Florida’s healthcare challenges are often discussed in terms of shortages, insurance barriers, and burnout. Beneath all that lies a more fundamental problem: the way we deliver care in primary care offices is no longer serving patients or providers well.
As a licensed practical nurse and registered nurse with more than a decade of experience in primary care, I have worked inside the traditional clinic visit model. I have seen providers expected to manage increasingly complex patients in tightly scheduled, high-volume days. I have seen patients leave appointments confused or rushed—not because their provider didn’t care, but because the system didn’t allow enough time.
Now, as a future nurse practitioner, I believe the question Florida must ask is not simply how many patients we see—but how we see them.
The traditional one-patient-at-a-time, 10-to 15-minute visit model was never designed for the realities facing primary care today. Chronic disease, mental health conditions, obesity, diabetes, and multimorbidity require education, behavior change, coordination, and follow-up. These needs cannot be met by checking boxes, clicking through templates, and rushing from room to room.
Yet current practice and insurance policies often leave primary care providers with little choice. Reimbursement structures reward volume and documentation rather than value, forcing clinics to overload schedules simply to remain financially viable. Time spent educating patients, coordinating care, or addressing social determinants of health is rarely reimbursed adequately—despite being essential to good outcomes.
The result is predictable: providers burn out, staff turnover increases, and patients feel unseen.
Florida’s growing and aging population makes this model even less sustainable. Parts of North Florida, including the Big Bend region, face primary care access constraints, and even in Tallahassee, patients often experience long waits and limited appointment availability. When access is strained, rushing care only compounds the problem.
There is, however, a better way forward.
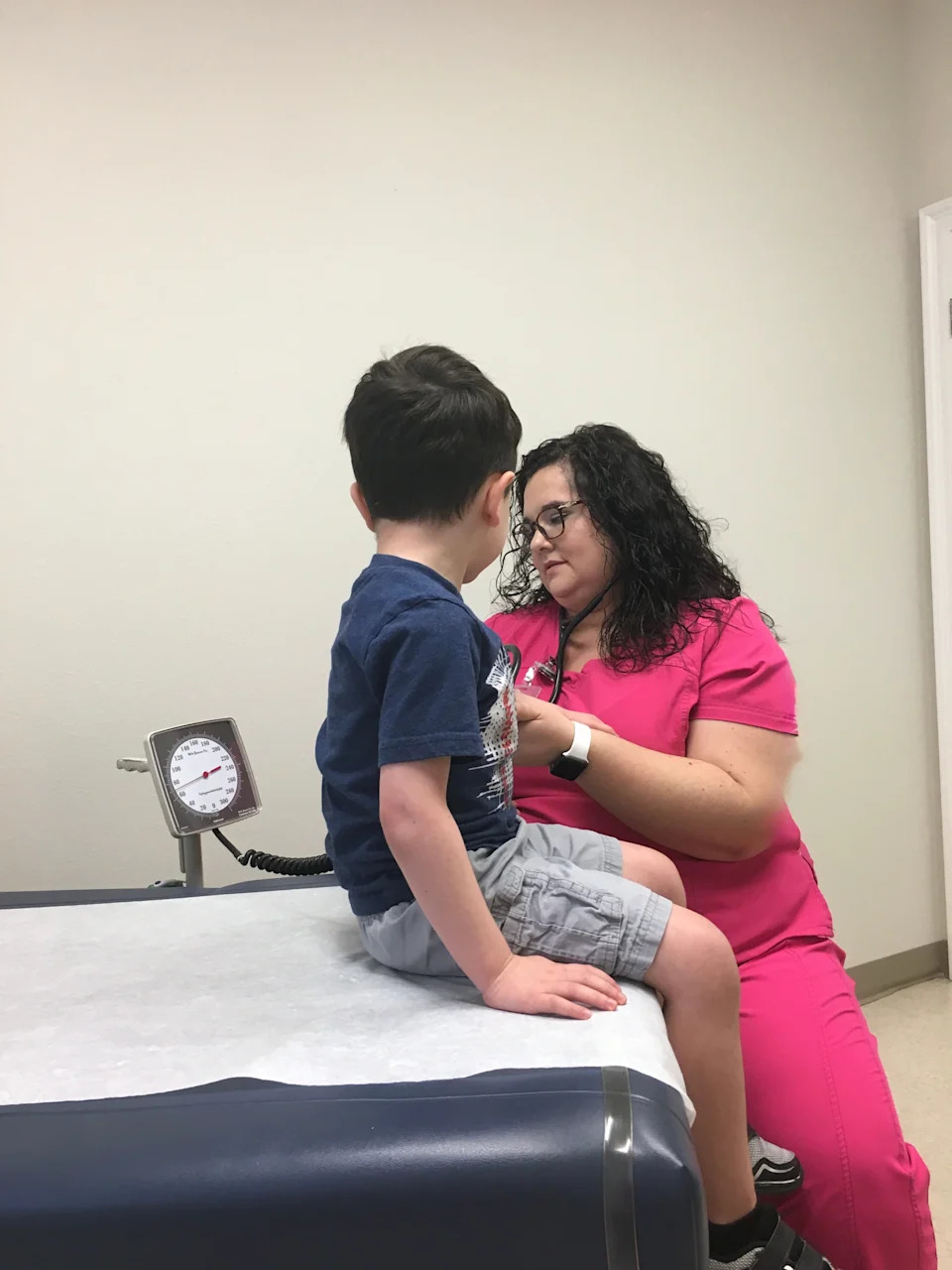
Rebekah Slack, DNP(c), BSN, RN with son, Micah Slack in 2019 checking blood pressure at his yearly well child exam.
Shared medical visits and team-based care models offer an alternative that better aligns time, outcomes, and sustainability. In shared medical visits, patients with similar conditions—such as diabetes, hypertension, or obesity—are seen together by a provider-led care team. These visits allow for extended appointment time, peer support, education, and meaningful discussion, while still addressing individual medical needs.
Evidence shows that shared medical visits can improve clinical outcomes, increase patient satisfaction, and reduce provider burnout. Importantly, these models do not replace individual care—they enhance it. They recognize that patients are not interchangeable and that meaningful care requires time, relationship, and context.
For these models to succeed more broadly in Florida, practice and insurance policies must evolve alongside them.
Stethescope image and healthcare costs
Any meaningful reform must include insurance policies that fully recognize nurse practitioners as primary care providers and reimburse them equitably for the same evidence-based care. When nurse practitioners are paid less or not recognized as independent providers, access suffers—especially in communities already facing shortages. Payment parity strengthens primary care capacity and supports innovative models like shared medical visits.
Primary care providers should not be forced to overload schedules to meet productivity targets that undermine quality. Reimbursement must reflect the real work of primary care—including education, coordination, and prevention—rather than rigid, outdated definitions of what constitutes a “billable” encounter.
When primary care is allowed to function as intended—preventive, relational, and team-based—patients benefit, providers stay engaged, and the healthcare system becomes more efficient over time.
Florida has an opportunity to lead by supporting care models that emphasize time, outcomes, and sustainability over volume. Shared medical visits and redesigned primary care workflows are not radical ideas—they are practical responses to a system that has outgrown its original design.
Progress does not require perfection. It requires the willingness to let go of models that no longer work and to invest in those that do.
Our patients deserve better; our providers need it and the future of primary care in Florida depends on it.

Rebekah D. Slack
Rebekah D. Slack is a future Doctor of Nursing Practice–Family Nurse Practitioner (DNP-FNP) at Florida State University. She is from Monticello, Florida, with 12 years of combined experience as an LPN and RN in primary care.
JOIN THE CONVERSATION
Send letters to the editor (up to 200 words) or Your Turn columns (500-550 words) to letters@tallahassee.com. Please include your address for verification purposes only, and if you send a Your Turn, also include a photo and 1-2 line bio of yourself. You can also submit anonymous Zing!s at Tallahassee.com/Zing.Submissions are published on a space-available basis. All submissions may be edited for content, clarity and length, and may also be published by any part of the USA TODAY NETWORK.
This article originally appeared on Tallahassee Democrat: Florida’s current primary care model needs to be reimagined | Opinion