A jury’s recent $18 million verdict in San Diego, later cut in half by California’s medical malpractice regulations, illustrates changes to a state law that limited payments for more than 50 years.
The case, which seeks compensation for a botched brain surgery that caused a debilitating stroke in an otherwise healthy patient, shows how increases in long-standing caps on “non-economic” damages, and on the fees that attorneys receive if they win, have changed the legal landscape statewide.
These changes are the result of Assembly Bill 35, legislation that took effect in 2023, the same year that Phuong Ho, 54, began experiencing minor discomfort in her head. Medical imaging revealed a tumor growing on her pituitary gland. Told that the mass could eventually grow large enough to impinge upon her nearby optic nerve, she underwent minimally invasive surgery at Sharp Memorial Hospital on Jan. 26, 2023.
Court records indicate that Dr. Sohaib Kureshi, a board-certified neurosurgeon affiliated with several San Diego County health systems, performed the surgery after an ear, nose and throat surgeon dissected the approach path, operating through an incision in Ho’s nasal passage.
Though court records show that there is significant disagreement about how Ho’s injury happened, there is no question that at some point her carotid artery, which passes very near the pituitary at the base of the brain, was damaged. The injury robbed the left hemisphere of her brain of blood flow, triggering a debilitating stroke.
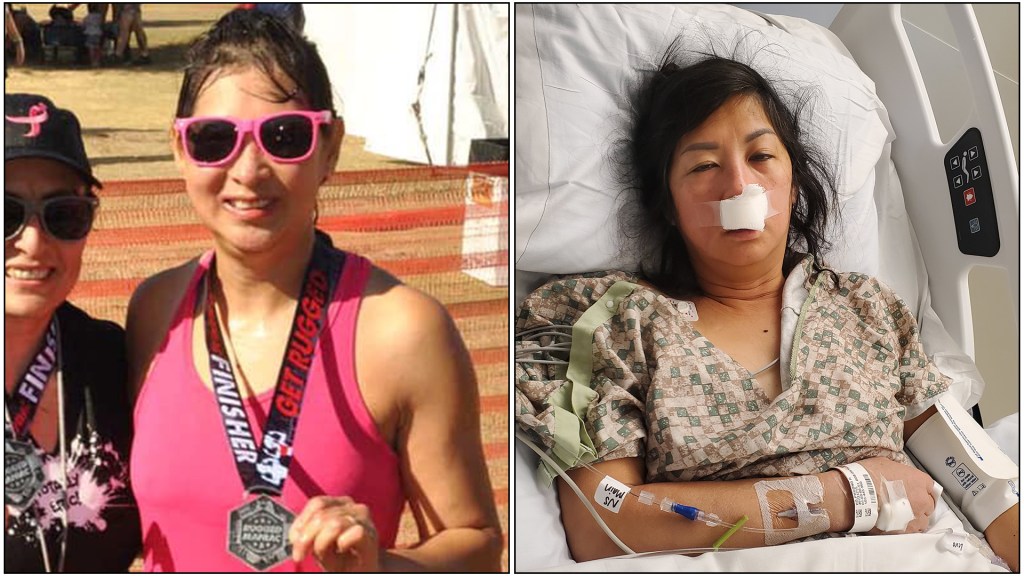
This unintended injury caused partial paralysis of the right side of Ho’s body. Though her condition has improved since the day of the surgery, her legal team argued in court that she will never be the same. A certified public accountant who worked as a financial manager for the San Diego Association of Governments, her civil lawsuit, filed in January 2024, notes that she was a healthy 52-year-old woman when she had the surgery. The stroke took away a very active lifestyle that included marathons and dragon boating, according to her attorney, Robert Vaage.
 Phuong Ho clears an obstacle at the EPIC Series Obstacle Challenge in San Diego. (VAAGE LAW)
Phuong Ho clears an obstacle at the EPIC Series Obstacle Challenge in San Diego. (VAAGE LAW)
In court, Vaage, who collaborated on the case with attorney Christopher Hendricks, made the case to jury members that Ho will need medical care for the rest of her life and is highly unlikely to resume her career.
“She started off with the entire right side of her body being paralyzed,” Vaage said. “Now that she has recovered, she can walk with a noticeable limp.
“She’s right-hand dominant, but she still can’t use her right hand; she’s had to learn to use her left. She has continuing cognitive and memory issues that have impacted her ability to speak and to think clearly.”
Vaage said that Ho declined to discuss the situation due to ongoing speech difficulties.
A possible appeal
There is ongoing disagreement from Kureshi’s side of the case.
During the trial, his legal team introduced an alternate cause of the carotid injury that caused the stroke, suggesting that the blood vessel may have been “stuck to the tumor” and thus ruptured as the benign growth was removed. Court papers indicate that Kureshi rejected the notion that he accidentally cut into the vessel because he was using a blunted cutting tool called a ring curette.
In an email, Clark Hudson, an attorney for the defense, said that this matter is not finished.
“Dr. Kureshi is one of the best neurosurgeons in San Diego,” Hudson said. “The surgery was to remove a tumor that was pressing on the patient’s optic nerves. The surgery he performed on this patient has known complications, to include strokes, (of) which the patient was informed.”
The attorney said that while the jury “did the best they could with the information allowed in evidence,” there will be an effort after trial to allow information that “would have reached a different result.”
“We will be asking the judge to re-evaluate whether the exclusion of evidence was prejudicial to the defense,” Hudson said. “If the Judge agrees it was prejudicial, then he will likely grant a new trial.
“If that request is denied, then we will likely file an appeal.”
The defense did not specify which evidence it believes was inappropriately excluded.
The new math of malpractice
Legal wrangling notwithstanding, the court formally recorded the jury’s verdict in mid-January, checking “yes” when asked whether Kureshi was “negligent in his care of Phuong Ho?”
A total of $5.4 million is awarded in compensation for Ho’s future medical expenses, with an additional $2.4 million for lost earnings, bringing the total economic damages to $7.8 million.
The balance of the $18 million that the jury awarded is non-economic damages: $1.7 million for Ho’s past “physical pain (and) mental suffering” and $7 million for the same damages in the future. Her husband, Trinh Nguyen, received a $1.5 million award for the loss of his wife’s companionship.
Here is where the state’s malpractice damage cap takes effect. Before AB 35, the Medical Injury Compensation Reform Act, often called MICRA, automatically reduced all non-economic damage awards to $250,000 per occurrence. The amendment that took effect in 2023 increased that limit to $350,000 per occurrence and adds $40,000 each year for 10 years, eventually reaching $750,000 for injury cases and $1 million for awards made after a patient’s death. Offering a larger cap for fatal cases is another change brought by AB 35. The injury cap reached $470,000 in 2026, the amount that was used in Ho’s case.
Juries are not told about these caps before they make rulings, meaning they have no opportunity to make their economic damage awards, which are uncapped, larger in compensation.
Under the cap, Ho’s total pain and suffering award falls from $8.7 million to $940,000, Ho and Nguyen each receiving $470,000, the updated cap on non-economic damages.
State law causes the total award to decrease by 51%, shrinking from the $18 million to just under $8.8 million. That’s $7.8 million in economic damages plus $940,000 for capped non-economic damages.
Remember, the amount juries award for economic damages, wages that will never be earned, and expenses that otherwise wouldn’t have been incurred, is uncapped. Juries are free to award a billion or a trillion if they feel it’s warranted, though judges can reduce awards considered to be beyond actual losses that a person actually experienced or will experience in the future
Attorney fees are taken from this reduced amount after caps are applied.
AB 35 also changed the fee structure that controls the amount that attorneys receive from jury awards and settlements.
Generally, malpractice cases are taken on contingency, meaning lawyers get paid only if they win monetary damages for their clients, and they must cover the entire cost of the action up front with no guarantee they will ever be repaid.
California law previously applied a graduated scale to the contingency fees that could be received: 40% of the first $50,000, 33% of the next $50,000, 25% of the next $500,000 and 15% of any amount that exceeded $600,000. AB35 eliminated the stepwise approach, instead allowing a 25% contingency fee for cases settled before a civil lawsuit or arbitration claim is filed and 33% after such legal actions are taken.
It is a significant difference in the financial reward available to attorneys willing to risk taking on malpractice cases on contingency. Applying the previous graduated contingency schedule to Ho’s $8.8 million reduced award, the contingency fee would have been about $1.39 million. Under AB 35, the fee jumps to about $2.9 million. Even taking into account that damage caps have increased from $250,000 before the MICRA update to $470,000, the increase in capped damages that awardees receive is significantly less than the increase to attorney fees. Compared to 2022, before AB 35 took effect, the non-economic damages cap was $250,000, a gain of $220,000 for each Ho and her husband with the new cap of $440,000.
Vaage declined to verify that math.
But he and Hendricks recently filed a petition in court arguing that the legal team should receive 40%, not 33%, of the reduced jury award, increasing their share from about $2.9 million to more than $3.5 million. If a judge grants the larger percentage, Ho’s take-home would decrease from $5.8 million to $5.2 million.
AB 35 does specifically allow attorneys to go beyond 33% if they can establish “good cause for the higher contingency fee.”
Vaage said that Ho agreed to a percentage greater than 33% in writing before he took the case.
Contingency calculus
An initial settlement offer of $2 million, the amount covered by Kureshi’s malpractice insurance coverage, Vaage said, was refused by the carrier without a counter-offered amount.
The investment in arguing a case in which the defendants were sure they would win, he said, was significant.
“That’s based upon the fact that we invested well over 1,000 hours of our time and approximately $300,000 of our money in a complex no-offer case,” Vaage said.
Did AB 35’s more than doubling of contingency fees and allowing an argument after trial for an even greater amount of compensation contribute to his willingness to take the case? The answer is yes.
“I would not have agreed to get involved in this case, understanding the complexity and the cost, if the MICRA cap and the attorneys fee provision hadn’t been changed,” Vaage said. “On a scale of one to 10 in terms of complexity, this case was a nine or a 10.”
The net effect, the attorney said, drawing on more than 40 years in malpractice law, is that more cases are likely to be taken on contingency than have been in the past.
“In my opinion, these changes in the law benefit patients who have been injured by malpractice much more than they do attorneys,” Vaage said in an email. “Without these changes, many malpractice victims would never have an opportunity to have their day in court.”
That is essentially the perspective circulated by the legal groups that pushed for decades to update MICRA’s limits, which had not been increased since the law passed in 1975. There has been a long debate about whether or not any caps at all are appropriate, with organizations representing doctors, such as the California Medical Association, resisting updates for many years.
While AB 35 was seen as something of a compromise, a comment on the bill from the Union of American Physicians and Dentists predicted that the bill “would increase health care costs for working families while raising the cost of medical malpractice insurance premiums beyond that which most physicians in private practice and small groups simply can afford, driving physicians out of private practice and exacerbating existing physician shortages.”
Is this scenario coming to pass? It is difficult to tell using publicly available data. Dr. Ted Mazer, a past president of the California Medical Association who is still involved in health care advocacy, said that it is a little early to see a new trend building. And that’s because, as Ho’s case shows, a medical malpractice case in which the injury occurred in 2023 is only now arriving at a jury decision.
“Have the increase in attorney fees and the increase of the cap really made that much of a difference?” Mazer said. “I would say we don’t know the answer, because cases that started in 2023 are just now going to trial, so we’ll have to see whether these changes drive more cases and bigger awards.”
Consumer Attorney of California, a statewide professional organization that was one of AB35’s largest backers, did not respond to a comment on the law’s effects so far. Californians Allied for Patient Protection, a coalition of medical providers that supported the bill but is generally dedicated to protecting MICRA, said in a short statement that the changes provide “fair compensation while preserving access to health care by keeping doctors, nurses and health care providers in practice and clinics open,” continuing to predict that an uncapped system would cause a reduction in medical services due to increased costs.