Dr. Michael Brode, medical director of UT Health Austin’s post-COVID-19 program, speaks at City Hall on Thursday, March 12, 2026 in Austin. The City of Austin issued a proclamation declaring March 15 “Long COVID Day.”
Aaron E. Martinez/Austin American-Statesman
Six years ago, Austin and the world shut down as COVID-19 hit the United States and began to spread.
For many, the pandemic feels like it’s over, but for some people “the pandemic never ended. COVID never went away,” said Katie Drackert, co-founder of Clear the Air ATX, a group committed to raising awareness about long COVID and providing public spaces and residences with HEPA filters to mitigate the spread of viruses in the air.
Article continues below this ad
One in 19 people in the country is living with long COVID — a disease with more than 200 symptoms that can develop after an infection and currently has no known treatment or diagnostic test.
On Thursday, Austin City Council declared March 15 Long COVID Awareness Day. The action serves as a reminder that an estimated 42,000 people in Austin have long COVID, while also encouraging funding of long COVID treatment programs and support groups and promoting COVID-19 precautions.
“The pandemic is not over,” said Dr. Desmar Walkes, public health authority for Austin and Travis County. “There are still people day after day contracting COVID-19.”
Her goal is to help people lessen the chance of getting long COVID by reducing their chances of contracting the virus through vaccination, washing hands, staying home when sick and getting treatment early.
Article continues below this ad
Long COVID can cause multiple problems including worsening preexisting conditions, said Dr. Michael Brode, medical director of the Post COVID-19 Program at UTHealth Austin, the clinical practice of Dell Medical School.
Some of the common long COVID symptoms include fatigue, especially after exertion; brain fog; shortness of breath or difficulty breathing; chest pain or heart palpitations; fever; insomnia; dizziness; headaches; diarrhea or constipation; joint or muscle pain; a pins-and-needles feeling; and depression or anxiety.
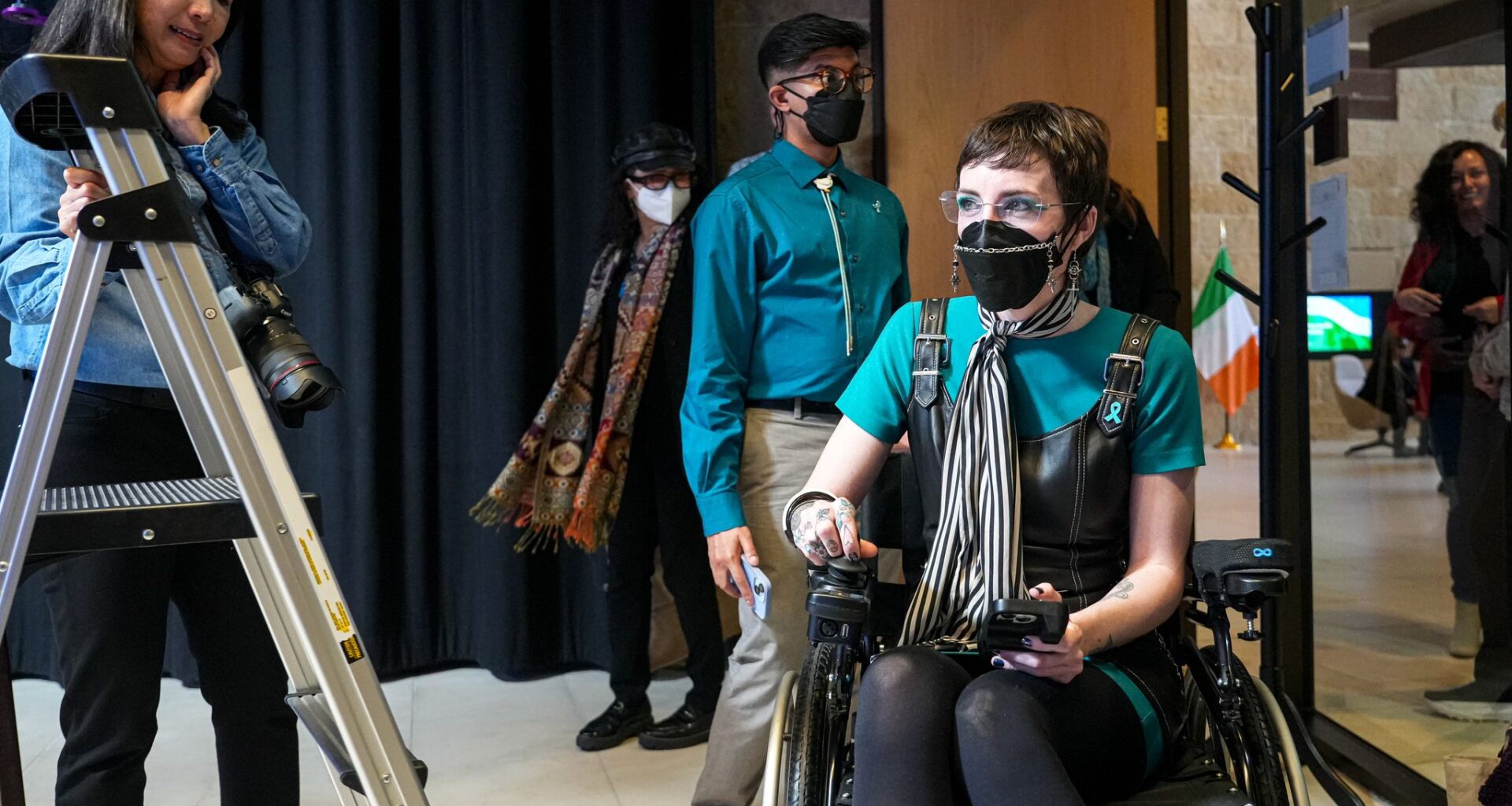
Katie Drackert, founder of Clear the Air ATX who lives with the effects of long COVID, enters the media room at City Hall on Thursday, March 12, 2026 in Austin. The City of Austin issued a proclamation declaring March 15 “Long COVID Day.”
Aaron E. Martinez/Austin American-Statesman
Living with long COVID
Long COVID is often very debilitating, Walkes said.
Article continues below this ad
Austin Council Member Marc Duchen, who presented the proclamation with Council Member Natasha Harper-Madison, said in addition to creating awareness, more support is needed for people with chronic illnesses, “which impact all aspects of our lives.”
Drackert was a working performance artist and a student when she got COVID for the first time in December 2021.
“It was bad,” she said, adding that doctors told her that if she hadn’t been vaccinated, she would have been hospitalized.
She was just getting over that infection when, six months later, she contracted it again. She has not recovered.
Article continues below this ad
She stopped being able to perform, dropped out of school and lost her job. She said she would have become homeless without support from friends. She now uses a wheelchair to conserve energy if she has to walk any distance.
Many fellow long COVID advocates have shared this experience.
Maggie Moore was a working archaeologist and otherwise healthy before she got COVID in July 2022.
“The symptoms never went away,” she said.
Article continues below this ad
She had a second infection in 2023 and had to stop working. She’s applied for Social Security disability payments, but has been denied twice. Long COVID has been recognized as a qualifying condition for disability benefits.
Now she wonders if her family should max out their credit cards or if she should take a job she knows she can’t do just to get a few paychecks before she has to quit because of her illness.
Moore and others connect through an online support group they founded: Long COVID Collective.
Lisa Noriega stopped working as a real estate agent and had to declare bankruptcy after contracting COVID for the sixth time. Now it’s difficult for her to walk across the room, and her memory has been affected.
Article continues below this ad
“Everything is harder now,” she said.
Rachel Madison was ready to start a career when she got COVID as she was graduating from college.
“I was super active, then everything went downhill,” she said. She moved back in with her parents in Austin.
“The disease brings real suffering,” she said. “… It steals joy. It devastates lives.”
Article continues below this ad
Why does long COVID happen?
COVID, and then Long COVID, are diseases of inflammation that affect the small blood vessels throughout the body, which is why it has so many symptoms.
People who have had very serious COVID infections have a greater chance of developing long COVID, Brode said. The risks increase with each infection.
Every infection comes with a 5% to 10% risk of developing long COVID, he said.
Article continues below this ad
People who are up to date on their COVID vaccinations have a lower chance of developing long COVID, he said. However, anyone who gets COVID — whether vaccinated or not, whether it’s their first infection or not, and whether the infection is particularly bad or more like a cold — still has a risk of developing long COVID.
Long COVID is not unique. Any infection can cause the body to have an overreaction of the immune system.
Symptoms like long COVID were recognized as far back as the 1890s in Russia during an influenza outbreak, Brode said. Other illnesses, such as Ebola and dengue fever, have been known to cause these lingering symptoms.
This post-infection syndrome is coming to light now because of the large number of people with COVID who continue to experience these symptoms.
Article continues below this ad
How is long COVID diagnosed?
Many doctors don’t recognize the pattern of symptoms as long COVID when a patient comes to them, Brode said.
“Many of my patients see six doctors before they see us,” he said. “They feel gaslit, like they are not being believed or taken seriously.”
Brode looks for the pattern of symptoms to make the diagnosis. Doctors also diagnose long COVID after ruling out other potential causes.
Article continues below this ad
Long COVID appears to be caused by the immune system continuing to attack the body even after the infection is gone.
How is long COVID treated?
About 50% of patients get better over time and return to their pre-COVID state. The rest do not fully recover, though they learn to manage the condition.
There’s no defined treatment. Instead, doctors take a holistic approach that includes managing physical symptoms, working with social workers to address patients’ needs, and cognitive therapy.
Article continues below this ad
They also work with patients on managing their energy levels.
“Texans are not wired to slow down and stop fighting it,” Brode said. “Pushing through and trying harder makes it worse.”
UTHealth Austin is part of a study testing a class of medications called biologics that are used for other autoimmune diseases such as rheumatoid arthritis.
Article continues below this ad