In April 2020, people around the globe were struggling to come to grips with the strictures of unprecedented societal shutdowns aimed at slowing the spread of Covid-19. Flattening the curve, in 2020-speak.
Six years later, school and business closures, mask wearing, and social distancing are dim, unpleasant memories. And Covid, though it still animates political animus plenty, feels like a threat from yesteryear.
What’s happened here? Have humans and the SARS-CoV-2 virus, the cause of Covid, reached a detente? Does this virus that ended an estimated 15 million lives globally in 2020-2021 alone still pose a major hazard? After two consecutive winters when influenza, not Covid, was the bug sending hordes to their beds, is Covid now more nuisance than peril?
To help answer those questions, STAT asked a number of experts how they now think about the risk SARS-2 poses, and who they think should still be getting Covid booster shots. Most suggested we and the virus have changed so much in the years since SARS-2 first emerged that, for many people, it’s effectively become one of the panoply of respiratory viruses that can sicken us, like flu or RSV or the viruses that cause what we call the common cold. But for some individuals, it still represents a significant risk.
Here are their thoughts about the changing Covid landscape and what it means for you.
Virtually everyone has at least some immunity to the SARS-2 virus at this point
When Covid first started spreading among people, none of us had any immunity to this new virus, which allowed it to wreak havoc.
In the intervening years, the immune systems of virtually every human on the planet have developed some armor with which to fend off SARS-2, either because they have been previously infected or been vaccinated against the virus or both. The exception, of course, is babies in their first year or two of life.
There is an ever-shrinking portion of the population that thinks it’s never been infected — the folks who call themselves Novids. Even among that population, many have all but certainly been exposed to the virus but had only asymptomatic infections.

STAT Plus: mRNA Covid shots may boost the effects of certain cancer treatments, study suggests
This, many experts told STAT, explains why the threat from Covid has subsided.
Lia van der Hoek, a Dutch virologist who has been studying coronaviruses that infect humans — she discovered one of them, NL-63 — since before SARS-2 emerged, has a different view.
She has for years tracked how often a cohort of men in Amsterdam has been infected with common cold coronaviruses to map out how long immunity to them lasts. In the fall of 2020, she published a paper effectively warning that we shouldn’t expect full long-lasting immunity after Covid infection, because reinfection with the other human coronaviruses can happen within a year, sometimes sooner.
Today, Van der Hoek, director of the virus discovery group at Amsterdam University Medical Center, doesn’t buy the notion that immunity to SARS-2 is what’s behind the changed pattern of illness we’ve seen over the past couple of years.
She believes emergence of the Omicron variant in late 2021 turned the tide in the battle against SARS-2. Though more adept at evading the immunity people had developed, Omicron viruses caused much milder disease, she said.
The current circulating viruses are all descendants of Omicron.
Whatever the reason, the outcome is clear: Covid isn’t the risk it once was.
We’re seeing fewer severe illnesses and fewer deaths
In 2021, Covid was the third most common cause of death in people ages 18 and older in the United States, according to the Centers for Disease Control and Prevention. By 2023, it had dropped to the 10th spot. In 2024, the most recent year for which these data are available, Covid ranked as the 15th most common cause of death among American adults. (Influenza was the 11th that year.) For kids and teens, Covid fell out of the top 10 causes of death in 2023.
Fiona Havers, a medical epidemiologist who worked on Covid at the CDC before quitting the agency last year, believes that Covid does remain a threat, and perhaps at this point an underappreciated one.
Now an adjunct associate professor at Emory University, Havers said people who die from Covid will often have a vague condition of some kind listed on their death certificates. Pneumonia — an umbrella term for a syndrome caused by many pathogens — or respiratory failure or something like that. The same kind of nonspecific causes of death have long been listed on the death certificates of people who die when they have influenza. As a result, CDC scientists use mathematical modeling to gauge how many people probably died from conditions like flu and Covid.

The indirect — and sometimes surprising — benefits of vaccines
The CDC estimates that between Oct. 1, 2024, and Sept. 30, 2025, 45,000-64,000 Americans died from Covid infections. In the seven months since then, the estimated range is 13,000-40,000 deaths.
For context, there were slightly more than 100,000 estimated Covid deaths in the United States in both 2022-2023 and 2023-2024.
“Every single year since the pandemic, the overall severity and impact of Covid has been going down,” said Havers. “And this last year has had the least amount of severe disease that we’ve seen since Covid started circulating, since SARS-CoV-2 emerged. So that’s good news.”
Stanley Perlman, a microbiologist from the University of Iowa who like Van der Hoek has studied coronaviruses for many years, finds even the most recent numbers higher than he would have expected.
“If you go into a hospital … and go to the ICU, you’d probably find nobody who’s dying from SARS-CoV-2,” he said. “Are these people in nursing homes? I don’t know who these people are who are dying, but there seems to still be a slew of them.”
In addition to causing fewer deaths and fewer severe illnesses, there appears to be evidence that Covid may not be circulating at the levels it once was.
WastewaterSCAN, a research project led by scientists from Stanford and Emory universities, draws samples from municipal sewage facilities across the country to look for pathogens people shed through their stool. These days, they aren’t detecting a lot of SARS-2.
“The levels that we’re seeing in wastewater are the lowest that we’ve ever seen,” said Alexandria Boehm, WastewaterSCAN’s principal investigator and a professor of civil and environmental engineering at Stanford. That could be because fewer people are being infected, or because people infected are shedding less virus, she cautioned.
Boehm noted that in previous years there has been a summer surge of activity, which typically started to show up in wastewater testing in May and June. “So I guess we will have to see if that actually happens this year or not.”
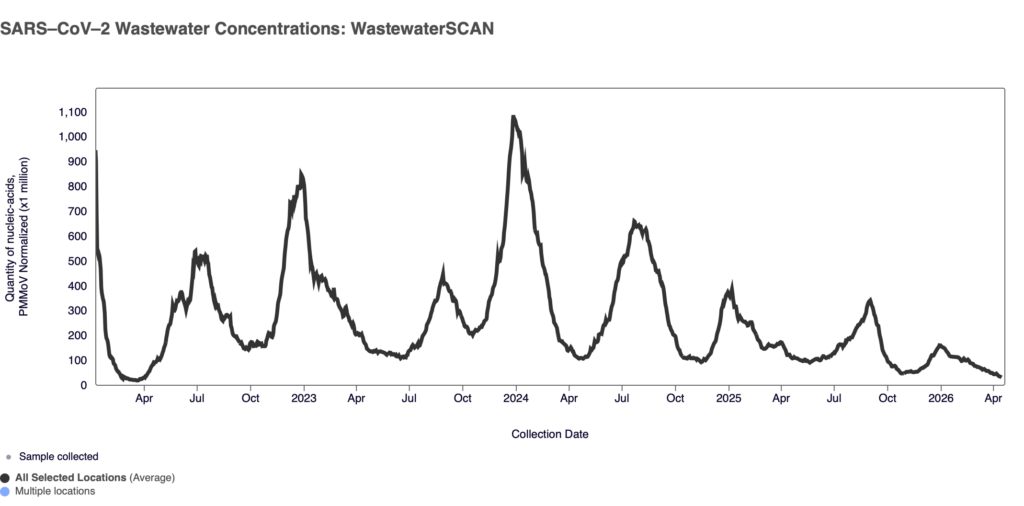 Covid wastewater concentrations from Jan. 8, 2022 through April 15, 2026.WastewaterSCAN
Covid wastewater concentrations from Jan. 8, 2022 through April 15, 2026.WastewaterSCAN
So — nuisance or peril?
Most of the experts STAT consulted believe the virus either now qualifies as, or is on its way to becoming, just another one of the viruses that make people sick with cold or flu-like symptoms — with some caveats. For one, the risk remains high for some people — particularly older people, very young children, and people with medical conditions that weaken their immune systems. For another, cold and flu-like viruses trigger symptoms that range from sniffles and coughs to knock-you-off-your-feet illness. A bad case of flu can take a couple of weeks to recover from, even for a healthy person. Same with Covid.
Malik Peiris, a professor emeritus of microbiology at the University of Hong Kong and one of the discoverers of two earlier coronaviruses, views SARS-2 now “as another seasonal respiratory virus.”
“While new and sometimes unexpected SARS-CoV-2 lineages will continue to emerge, the global population now has sufficient immunity that a variant causing major public health impact, i.e. severity, is unlikely, though not impossible,” he wrote in an email.
Vineet Menachery, a virologist at the Emory University Vaccine Center, agreed. “The patterns indicate that new strains are relatively more capable of overcoming our immune responses, but the infection outcomes are more mild,” he wrote in an email. “This trend puts them on par with the common cold [coronaviruses], which are generally more of a nuisance illness, but can exacerbate to more severe disease even in young/healthy populations.”
Ben Cowling, chair of epidemiology in Hong Kong University’s School of Public Health, isn’t convinced Covid is yet as minor a threat as the other coronaviruses that infect people. While he said it’s reasonable to think SARS-2 is on that trajectory, “I’m not sure if we’re there yet.”
That’s not the way Van der Hoek sees it. “It’s just number 5 of the common cold [coronaviruses],” she said. “And if it’s not as mild as it can be for the four seasonal coronaviruses … it will be there soon.”

Where the risk persists and the need for boosters remains
In the early days of the pandemic, Covid deaths occurred in people of all ages. Today the at-risk population has narrowed.
“One has to understand that Covid-19 is a mucosal infection that can invade in people who have poor immune responses,” said Stanley Plotkin, a legendary vaccinologist who helped develop rubella and rotavirus vaccines. “That means most healthy people can control the infection, but the very young and the very old may not.”
Havers said this is evident in the Covid hospitalization and death data.
“The pattern of who Covid is affecting severely has settled out, so it looks a lot more like all the other respiratory viruses, where we see the people at the extremes of age that are most vulnerable to severe disease,” she said.
Of course, severe disease and death are not the only risks associated with Covid infection. New cases of long Covid are still being reported, though the incidence has declined since the early days of the pandemic, a trend attributed in part to a perceived protective effect of Covid vaccination.
The frequency of other serious side effects has also declined — myocarditis or inflammation of the heart muscle, a condition reported most commonly in teenage boys, and multisystem inflammatory syndrome in children, or MIS-C, Havers said.
So what does this pattern tell us about who still ought to be getting Covid shots?
The CDC’s Advisory Committee on Immunization Practices was working on new Covid vaccine recommendations that were scheduled to come up for a vote at its June 2025 meeting, before it was disbanded by health secretary Robert F. Kennedy Jr., who appointed new members skeptical of the benefits of vaccines. The group was considering moving from a universal recommendation — where everyone 6 months and older was advised to get a Covid shot every year — to one where only older adults, very young children, and some immunocompromised individuals would be urged to get an annual shot, or more than one shot a year, for some very vulnerable people. Others would be told they could get one if they wished.
Multiple peer countries had already adopted some version of that approach to Covid vaccination.
The new ACIP voted last September to recommend that everyone 6 months and older could get a Covid shot if they wanted, after discussing it with their physicians.
Marion Koopmans, scientific director of the Pandemic and Disaster Preparedness Center at Erasmus University in Rotterdam, the Netherlands, said at this point, annual boosting is probably not doing much for people who aren’t at high risk.
“What we really would need is data on what the effect is of boosting on variant specific responses AND protection from disease over increasing intervals between boosters. That data is virtually impossible to get,” she wrote in an email. (Pfizer recently announced it had halted a clinical trial the Food and Drug Administration asked it to conduct in healthy adults aged 50 to 64, because it couldn’t recruit enough volunteers.)
But for high-risk individuals, Covid boosters still offered protection against becoming sick enough to require hospitalization, the latest study in the Netherlands concluded, Koopmans said.
The Washington Post reported last week that HHS has shelved a study CDC scientists were on the verge of publishing showing that this past winter the vaccines reduced the risk of needing emergency care or hospitalization for Covid by 50%.
Meanwhile, the public appears to have decided on its own that Covid boosters are not a priority. The CDC reports that in the 2025-2026 season, just 9.4% of children and teens, 17.5% of adults 18 and older, and 22.1% of adults 65 and older had received Covid boosters. More than twice as many adults 65 and older received annual flu shots.
Internationally, Covid booster rates have also plummeted. The World Health Organization reported late last year that 13% of older adults and 6% of health workers had a shot in 2024, with most of those doses administered in high-income countries. In low- and middle-income countries, rates of booster uptake had fallen below 1%, even among high-risk groups.
A further sign of the times: Gavi, the Vaccine Alliance, which helps lower-income countries purchase vaccines, discontinued its support for Covid vaccine purchases at the end of 2025.

