Design, sample and setting
A cross-sectional survey study was conducted among older patients hospitalized in the geriatric, cardiology, pneumology, endocrinology, orthopedics and traumatology wards of the University Hospital Leuven, a tertiary academic hospital in Belgium. Patients were eligible if they were aged 65 or older and had at least two chronic diseases (i.e., multimorbidity), as determined by hospital staff. They needed to be hospitalized on one of the study wards and discharged to their home environment, including assisted living. Patients were excluded if they had confusion, psychosis, or severe cognitive impairment, based on the clinical judgement of ward nurses at admission. Non-Dutch speaking patients and nursing home residents were also excluded.
The hospital was actively involved in the Integrated Care for Better Health’ (Integreo) project, a federal government initiative aimed at implementing integrated care principles within the Belgian healthcare system. The ultimate goal of Integreo is to advance the quadruple aim of healthcare: improving population health, enhancing patient experience, reducing costs, and supporting the well-being of healthcare providers12,18. To achieve this, the Belgian government defined 14 core components of integrated care to be implemented across 12 pilot regions. Local project teams were given the flexibility to define specific care goals and target populations, allowing integrated care to be tailored to the needs and priorities of their respective regions.
Zorgzaam Leuven and Verbonden in ZOHrg are two of the 12 ongoing pilot projects within Integreo. Zorgzaam Leuven covers the Leuven region, while Verbonden in ZOHrg operates in the Tienen region. Each project serves approximately 100,000 inhabitants and aims to drive sustainable change towards integrated care. The pilot phase of these integrated care projects (ICPs) ran from 2017 to 2022. Numerous care initiatives were developed and implemented during this period, many of which focused on improving transitional care for patients with chronic ilnesses. Further details on Zorgzaam Leuven and its transitional care actions, stakeholder experiences and perceptions and implementation factors, are described elsewhere19.
Variables
The following demographic variables were collected: gender, age, educational level (no education, primary school education, secondary school education or higher education), living situation (living alone or cohabiting) and monthly net pension. Patients’ postal codes were used to determine whether they resided within or outside an ICP region.
The following clinical variables were recorded: type of chronic conditions (via a multiple-choice question listing common chronic diseases), number of hospital admissions in the past 12 months, general assessment of mental health (i.e., self-rated Likert question on general mental/physical health with five answer options ranging from poor to excellent), functional status (via a multiple-choice question listing activities of daily life), presence or absence of social support, and existing professional support, including home nursing, general practitioner, physiotherapist or day care centre (measured as days per week or month). Additionally, the number of nights spent in the hospital and the medical specialty for which the patient was admitted were recorded.
The survey questionnaire included two outcome variables, i.e., HRQoL and patient experiences.
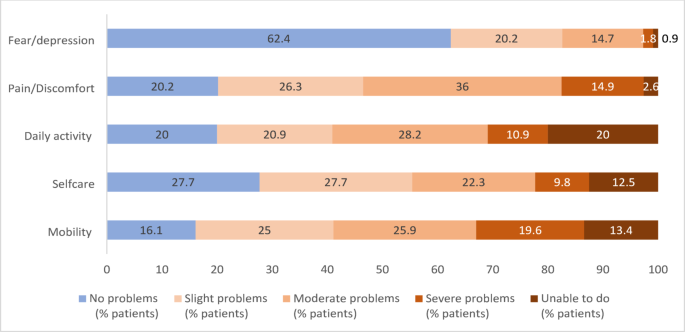
HRQoL was measured with the EQ-5D-5L (see Supplementary information 1), a validated instrument to measure the health status of the population, which can be used for a variety of health conditions and treatments15. The EQ-5D-5L includes five health dimensions (i.e., mobility, self-care, usual activities, pain/discomfort, anxiety/depression), which need to be rated as no problems, slight problems, moderate problems, severe problems, or extreme problems. This results in a score of 0 to 4 for each dimension and a total score of 0 to 20 for the scale, with a higher score indicating more severe problems. We calculated the EQ-5D utility score which represents a single number that reflects the overall quality of life associated with a specific health state, as perceived by the general Belgian population20. The score is anchored between 1 (representing full health) and 0 (representing a state as bad as being dead), with negative values indicating health states considered worse than dead. The EQ-5D-5 L questionnaire also includes a visual analogue scale where patients are asked to rate their health today on a scale of 0 (i.e., the worst health you can imagine) to 100 (i.e., the best health you can imagine).
Patient experiences were measured with the ‘Experiences with Hospital Care, Admission and Discharge’ instrument (see Supplementary Information 1). This questionnaire was originally developed by the Netherlands Institute for Healthcare Research (NIVEL) and was tested for validity, reliability and discriminating ability21. It is based on three existing questionnaires: the internationally used ‘Consumer Assessment of Healthcare Providers & Systems’ questionnaire on hospital care, the ‘Dutch Association of Hospitals’ questionnaire on ‘Satisfaction with Hospital Care’ and the NIVEL questionnaire ‘Consumer Association’s Hospital Comparison’21,22. The instrument assesses patient experiences throughout the care pathway, from hospital admission to discharge home. While it focuses primarily on in-hospital care, the components related to admission and discharge capture key aspects of care transition quality.
To ensure that the questionnaire captured relevant aspects of care transitions, certain elements from the original instrument were adapted by removing, rephrasing, or adding questions. Specifically, items not directly related to transitional care—such as those about room comfort, food, and the general inpatient environment—were removed. Additionally, some questions were slightly rephrased to align with the Belgian healthcare context and terminology (e.g., using the Flemish term for emergency department).
The questionnaire used in this study consists of 61 questions covering the following nine domains: accessibility of the hospital (3 questions), hospital admission (4 questions), admission conversation (12 questions), welcome at the ward (7 questions), care provided by nurses (8 questions), care provided by physicians (8 questions), communication about treatment (6 questions), feelings of safety (1 question), and hospital discharge (12 questions).
Finally, we added one multiple choice question asking patients to indicate the three elements they considered most important during their hospitalization.
Data collection procedure
The study was approved by the Research Ethics Committee of UZ/KU Leuven (file number S63948) and conducted in accordance with the Declaration of Helsinki and the principles of Good Clinical Practice. Written informed consent was waived by the Research Ethics Committee of UZ/KU Leuven as the study does not fall within the scope of the Law of 7 May 2004 related to experiments on human people.Data were collected between September 2020 and December 2021. Due to the COVID-19 pandemic and some wards temporarily being transformed to dedicated COVID wards, data collection was not continuous, as originally planned, but was paused at various points. Eligible patients received the survey upon hospital discharge from ward nurses, who also provided an orally explanation of the study’s aims and procedures. To support consistent inclusion, nurses received an information session on the data collection process and leaflets were distributed at the hospital wards for reference. The research team also visited the wards regularly to follow-up on the process and address any questions. Included patients were asked to fill out the paper questionnaire at home within 10 days after discharge and to return it to the research team via a prepaid envelope. The questionnaire included instructions for filling in and contact details of the research team in case questions occurred. No reminders were sent out, as no contact details were collected from the participants. The collected data were managed using REDCap software. Data entry was conducted by two student researchers, and quality checks were performed by a third researcher (ML).
Data analysis
Descriptive analysis of the demographic and clinical characteristics was performed for the total sample (see Table 1). To facilitate concise reporting of the data summaries, we regrouped most clinical and demographic variables into a maximum of two or three distinct categories. Additionally, for medical specialty data, we removed patients from the sample who selected multiple specialties, who answered ‘I don’t know’ or who did not answer.
Table 1 Description of the sample and comparison between those living within or outside an ICP region (n = 119).
Next, descriptive analysis of patient experiences and HRQoL was performed for the total sample without imputation of missing data. Responses for which the patient did not answer or selected the option ‘not applicable’ were classified as missing data and were excluded from the summary report. Additionally, for questions where a higher score indicated more problems or worse health, we reversed the scores in such a way that a higher score always indicated a better experience.
Patients living within and outside the ICP region were compared using the chi-square test to verify whether the groups were comparable in terms of their demographic and clinical characteristics.
Finally, the patient experience and HRQoL of patients living within and outside the ICP region were compared using independent sample t-tests to test for statistically significant differences in the mean score for each measure. To account for multiple testing, we applied the Bonferroni correction and considered a p-value of ≤ 0.005 to indicate statistical significance for the patient experiences measured in this study. IBM SPSS statistics 28 was used for the data analysis.