It’s the kind of budget cut that draws outrage: rollbacks to a 50-year-old program that enables tens of thousands of Massachusetts seniors and people with disabilities to live independently.
But this time, the reductions didn’t come from politicians or bureaucrats. They came from some of the program’s own beneficiaries.
Program users, providers, and disability rights advocates involved with the state’s Personal Care Attendant program participated through much of 2025 in a state-assembled working group that recommended $32 million in cuts to the service, which provides help with activities such as dressing, eating, and bathing to about 56,000 people. MassHealth, which funds the program, expects to put the trims into effect this summer.
The cuts, necessitated by deep federal spending reductions, cap the number of overtime hours each attendant can work, as well as how long they can spend on meal preparation — changes that will force some users to scramble for additional services.
Getting stakeholders’ input helped reduce the pain of cuts to the PCA program, officials said, and it is a model Massachusetts expects to replicate as it seeks savings in other long-term care programs while limiting harm.
“There is an enormous amount of urgency precipitated by federal actions,“ said Mike Levine, assistant secretary for MassHealth. ”I suspect we will be putting that model to work in many different forms.“
MassHealth officials said they are forming similar working groups to look for savings from programs that provide adult day care and adult foster care, which provides continuous live-in care for seniors and those with disabilities.
These programs have to become leaner, state officials said, to survive federal spending reductions.
“It’s really hard to hold all these things together and see the solution for how we get through the next 10 years,” said Leslie Darcy, MassHealth’s chief of long-term services and supports.
There’s no other way to see it: Massachusetts is facing a fiscal cliff, the result of Congress’s $1 trillion reduction to Medicaid spending through 2034. That decision last summer exacerbated the state’s existing health care spending crisis, a consequence of growing costs and an aging population. The state already spends more than $22 billion on Medicaid, well over a third of its budget, and its largest cost driver. The lean years ahead are expected to batter hospitals, leave hundreds of thousands uninsured, restrict the state’s ability to raise money, and shake the foundations of a robust social safety net.
 Koa Pea keeps a photo of herself sitting in a wheelchair in 2015 before her injuries.John Tlumacki/Globe Staff
Koa Pea keeps a photo of herself sitting in a wheelchair in 2015 before her injuries.John Tlumacki/Globe Staff
The decision to cut Medicaid spending will cost Massachusetts $3.5 billion a year by the 2030s and leaves the governor with choices that range from bad to terrible.
“We were faced with really difficult decisions,” said Becca Gutman, a PCA working group participant and vice president of home care for Local 1199 SEIU, which represents 58,000 PCA workers. “We recognized the difficult situation the state is in, and we approached it like we were trying to solve a problem.”
While the work groups give influence to people with a stake in service programs, they can also create tensions for members.
Fifty years ago, Charles Carr helped author the proposal that led to Massachusetts’ PCA program. Accustomed to fighting the state to fund services like the PCA program, he suddenly found himself participating in the work group and looking critically at his own brainchild.
“It was really awkward for me,” said Carr, a legislative liaison for the Disability Policy Consortium. One of the state’s most prominent disability rights advocates, Carr uses a wheelchair and relies on PCAs himself. “Here I am representing cuts to the program, and I’ve got a whole community of people I’m representing that don’t want to see the program cut at all.”
The group considered a range of budget-cutting options, such as eliminating overtime entirely. Another was to limit hours for so-called Instrumental Activities of Daily Living, such as house cleaning, food preparation, and bill paying, an option Carr said he fought hard to rule out.
“Where are people going to go to get these services done?” Carr recalled asking during discussions with working group members. “It got down to some heated discussions.”
The working group ultimately recommended reducing the overtime pay cap from 66 to 60 hours per worker and allowing no more than seven hours a week for meal preparation. The changes go into effect July 1.
Legislation in 2024 authorized the creation of a PCA working group well before Congress’s massive funding cuts, but unlike previous efforts to reduce PCA costs or introduce reforms, which fizzled in the face of advocacy from the state’s disabled community, these came with new urgency amid Congress’s cuts, Carr said.
“It made me realize we’ve got to seriously make some concessions,” he said.
The PCA cuts are a pittance compared to Massachusetts’ coming financial losses. Amid billions lost, MassHealth anticipates spending $6 million on new staff this year to manage increased administrative tasks.
The fact that a program for disabled and elderly residents is among the first to see cuts this year alarms some advocates, who worry the most vulnerable will disproportionately shoulder the pain.
“I don’t think this administration is committed to home, community-based services,” said Chris Hoeh, a disabled rights activist and PCA user. “They’re making a strategic choice to protect institutions over community-based capacity.”
State officials said they are looking everywhere for savings, including reviewing how hospitals bill Medicaid. The governor has also proposed a Medicaid rate freeze and ending coverage of GLP-1 drugs for weight loss, saving $15 million. But programs that provide long-term care for people outside of nursing homes, including the PCA program, are a big part of Medicaid’s growing cost, exceeding $3 billion a year.
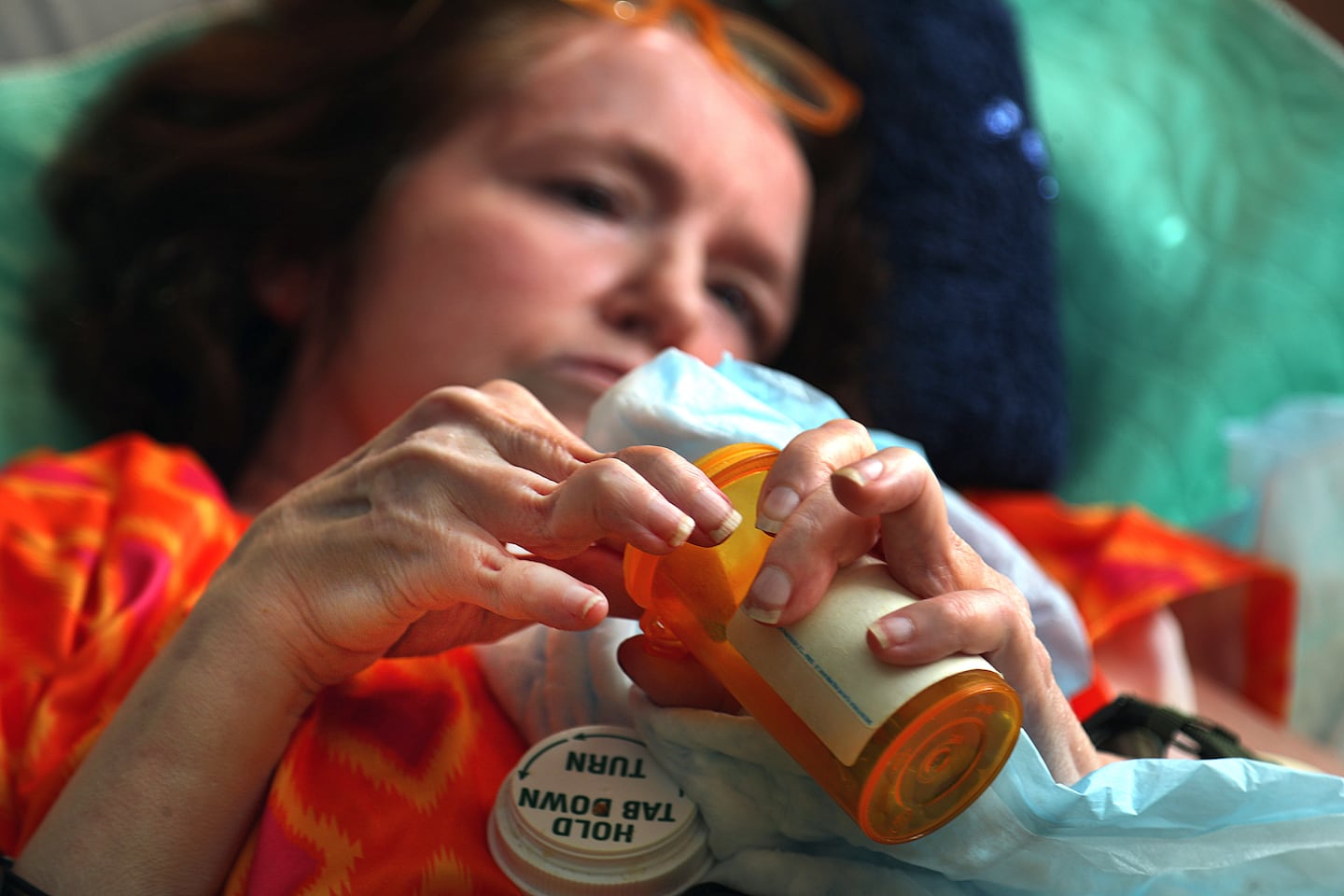 Pea took her 11 a.m. medications.John Tlumacki/Globe Staff
Pea took her 11 a.m. medications.John Tlumacki/Globe Staff Towels and laundry lines furniture to dry in Pea’s apartment left there by her personal care attendants on Feb. 13.John Tlumacki/Globe Staff
Towels and laundry lines furniture to dry in Pea’s apartment left there by her personal care attendants on Feb. 13.John Tlumacki/Globe Staff
“That has reached the big money category, I think,” Levine said.
Created in 1974 in response to conditions in state institutions, the PCA program gives people with significant disabilities the support needed to live independently. Users act as employers with control over who cares for them, when, and how. It also allows relatives to be compensated for caregiving.
The program’s growth has outpaced both inflation and the state’s increase in senior residents. Workers have negotiated for better wages, demand has increased as the state’s population ages, and people who need PCAs have tended to have more complex conditions.
Many PCA users said the program is the only thing keeping them out of a nursing home. Jonathan Gruber, an MIT economics professor who specializes in health care and consulted with the working group, said the state has an obligation to push back on assumptions about its programs. The role PCAs play in keeping people out of nursing homes hasn’t been well documented, he said, and it is worth looking at how services can be cut to ensure the most care for the most people.
“Now is the time to rethink what we spend our MassHealth dollars on, and to restructure those dollars toward what will do the most good,” he said.
Talk of hard decisions is terrifying for many PCA users.
Koa Pea, bedridden at her apartment in the West Fens because of a hip she broke a decade ago that she said can’t be treated, fears for her ability to stay home.
Pea, 62, born with cerebral palsy, owned a boat in Hawaii and taught elementary school in California. Now, her life is restricted to a small seventh-floor bedroom, where pictures of herself in the sun hang alongside notifications that she should not be resuscitated during a medical crisis.
She receives 45 hours of PCA care each week. Without it, she would be in a nursing home, where she fears she wouldn’t receive adequate care. Even confined to a bed, the freedom to stay at home is invaluable, she said.
“If I want to stay up all night until I can finish an audiobook, that’s my business,” she said.
Even the proposed changes have caused concerns. People already struggle to fill hours under existing overtime limits, said Sally English, chief executive for AdLib, a Berkshire County center for independent living that helps people coordinate PCA care. What lies ahead remains concerning, she sad.
“Because other programs that provide home care services are also being cut, I don’t know what people are going to do and where they’re going to go,” said English, who said AdLib works with 1,000 PCA users in Western Massachusetts.
The PCA working group, meanwhile, is still meeting, and may be asked to seek another $68 million reduction by 2027. Carr, the longtime disabled rights advocate, said there is a limit to the cuts he is willing to consider. Trimming another $68 million would “kill the program,” he said.
“If this escalates and the Legislature does decide to go with the $68 million, I’ll be in the street protesting,” he said.
Jason Laughlin can be reached at jason.laughlin@globe.com. Follow him @jasmlaughlin.

