LYNCHBURG, Va. (WSET) — Getting in to see a doctor without a painful wait time is harder and harder.
For some of you in our viewing area, it’s nearly impossible without traveling out of the region.
A growing shortage of physicians is leaving communities with longer wait times, fewer options and serious concerns about access to care.
A CT scan in June 2025 left Wendy Barnes’ doctor concerned.

Wendy Barnes had to travel to Charlottesville to get testing in a timely manner (Photo: ABC 13)
“He said ‘I see some issues in your lungs and need you to see a pulmonologist in the next week or two’,” Barnes said. “I called, of course, and said I have a referral that I need to be seen right away to pulmonologist.”
At the time, the first appointment available in Lynchburg was in February 2026 — 8 months out.
“I was shocked,” Barnes said.
SEE ALSO: Local healthcare heroes stay overnight at Lynchburg hospital during winter storm
Healthcare workforce shortages are a growing problem for communities across Virginia and the U.S.
Primary care physicians, you know, the ones you go to see for your overall care, are diminishing.
Dr. Alex Krist is a physician and faculty member for Virginia Commonwealth University’s residency program.
“Our systems are broken and we need to fix the systems,” Krist said.

Dr. Alex Krist leading efforts to train, recruit and retain PCPs (Photo: ABC 13).
Krist sits on several task forces trying to find a cure the doctor shortage epidemic.
“I think across the nation and in Virginia, we have a shortage of primary care clinicians. And we have a shortage of specialists as well,” Krist said. “So there’s an inadequate workforce right now to help all the people in our communities.”

In 2019, a VCU Health study found there were 5,899 primary care doctors in the Commonwealth. In 2024 that number rose, a little, to 5,941.
Still, Dr. Krist said we need about 40% more to meet the current demand.
Dr. Hannah Shadowen led a recent VCU study looking into the problem published in 2025.
They found 44% of all neighborhoods in the Commonwealth don’t have enough physicians to care for the people who live there. That affects nearly 3.8 million Virginians.
“I found that there are not enough primary care doctors in general. And then specifically in rural communities,” Shadowen said.
Shadowen outlined the shortage with a heat map of Virginia.
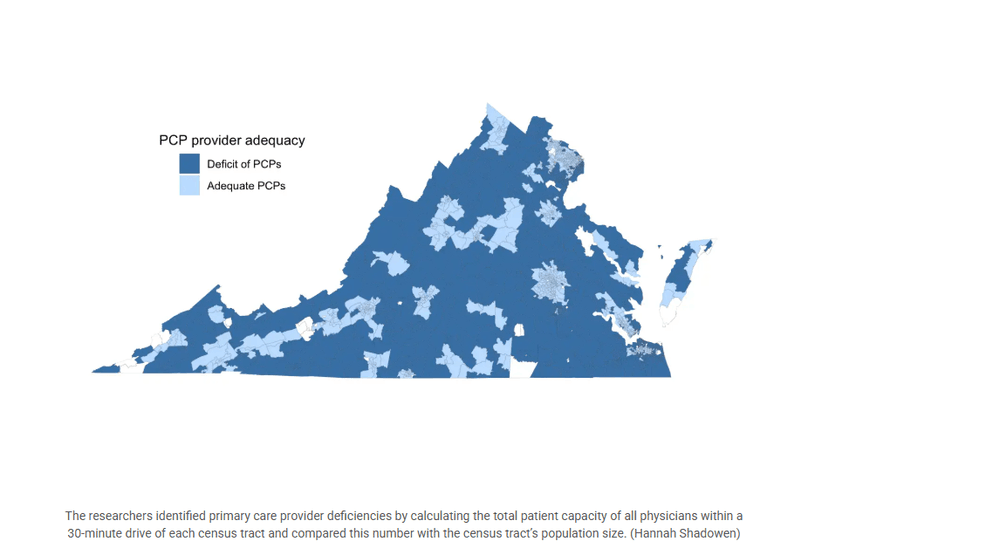 PCP shortage heat map in Virginia (VCU Health).
PCP shortage heat map in Virginia (VCU Health).
Sloan Albert, Chief Operating Officer at Centra, said it’s an obstacle for their health care system.
“It is a two-pronged problem. There aren’t enough (doctors) out there, particularly in certain specialties,” Albert said. “But I think the other is finding physicians that want to work in a rural environment.”
 Centra’s COO discussing the doctor shortage and what the health care system is doing to hire doctors (Photo: ABC 13).
Centra’s COO discussing the doctor shortage and what the health care system is doing to hire doctors (Photo: ABC 13).
Dr. Krist points to burnout, retirement and growing demand in healthcare as factors also putting a strain on the number of doctors available.
“So we have more people and the physician workforce hasn’t kept up with that,” Krist said. “So, I’ve been at my practice now 30 years. I’m a family doctor. I started out seeing young folks, and a lot of my patients have aged with me, and my community is older now too, as well. So we have a lot more folks who are living longer and healthier lives. But that also means that they have more medical needs as well. So there’s more need for medical services in many communities than there used to be.”
Unfortunately, there’s no perfect workaround for everyone. If you can’t wait to see a doctor, you may have to shop around out of the area.
Barnes ended up having to travel to UVA Health in Charlottesville for her testing.
They were able to get her an appointment in days rather than months.
Doctors diagnosed her with pulmonary fibrosis.
“It won’t get better, but at least they can start doing things the right way,” Barnes said.
The Association of American Medical Colleges estimates by 2032, the United States will be short by more than 55,000 primary care physicians.
Dr. Krist is working on ways to solve that deficit.
“I think some ways are to try and encourage more physicians to pursue primary care. As a discipline as opposed to specialty,” Krist said. “Then trying to help reduce burnout and help physicians practice better so that they’re happier and stay in practice longer.”

