A brain-infecting parasite carried by rats and slugs — and capable of causing neurological illness in humans — has surfaced closer to home, prompting questions about whether it could spread north into Santa Barbara County.
Known as rat lungworm disease, or angiostrongyliasis, the parasite was recently identified in animals in San Diego County, including a case that led to the death of a wallaby at the San Diego Zoo in 2024. The finding — published this February in the Centers for Disease Control and Prevention’s peer-reviewed journal Emerging Infectious Diseases — has raised concern about its presence in Southern California ecosystems.
In Santa Barbara, local officials say the risk remains low.
“Not too worried at this point,” said Brian Cabrera, general manager of the Mosquito and Vector Management District of Santa Barbara County. “As far as we know, that particular creature is not found here in Santa Barbara County.”
That “particular creature” is a semi-slug — a key carrier of the parasite. Without it, the disease is unlikely to establish locally.
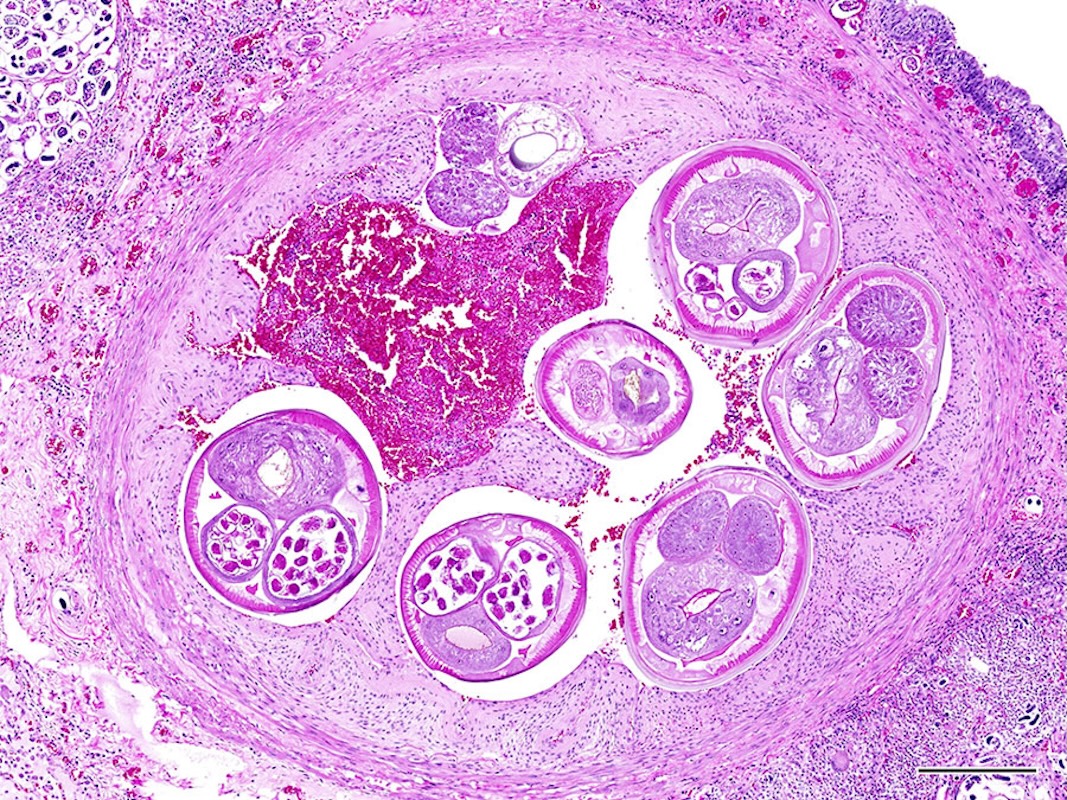
Rat lungworm disease is caused by the parasite Angiostrongylus cantonensis, which primarily cycles between rats and slugs or snails. Humans can become infected accidentally, typically by consuming contaminated produce or undercooked hosts.
Once inside the body, the parasite’s larvae can travel to the brain, causing a meningitis-like illness, or settle in the digestive tract, “similar to appendicitis,” according to Cabrera.
Despite its unsettling symptoms, the disease remains rare in the continental United States. In an email to the Independent, Santa Barbara County’s Public Health Department wrote that there are currently no confirmed human cases in California, though the parasite is established in Hawai‘i and parts of the Southeast.
Its spread is closely tied to globalization and environmental conditions — particularly the movement of plants. “The most likely method of getting up here would be through transport of infested plants or vegetables,” Cabrera said, noting that semi-slugs could hitchhike on nursery plants or produce brought from affected areas.
Even in places where the parasite is present, infection typically requires a chain of events: an infected rat, a slug or snail that consumes rat feces, and a human who unknowingly ingests the contaminated organism — or residue from it.
Prevention, officials say, is straightforward.
“Washing the fruits and vegetables” and maintaining basic cleanliness are key, Cabrera said, along with controlling rodent populations around homes and food sources.
Public health guidance echoed the advice and added: avoid eating raw or undercooked snails or freshwater animals.
In Hawai‘i, where the parasite is endemic, cases have been linked to unwashed lettuce, contaminated water, and even accidental ingestion of slugs. In areas where rat lungworm has taken hold, doctors are urged to recognize early symptoms — which can range from headaches and neck stiffness to more severe neurological complications — and consider treatment quickly. Case studies have shown that early intervention, often including anti-parasitic medication and steroids, can improve outcomes, particularly when the parasite has migrated toward the central nervous system.
Still, Cabrera emphasized that local conditions do not currently support the same level of concern. For now, the parasite remains a problem to watch — not one actively spreading on the Central Coast.