress experienced by NHS staff was more than burnout – it was also the impact of moral injury, where “sustained moral distress leads to impaired function or longer-term psychological harm”. The Inquiry found that 80% of healthcare staff reported having to act in ways that conflicted with their values – for many front line staff this happened every day.
This devastating, emotional, 2-minute clip of the oral evidence from Professor Kevin Fong discussing his hospital visits at the height of the second wave perhaps explains it best.
The “unimaginable scale of deaths” that Professor Fong talks about in the clip were people – people who left behind devastated loved ones up and down the country. There have been more than 200,000 Covid-related deaths in England to date; 140,000 of them were during the first two waves.
The final set of oral hearings for the Covid inquiry were given by the bereaved. Some of their stories are also captured in the Inquiry’s “Every Story Matters” collection. The collection explained how many bereaved families and friends said how distressing it still is to think of their loved ones not understanding why their family and friends were not with them at the end.
“I cannot move beyond my trauma, I cannot move through this grief…my father died from the effects of isolation, from the heartbreak of not being able to see his wife and family, from the lack of care and love he should have so rightfully received.” – Bereaved family member, Every Story Matters
“There’s been about 6 or 7 instances where he texted us to say goodbye. We would try and phone or text back but, you know, his texts, because he couldn’t hold his phone very well, were often a little bit confusing to us. The other thing was he was so weak at times, he couldn’t pick up his phone…he’s bedridden, he can’t move…he can’t access any forms of communication and they [healthcare professionals] were so busy when often he would press the bell, and nobody would come.” – Bereaved family member, Every Story Matters
The Inquiry makes clear that the scale of this suffering was worsened by political failure.
This is where the findings of Module 2 on government decision-making are so important. In meticulous detail over two volumes, the overall conclusion is that the scale of deaths in the first wave could have been much lower and the devastating second wave could have been largely avoided. Tens of thousands of deaths could have been prevented.
The Module 2 report lays out the missed opportunities, delayed decisions, a refusal to learn, a downplaying or failure to believe advice from SAGE, and a general unseriousness on the part of government.
Professor Edmunds, who served on the SAGE modelling subgroup Spi-M, testified that the failure to act to control the second wave “was not because of a lack of situational awareness or knowledge of how to control it. We let this second wave happen.” . Professor McLean, now the UK’s Chief Scientific Advisor, described it as the worst period of pandemic, saying:
“We could see what was coming and could not understand why the government did not act upon the science advice by introducing effective interventions”
This isn’t speaking with the luxury of hindsight – witness after witness testified that SAGE was warning what was coming at the time. And it wasn’t just SAGE. The Academy of Medical Sciences published a detailed report in July 2020 (shared with the government via SAGE) on the need to prepare for a challenging winter, including advice on NHS resilience, contact tracing, and public health mitigations. Indie SAGE too published many reports that summer and autumn, on how to make contact tracing more effective, on how to improve testing, on safer return to work and study, the need to support people isolating. We highlighted the urgency of what was happening in the lead up to Christmas 2020 as things were spiralling out of control, and called for an emergency national lockdown almost two weeks before the government acted.
So it is not simply that mistakes were made under pressure; it is that failing to prepare over the spring and summer of 2020 and then to act quickly as the situation worsened transferred risk and suffering onto hospitals, staff, patients and families.
What makes it even more tragic is that the UK was the first country in the world to start vaccinating people – in early December just as the second wave was turbocharged by the new alpha variant. Our vaccine rollout was phenomenal – by mid-March 2021, over 25 million people had received at least one dose of Covid vaccine, which included over 95% of all adults over 65 years old. Early evidence was that even one dose reduced the chance of death by over 80% in older adults.
Imagine the lives that could have been saved had we managed to delay the next wave until after our population was vaccinated. Actually, we don’t need to imagine – countries that avoided significant waves until after their populations were vaccinated saw far fewer Covid deaths.
The world has moved on, plunged into crisis after crisis and there seems to be a collective determination to forget and never speak of the pandemic. But to ignore the findings of the Inquiry – to refuse to learn from the evidence and the pain – disrespects the sacrifices of those who held key services together and those who died. It would devalue all of us – and leave us as unprepared for the next pandemic as we were for this one.