Katie Lester initially blamed her red, irritated eyes on spending too much time on her computer and phone.
But when a few days later they hadn’t improved, she went to her pharmacy and bought over-the-counter eye drops – these didn’t help.
‘My left eye became bloodshot and felt gritty,’ says Katie, 34, who works in HR.
As the days passed, she noticed she was becoming very sensitive to light.
Not wanting to make a fuss – and knowing that red eyes can be common – she persisted with the eye drops.
‘This went on for weeks, and my eyes looked awful,’ says Katie, who lives in Kent with her husband Danny, 34 and their dog, Apollo.
‘I was still able to work but it was incredibly irritating, and I had to keep taking screen breaks.’
Eventually, she made an appointment with an optician, who diagnosed a corneal ulcer: an open sore on the clear corneal dome on the front of the eye. If not treated promptly, it can lead to blindness.
The pain can also be excruciating, as the cornea has one of the highest density of nerve endings in the body.

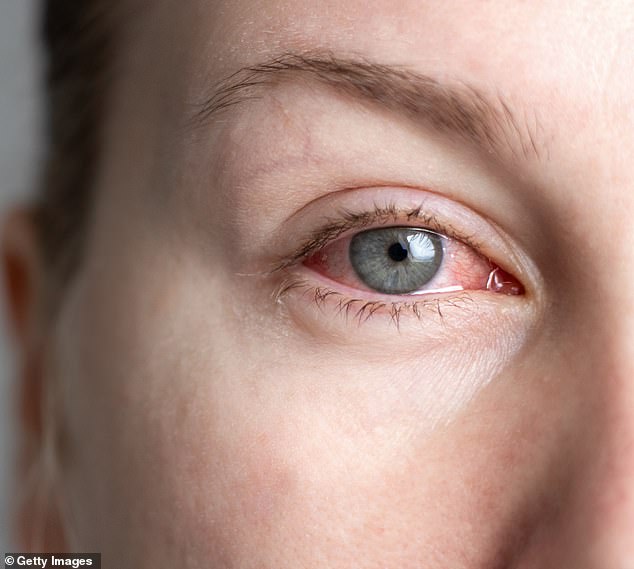
Katie Lister’s red and irritable eyes went on for weeks before she went to the opticians where she was told she had a corneal ulcer
‘I was shocked – and terrified,’ says Katie.
She was prescribed chloramphenicol ointment, the standard antibiotic treatment for an ulcer in the early stages. Yet over a year later, she now has to wear special goggles in windy weather – and even when opening the oven – to try and reduce the risk of developing another ulcer.
Corneal ulcers often start as a scratch or minor injury and then become infected by ‘opportunistic microorganisms such as bacteria, fungi and viruses’, says Jaclyn Pugh, an optometrist at The Optical People and Dry Eye Wales, a specialist dry eye clinic.
‘The longer ulcers are left to thrive on the cornea, the harder they become to treat.’
Severe untreated infections could lead to the cornea developing a hole and the infection can get inside the eyeball – which could lead to permanent loss of vision, warns Badrul Hussain, a consultant ophthalmic surgeon at Moorfields Eye Hospital.
Corneal ulcers can affect anyone but those most at risk include people who use reusable contact lenses, as these may harbour bacteria.
Open-water swimming and leaving lenses in as you sleep are also risk factors, as they all increase the chance of coming into contact with infection-triggering organisms.
Any contact lens wearer with a red, painful eye, accompanied by persistent light sensitivity, vision changes such as blurring, or seeing white ‘spots’ on the cornea should seek medical help immediately, says Mr Hussain.
‘As well as the eye becoming red, there is usually a foreign body/pricking sensation in the eye, watering, sensitivity to light and aching rather than just soreness of the eye.’
Infection isn’t the only cause – ulcers can also result from inflammation or severe dry eye or blepharitis, inflammation of the eyelids, that can also cause dryness and irritation on the surface of the eye – and it was this that Katie would learn had led to her ulcer.

Jaclyn Pugh, an optometrist, said ‘the longer ulcers are left to thrive on the cornea, the harder they become to treat’
Initially, Katie’s antibiotic ointment worked. But six weeks later she had another flare-up.
She returned to the optician – only to be told she now had corneal ulcers in both eyes.
That’s why, a few weeks later, in December 2024, she paid for an urgent private eye consultant and was told she had marginal keratitis – an inflammatory disease of the cornea, commonly associated with blepharitis.
In this case ‘bacteria that naturally live on the eyelids can get into the eye and via the cornea,’ explains Jaclyn Pugh, who says it’s normally treated with steroids to reduce inflammation, as well as antibiotics.
Red eyes can be an early warning sign of all sorts of conditions – some serious – and should not be ignored.
The redness is due to ‘inflammation which makes the blood vessels that are present on the surface of the eye bigger and more prominent,’ says Mr Hussain.
One of the most common causes is using screens too much because when we concentrate we blink significantly less frequently, meaning eyes miss out on lubricating tears which wash over the eye.
‘This causes our eyes to dry out in between blinks and then when we eventually blink, we blink on a poorly lubricated eye, which can cause red, sore eyes,’ says Jaclyn Pugh.
This, however, normally results in only transient discomfort.
Allergies such as hay fever are another cause of red eyes – but typically occur alongside itching (as the eye waters to try to dislodge the allergen).
Conjunctivitis, a bacterial or viral infection affecting the white of the eye can also cause redness – other signs include irritated, sore, weeping eyes. (This may require over-the-counter drops or cream.)
A burst blood vessel, alarming though it appears, is not usually a cause for concern, says Mr Hussain.
‘It can look worse than it actually is – as blood spreads easily on the transparent skin of the eye [conjunctiva],’ he explains.
‘It can happen very easily, such as as a result of vigorous coughing or sneezing, which puts pressure on the tiny blood vessels.’
But seek medical help if there is pain or vision changes with it, he adds.
Jaclyn Pugh says there are key steps you can take to protect against eye problems – such as selecting eyeliners with care.
‘These products are often oil-based and can seriously interfere with the meibomian glands [the glands in our eyelids which release the oils that help our eyelid slide over the eye on a blink].
‘They can block them, causing irritation and inflammation.’
That irritation can sometimes escalate into more serious issues, including conjunctivitis, corneal ulcers or even uveitis – inflammation deeper into the eye.
‘I currently have a 22-year-old under my care who has chronic conjunctivitis, after her eyes went into a downward spiral after using a new brand of eyeliner two years ago,’ adds Jaclyn Pugh.
‘It’s led to blocked and damaged meibomian glands, which then altered the entire make-up of the tear film. This led not only to severe discomfort, sensitive eyes and pain at times, but chronic conjunctivitis.’
Allergies such as hay fever are another cause of red eyes – but typically occur alongside itching
And Jaclyn Pugh warns: ‘Products we use to remove waterproof make-up also have a negative impact as they are often non-selective and remove everything from our eyes, including the healthy oils and naturally occurring protection our body produces.
‘I would advise regular use of products, such as hypochlorous acid – a gentle cleaning solution that helps keep the eyelids and lashes healthy. Your body actually makes it naturally, it’s part of how your immune system fights germs.’
Hypochlorous acid helps destroy viruses, fight fungi and calm inflammation.
‘It’s great for children, the elderly, contact lens wearers and everyone in between because we all want to keep the area around our eyes hygienic without harsh chemicals.’
She adds that one group who really should use it are those who wear false eyelashes, ‘as these can very quickly harbour nasties and hypochlorous is safe and effective in these people’.
Katie now uses special wipes ‘to clean my upper and lower lids twice a day to prevent any infections’, she says.
‘And I massage around my eyes to unclog the glands, encouraging eye oil-flow to help the eyes be less dry as a result of my blepharitis.’
Going out in the wind can dry and irritate them because it exacerbates the dryness, so she has to wear special moisture chamber glasses – rather like ski goggles.
‘I even wear them if I have to open the oven as the blast of hot air can irritate my eyes,’ she says.
‘It’s painful. When I have a flare-up, I have pain, severe sensitivity to light, red, watering eyes – and struggle with screen time even at the lowest brightness.
‘Holidays to dry, far-off exotic places are out of the question as the dry air can cause a flare-up.’
She adds: ‘I do still get ulcers and will get them for the rest of my life, as unfortunately this condition is not curable, it just has to be managed and treated when it flares-up.
‘I thought red eyes were common and nothing to worry about. In fact, they were a sign of something that could have led to me losing my sight – I’d advise anyone not to ignore them.’
