Thanksgiving is here—that magical week of joy, chaos, and family members who can somehow turn small talk into a UN summit.
Here are a few things that might help you survive the holiday: viral updates, food safety tips (yes, bird flu is hitting turkeys), navigating tricky conversations, and a poll for the most important debate of the season: store-bought or homemade cranberry sauce.
We also touch on the opioid settlement, which sends $7 billion to communities, the Department of Education removing public health degrees from “professional” status, and, as always, some great scientific news.
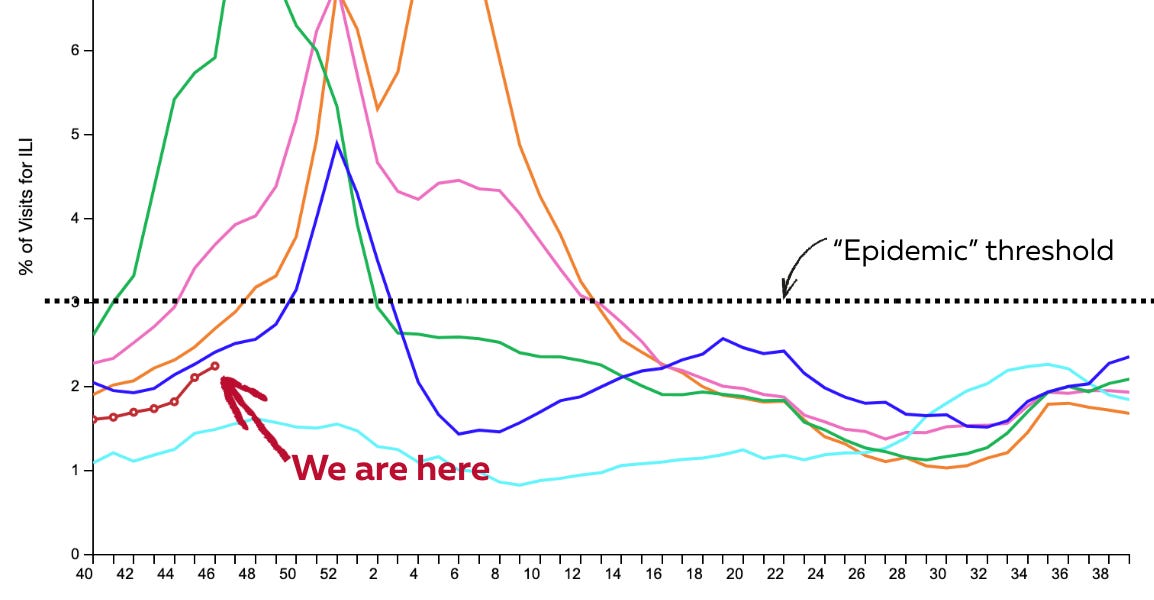
Colds, fevers, and coughs (also known as influenza-like illnesses, or ILI) are just getting started and haven’t reached the epidemic threshold. That’s great news heading into Thanksgiving, as there’s simply less circulating illness than in previous years, which means a lower chance of getting sick and fewer last-minute cancellations at your table.
 Source: CDC; Annotated by Your Local Epidemiologist
Source: CDC; Annotated by Your Local Epidemiologist
Covid-19 levels remain very low nationally. I expect activity to pick up soon and peak around January.
RSV is rising rapidly, so for infants, it’s best not to pass them from person to person during the holiday. If the mom got the RSV vaccine during pregnancy or the infant received the monoclonal antibody, they are incredibly well protected, and I wouldn’t think twice about it.
Norovirus—the nasty, highly contagious stomach bug that causes vomiting and diarrhea—is rising across all U.S. regions, with the South hit hardest. On average, one infected person can spread it to 2–7 others. It’s a common foodborne illness. So, if you have symptoms (or recently recovered, since you can still spread it for days after they fade), avoid preparing food or drinks for others. Wash your hands thoroughly (30 seconds with soap and water) and clean bathrooms frequently with bleach-based products. Hand sanitizer won’t work against this one.
 Source: NREVSS Enteric Dashboard
Source: NREVSS Enteric Dashboard
We often say “public health is everything”—and yes, that includes what happens around the Thanksgiving table. Here are a few public health tips.
Hard topics. You may not see eye to eye with relatives on what’s happening in the world (and there’s… a lot happening). Thinking Is Power shared eight tips for approaching conversations:
Never mock or judge. Defensiveness shuts things down.
Don’t make it personal. Address the belief, not the believer.
Find common ground. Shared values build connection.
Work together. Explore the idea collaboratively.
Ask, don’t tell. Curiosity opens dialogue.
Lead by example. Model the tone you want.
Focus on why, not what. How people form beliefs matters.
Know when to walk away.
If vaccines come up, keep these in your back pocket:
The vast majority of people (80-90%) support routine vaccinations.
Hesitancy is a spectrum. Only a tiny fraction are true deniers (e.g., those who believe vaccines contain 5G chips). Don’t assume the extreme if they have doubts or questions.
Separate Covid vaccine conversations from routine childhood vaccination conversations. There are a lot of feelings around Covid-19 vaccines that we don’t want bleeding into other vaccines.
Avoid the words “misinformation” or “mandate”—both trigger strong reactions for ~50% of the country. Try “falsehoods,” “rumors,” or “school requirements.”
Remember, you will not change someone’s mind in one conversation. The goal is to set new foundations of trust so they keep coming back with curiosity and being met with empathy.
Our friends at Unbiased Science put together a crash course on how to handle some of this year’s controversial topics (think seed oils, vaccines and autism, conspiracy theories.) Check it out here.
Food availability and safety. Bird flu (H5N1) has taken out nearly 2 million turkeys since September 1. While this happens every year—bird flu spreads two times faster in turkeys than in chickens—it has started earlier than expected. This shouldn’t impact supply.
Can you get bird flu from eating turkey? There have been no reported human cases of bird flu in the U.S. linked to handling raw food from the grocery store. Regardless, remember to cook turkey to an internal temperature of 165°F to kill bacteria and inactivate viruses.
Last week, a judge ruled that $7 billion from the Sackler family fortune will flow to communities across the nation to help fund solutions to the opioid crisis. The Sacklers, who owned Purdue Pharma, had aggressively marketed prescription opioids while denying their addictive properties to maximize profits. This decision represents justice that hits home for a lot of people who lost loved ones to this epidemic.
One of those families was in Marin County, CA, where Matt Willis—YLE correspondent—served as public health officer. Matt, take it from here:
During my first week as public health officer in Marin County in 2013, I met a father whose son died from an overdose of a prescription painkiller. The young man was at a party in his first year of college, took two pills, and never woke up. That conversation helped open my eyes to the local toll of this crisis. Working with other impacted families, we formed OD Free Marin, a county-wide initiative to tackle the opioid crisis.
Eight years later, I was invited to Washington, D.C. to share our local experience with federal judges deciding how opioid settlement dollars should be spent. I shared two perspectives: as a physician, I’d been trained to treat pain as “the fifth vital sign” and address it in every visit. With the whole medical community, I was misled by manufacturers like Purdue Pharma, that opioids were effective and non-addictive, if used as directed.
As a health officer, I saw how our community was fighting the opioid battle on multiple fronts—mental health and rehabilitation services, law enforcement, health care, schools—without enough resources to address the crisis these companies created. Communities like ours were sharing approaches, proving what was possible, but needed support to scale services to match overwhelming demand.
Purdue is one of many companies being held responsible for fueling this epidemic. So far, around $50 billion has been invested back into American communities through lawsuits against familiar names like CVS, Walgreens, and Johnson & Johnson—companies that manufactured, distributed, or dispensed these medications while the crisis escalated.
The judges decided that most funds should be allocated to state and local governments for evidence-based strategies: treatment for opioid use disorder, Narcan distribution, education campaigns, youth outreach, and rehabilitation services. Ensuring these funds end up supporting opioid mitigation, and not going to fill potholes or other government priorities, is another challenge. You can track spending here.
The money flowing from this decision will ideally help fund the kind of work we began in the wake of that young man’s death: preventing more losses, supporting those at risk, and building local infrastructure to fight this crisis on all fronts. It won’t bring him back—or the more than 1 million Americans who have died from overdose since 2000—but it’s placing accountability on an industry that knowingly put profits ahead of health.
Three pieces of great news this past week:
86 million girls vaccinated. Vaccine alliance Gavi announced that 86 million girls in high-risk countries have received the HPV vaccine, preventing an estimated 1.4 million deaths from cervical cancer.
Another mRNA win: better flu vaccines. Clinical trial data shows mRNA flu vaccine was 34.5% more effective than a licensed seasonal flu vaccine. Side effects were more common (e.g., fever: 5.6% vs 1.7%), but overall, this a major step forward toward better flu vaccines. The bigger question is whether people will accept mRNA platforms amid ongoing rumors and falsehoods.
Short workouts = big benefits. New research shows short bursts of vigorous exercise are incredibly efficient for heart health—6× more effective for preventing cardiovascular disease and 9× more effective for preventing diabetes than moderate activity. If vigorous activity isn’t your thing, moderate exercise is still great. The bottom line: move your body.
The government no longer considers MPH and DrPH (master of public health and doctor of public health) professional degrees. What does this mean for students and public health as a whole?
Last week, the Department of Education agreed on a draft definition of what counts as a “professional degree program” under the One Big Beautiful Bill. Several essential fields—public health, nursing, social work, physician assistant programs, and others—were removed from that list.
If this stands, students in these programs could lose access to federal financial aid. Specifically, lower borrowing limits, fewer scholarship pathways, and limited eligibility for loan-repayment programs. It will make it harder to enter these careers at the exact moment our country needs more of these professionals. The broader consequences are significant: fewer trained professionals, more barriers for students from low-income backgrounds, and added strain on already stretched health and social systems.
The Department of Education will release a formal proposal in the next few weeks, launching a 30-day public comment period. When that opens, I’ll make sure you know, because responses will matter.
That’s it for the week. YLE is closed until next week for the holiday and some much-needed unplugging. Grateful for all of YOU!
Love, YLE
Your Local Epidemiologist (YLE) is founded and operated by Dr. Katelyn Jetelina, MPH PhD—an epidemiologist, wife, and mom of two little girls. YLE is a public health newsletter that reaches over 400,000 people in more than 132 countries, with one goal: to translate the ever-evolving public health science so that people are well-equipped to make evidence-based decisions. This newsletter is free to everyone, thanks to the generous support of fellow YLE community members.