The number of hospitalizations Massachusetts has seen for septicemia has more than tripled since 2010, to more than 42,000 people in the year ending September 2025, preliminary state data show. Since at least 2019, it has been the third-leading cause of hospitalizations in Massachusetts.
Some of the uptick may be better recognition and diagnosing. But experts, insurers, and even some providers point to another explanation that is less about the actual medical threat and more a statement on modern health care: the increasingly sophisticated battle between hospitals and insurers over billing, each side using the power of artificial intelligence and other tech tools to protect their businesses.
Insurers say hospitals are billing for the most expensive conditions and highest severity that patients could conceivably have with their symptoms. Hospitals say they have to optimize billing to combat higher rates of denials from insurers. Regardless, experts say the practice is adding to health care costs while providing very little if any benefit to patients. On sepsis alone, the practice could add thousands of dollars to each bill hospitals submit.
“The way we pay for health care in the country creates a game, and people learn to play the game. The game has all to do with increasing revenue,” said Don Berwick, a former administrator of the Centers for Medicare and Medicaid Services and former president of the Institute for Healthcare Improvement. “But it’s gotten way out of control.”
Billing practices are a core contributor to both rising costs and wasteful spending in the health care sector, Berwick said. Insurers have cited more intense billing as one driver of spending, which contributes to ever escalating health insurance premiums that households, employers and even many towns are struggling to pay.
Insurers and some experts say hospitals are using tools and vendors to comb through medical records, submitting billing codes that make the patient look as sick as possible.
And, the sicker the patient, the higher the payment.
“Providers [are] coding differently to generate, ultimately, higher payments without any change in the quality of care being delivered,” said Michael Guerriere, chief actuary at Blue Cross Blue Shield of Massachusetts. “It’s just documentation.”
 Registered nurse Cristhel Morin cared for a patient in the COVID-19 intensive care unit at UMass Memorial Medical Center in 2021. Erin Clark/Globe Staff
Registered nurse Cristhel Morin cared for a patient in the COVID-19 intensive care unit at UMass Memorial Medical Center in 2021. Erin Clark/Globe Staff
Hospitals, for their part, say the size of the charges fully reflect the illnesses they treat and the care that is delivered; moreover, the tools that do this are necessary to capture as much revenue as possible in increasingly expensive operating environment, as well as to combat insurers’ growing use of AI to deny claims.
“The tension between payers and providers has never been higher and it’s likely to get much worse over several years,” said Dr. Eric Dickson, chief executive of UMass Memorial Health.
Facing budget shortfalls, UMass last year cut some services and faced off with Blue Cross over a new rates, risking the access of 200,000 patients to their doctors, before reaching an agreement.
“Why is this happening? Providers are losing money,” Dickson said, adding: ”When you start losing money, you are looking at any source of margin you can find to get back on track. One source is to make sure you are appropriately coding for everything you can.”
Many are quick to point out that the practice largely is not fraudulent. For example, take calcium levels. In the past, low levels in a patient might have just been something discussed and watched among clinicians. But with AI tools that record doctors’ visits or other technology that reviews those recordings and scours notes, that lab value can now be flagged as hypocalcemia for billing purposes, which increases the reimbursement.
Sometimes, even the order in which diagnoses are put on a claim can change a reimbursement. Though the underlying care sometimes hasn’t changed, the bill for the visit can stretch far higher.
Matthew Day, senior adviser at Blue Cross Blue Shield of Massachusetts, said septicemia is the most intense and expensive example — hospital cases with a septicemia diagnosis garner $10,000 more on average per claim than one for an infection alone.
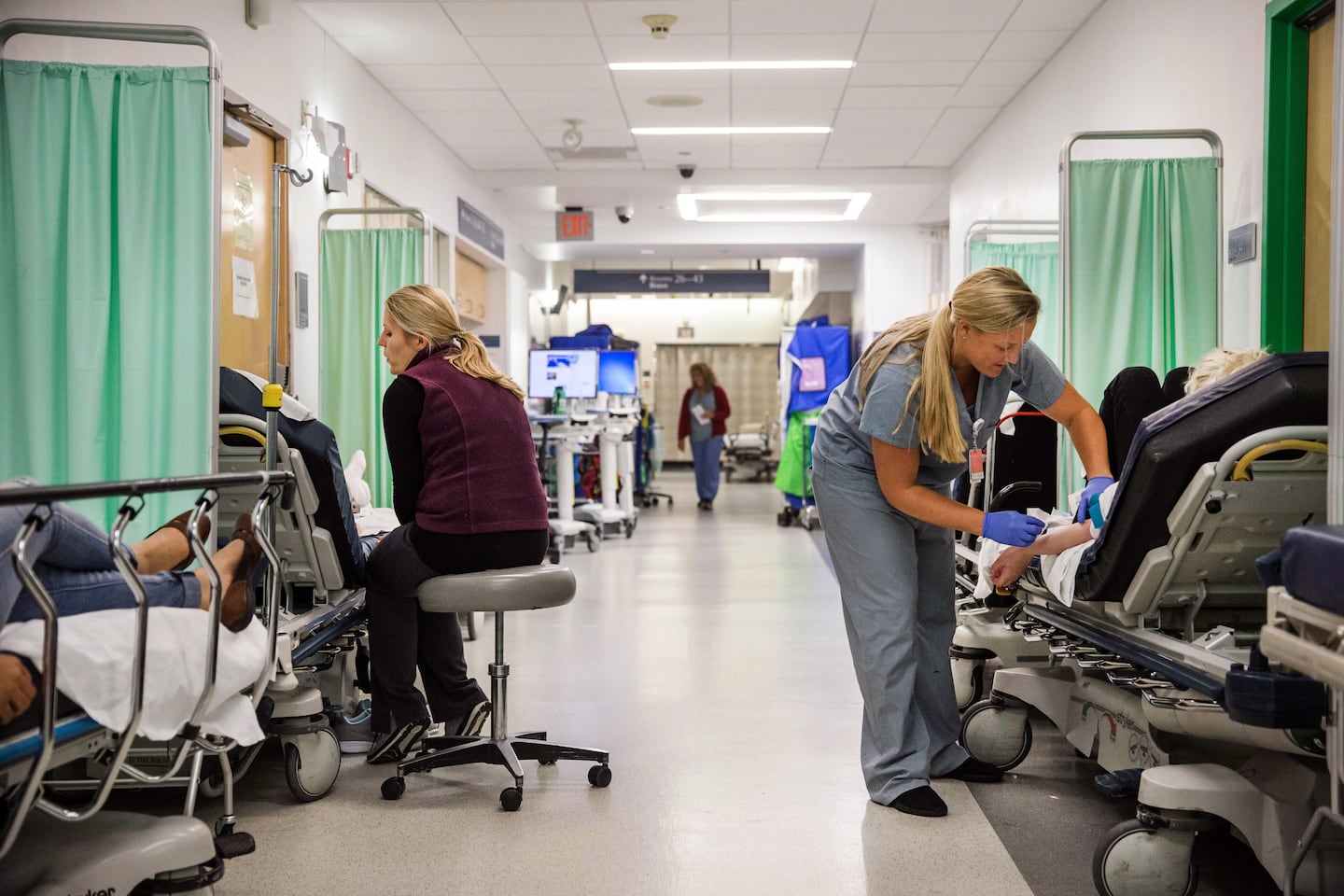 Patient beds lined a hallway in 2019 in the emergency department at Brigham and Women’s Hospital in Boston. Aram Boghosian for STAT
Patient beds lined a hallway in 2019 in the emergency department at Brigham and Women’s Hospital in Boston. Aram Boghosian for STAT
And, it isn’t just septicemia. Day said an analysis by Blue Cross revealed that patients with bronchitis or asthma are now being billed as having pulmonary edema or chronic obstructive pulmonary disease. C-section deliveries are now more frequently billed in conjunction with other complications, such as with posthemorraghic anemia — a serious condition that typically signals severe blood loss.
Commercial billing data of maternity admissions for a group of Blue Cross Blue Shield plans, compiled by their trade association, found the share of cases coded for acute posthemorrhagic anemia increased by more than one third, to 9.3 percent of all admissions, over a nearly three-year period ending in early 2025.
Despite the more serious diagnosis, patients didn’t receive more intensive services. Many flagged with the diagnosis did not receive blood transfusions; in fact, blood transfusion rates across the same period remained relatively flat.
The increase in coding for acute posthemorrhagic anemia alone at the analyzed hospitals added an estimated $22 million to the costs of maternity admissions for those Blue Cross insurers, according to the report.
If patients were fundamentally sicker than in the past, all hospitals would be billing for sicker patients uniformly. Instead, the higher reimbursements were occurring at hospital systems that have resources to invest in the new technology, Blue Cross executives said. Additionally, studies have also shown that for-profit hospitals have been quicker than nonprofits to adopt the most aggressive billing practices.
Health insurers are already feeling the effects of this more intense billing. The state’s largest insurer, Blue Cross Blue Shield of Massachusetts, reported a $380.5 million operating loss last year, and undertook a buyout and some staff reductions. According to the insurer, approximately one-third of its rising expenses were attributed to higher-intensity medical services. While a portion might be people needing more complex care or being treated at more expensive places, the insurer said some of the increase is simply due to billing practices — to the tune of tens of millions of dollars.
High volume of claims for cardiac conditions and sepsis also contributed to escalating spending at Point32Health, which similarly reported a $301 million operating loss last year and recently made layoffs.
While not the leading cause of escalating health care spending, billing practices are a “meaningful contributor,” Day said.
That trend scares insurers, who worry what will happen when all hospitals start using the technology, and for a broader array of diagnoses.
From a doctor’s perspective, the focus is on treatment of the patient, not how much each step generates in revenue, said Dr. Jeremy Faust, an emergency physician at Brigham and Women’s Hospital who has written about sepsis policy.
While coding experts within the hospital may ask doctors to record the visit in a way that maximizes the reimbursement, ultimately the hospital is being paid for care it has delivered, Faust said. For example, in the case of a patient with a rapid, irregular heartbeat, the doctor could either simply summarize the visit by noting the medications that were prescribed, or make more extensive notes reflecting the 35 minutes spent providing critical care to a patient in urgent need.
“In both cases, the patient got what they needed. In one case, the hospital got a bit more money. Am I wrong to document what I did?” Faust said.
But many patients are likely unaware this is going on. And, occasionally the coding practices can end up costing them as well.
 A room at the hospital then called Morton Hospital in 2015.Jonathan Wiggs
A room at the hospital then called Morton Hospital in 2015.Jonathan Wiggs
One executive in the health care industry recounted her own personal experience with more intensive billing of a long-standing medical condition. The executive, who asked for anonymity to avoid retribution, said she would typically be prescribed an inhaler and cough suppressant for a persistent cough and cold she would get most winters.
But then one year she tried to purchase long-term disability insurance and was denied: the insurer said her medical records had a diagnosis of chronic obstructive pulmonary disease, an inflammatory lung disease she had not been knowingly been diagnosed with.
She contested the diagnosis with her primary care physician, who agreed she didn’t have COPD. She suspects either a coding specialist or a technology tool that reviewed the recording of her doctor’s appointment classified her illness under the most severe diagnosis it could find.
Now, she refuses to have her medical visits recorded, but fears for other patients who do not know about this trend.
Still, there is some debate about whether the billing practices reflect other factors at play — such as whether the US population is fundamentally sicker.
Dr. Hemant Hora, vice president of medical affairs for Point32Health and a practicing physician, acknowledged that more intensive coding has contributed to high spending. But he also said bills are higher because patients are generally sicker and are getting more services.
A 2019 analysis by the Health Policy Commission, however, found some evidence that isn’t the case. For example, the analysis found a sharp rise in the most severe cases of chronic obstructive pulmonary disease. Though these patients were documented as sicker, their hospital stays were shorter and the need for intensive care had declined. Nonetheless, the increase in severity at the highest level effectively doubled the reimbursement for each admission.
Similar questions surround the rise of septicemia.
Dr. Chanu Rhee, director of the Center for Sepsis Epidemiology and Prevention Studies at the Harvard Pilgrim Health Care Institute, has spent more than a decade researching the national and global rise of sepsis. On the one hand, septicemia and sepsis are squishy diagnoses, without consistent definitions. Part of the increase is likely better recognition and awareness, which can lead to closer monitoring and faster medical responses.
But Rhee has also led studies that cast doubt on that as a sole explanation. While there are more claims for sepsis that suggest dramatic increases, Rhee said clinical data from electronic health records show the incidence of sepsis has been more stable.
“We’re not so much saying sepsis isn’t a problem. It’s a huge problem. We deal with it all the time in the hospital. It’s a major cause of morbidity and mortality,” Rhee said. “But in terms of understanding trends, it’s become pretty clear what we’re seeing is not a true ballooning of disease incidence, but better recognition, enhanced diagnosis, and also enhanced coding.”
Data from Massachusetts are also suggestive: There isn’t an increase in the lowest-severity cases, which would support the theory of recognition of fringe cases; it’s the highest-severity cases, which fetch more reimbursement dollars, that are growing.
Hospitals say the higher bills are partly a reflection of an aging, and sicker, population, but also that such billing practices have become a necessity. Denial of claims used to be less frequent. But a recent analysis from a state agency found that one in five claims submitted by providers to commercial health insurers in Massachusetts were denied.
The use of technology is helping insurers be more aggressive with claims. In fact, Blue Cross Blue Shield of Massachusetts said in October it would use computer algorithms to scrutinize doctors who routinely bill at the highest severity levels and could pay less than what was requested.
“I’d love to say, ‘We’re right and they are wrong,’” said Dickson, the UMass Memorial CEO. “But in many ways, we are both wrong. They are spending more money on denials and medical directives and challenging it. We spend money managing it. We are both equally adding administrative expense to health care. Ultimately, the patient hasn’t gotten anything better.”
Jessica Bartlett can be reached at jessica.bartlett@globe.com. Follow her @ByJessBartlett.